Chapter: Pharmaceutical Biotechnology: Fundamentals and Applications : Gene Therapy
Ex Vivo Versus In Vivo Gene Therapy
EX VIVO VERSUS IN VIVO GENE THERAPY
Gene therapy is a means of treatment for diseases that have limited or
no therapeutic options. Once a disease has been identified as a possible
candidate, the gene necessary for treatment must be identified and cloned.
Enough must be understood about the disease and the gene product in order to
ensure that the therapeutic component is delivered to the appropriate cellular
compartment responsible for its processing and sub-sequent biological activity.
The necessity for long-term gene expression or requirements that expression be
timed with other biological processes will influence the design of the vector
component of the therapy. The target tissue/organ must be readily accessible
and a defined, measurable endpoint must be identified for assessment of
therapeutic efficacy. Several strategies can be used for gene transfer. Direct
injection of vector/ DNA complexes into the bloodstream is often char-acterized
by low levels of gene expression, making large amounts of vector necessary for
therapeutic efficacy. Broad distribution of the vector may adversely affect the
function and health of normal tissues and cause adverse reactions. This method
also has limited utility for the treatment of tissues with restricted blood
supplies such as muscle and tumors. Other delivery methods employed for in vivo
gene transfer include intratumoral, intraperitoneal subcutaneous, and
intra-muscular injection. These are crude, invasive and, in some cases, require
specialized surgical skills, making efficient tissue-targeted delivery systems
essential for successful gene transfer.
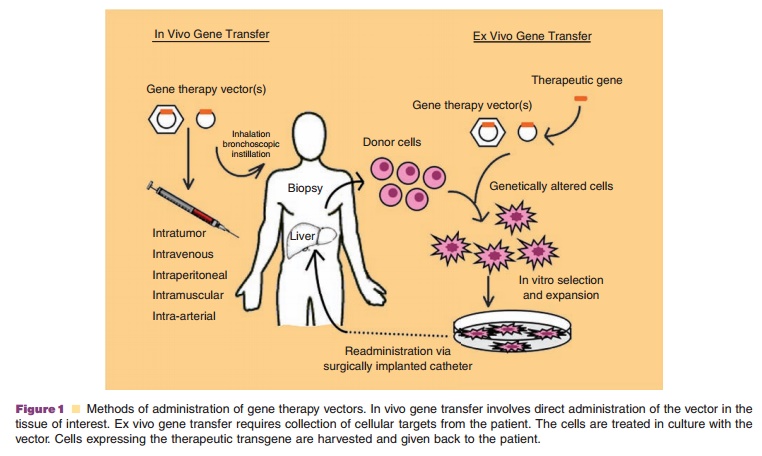
Ex vivo gene transfer strategies involve isolation and culture of
cellular targets. Gene transfer is achieved by direct application of the vector
(virus, plasmid) for efficient gene expression (Fig. 1). Cells are then studied
after treatment and only healthy cells expressing the therapeutic gene
collected and given to the patient. Initially, this approach was limited to
disorders in which the relevant cell population (i.e., bone marrow,
hepatocytes) could be removed from the affected individual, modified and then
replaced. Today, cells can be administered by local or systemic injection,
delivered in encapsulated form or as tissues comprised of cells seeded on
scaffolds. Patient safety is often improved with ex vivo gene transfer since
the host immune response to the vector or toxic effects associated with
transfection reagents are eliminated.
Related Topics