Chapter: Basic Radiology : Brain and Its Coverings
Exercise: White Matter Diseases
EXERCISE 12-7.
WHITE MATTER DISEASES
12-16. In Case 12-16, what is the most likely diagnosis (Figure
12-36 A, B)?
A.
Pseudotumor cerebri
B.
Metastatic disease
C.
Septic emboli
D.
Radiation necrosis
E.
Multiple sclerosis
12-17. In Case 12-17, what is most likely responsible for the
abnormalities seen on the MR image (Figure 12-37 A, B)?
A.
Cardiac arrhythmia
B.
Chronic hypertension
C.
Remote trauma
D.
Hepatic failure
E.
Carbon monoxide poisoning
Radiologic Findings
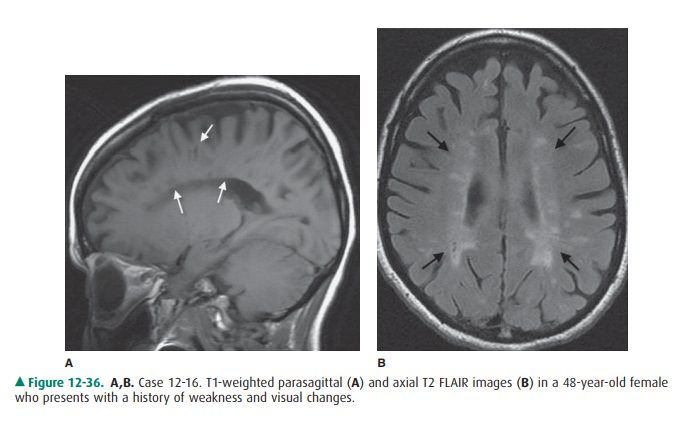
12-16. In this case, sagittal T1-weighted and axial FLAIR MR
images (Figure 12-36 A, B) show multiple foci of abnormal signal within the
periventricular white matter (arrows). These lesions are quite characteristic
of multiple sclerosis (E is the correct answer to Ques-tion 12-16). The
patient’s visual difficulties were due to optic neuritis, a common abnormality
in multiple sclerosis.
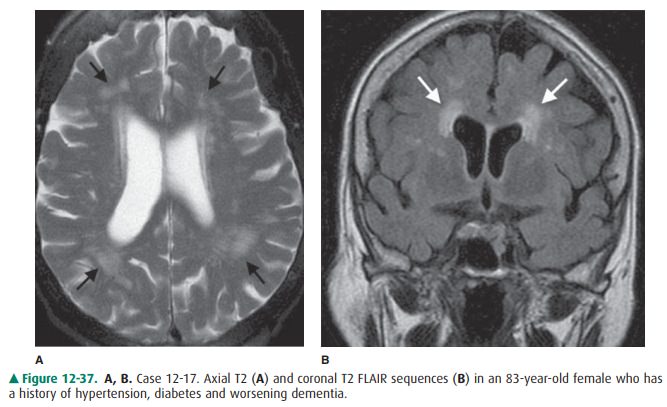
12-17. In this case, there are patchy areas of increased T2 sig-nal (arrows) within the periventricular white matter(Figure 12-37). Usually seen in elderly hypertensive patients, these lesions correspond to focal areas of de-myelination secondary to deep white matter ischemia (B is the correct answer to Question 12-17).
Discussion
Diseases that primarily affect
the cerebral white matter have a host of causes. Unfortunately, very few of
these conditions have specific appearances on CT or MR scans. Neuroimaging is
usually performed to determine whether there are changes within the brain that
are compatible with one of the white matter diseases and to rule out other
conditions that might mimic white matter disease.
White matter diseases include
both inherited and ac-quired conditions. They can be further subdivided into
de-myelinating conditions (destruction or injury of normally formed myelin) and
dysmyelinating conditions (abnormal formation or maintenance of myelin, usually
because of an enzyme deficiency). The dysmyelinating conditions are rare and,
for the most part, include the leukodystrophies, such as adrenoleukodystrophy
and metachromatic leukodystrophy. Although the MR appearance can be striking in
some of these diseases, it is often nonspecific. These conditions are not
dis-cussed here.
Multiple sclerosis (MS) (Case
12-16) is the most common demyelinating disease. Because there is no generally
accepted etiology for MS, it is also referred to as a primary demyelinat-ing
disease. Secondary demyelinating conditions are those caused by a known agent
or event. MS usually occurs in young adults and more often in women than men
(approxi-mately 2:1). The disease is characterized by a relapsing and remitting
course and by varying neurologic symptoms, de-pending on the location of the
lesion within the CNS. Al-though diagnosis of MS is usually based on clinical
criteria, MR imaging can be a very helpful confirmatory test. Typical MS
plaques appear as ovoid, T2 signal hyperintensities within the periventricular
and deep white matter. Lesions are also common within the corpus callosum,
brainstem, cere-bellar peduncles, spinal cord, and optic nerves. MS plaque
enhancement on gadolinium-infused MR images suggests active disease (ie,
breakdown of the BBB). Confluent areas of T2 signal abnormality in the
periventricular white matter are common in severe cases.
Ischemic demyelination (Case
12-17) is usually seen in patients with small-vessel disease (such as from
long-stand-ing hypertension). This condition, also called leukoaraiosis (white
matter softening), occurs because of hypertension-in-duced arteriolar sclerosis
of penetrating medullary arteries that supply the deep white matter of the
brain. This leads to a reduction in white matter blood flow with accompanying
is-chemic demyelination. This condition occurs most com-monly in older patients
and is associated with small-vessel brain infarcts (lacunar infarcts). MR
imaging usually demon-strates patchy areas of increased T2 signal in the deep
white matter. The lesions are often bilaterally symmetric and periventricular
in distribution.
Related Topics