Chapter: Medical Physiology: Secretory Functions of the Alimentary Tract
Characteristics of the Gastric Secretions
Gastric Secretion
Characteristics of the Gastric Secretions
In addition to mucus-secreting cells that line the entire surface of the stomach, the stomach mucosa has two important types of tubular glands: oxyntic glands (also called gastricglands) and pyloric glands. The oxyntic (acid-forming) glands secrete hydrochloric acid, pepsinogen, intrinsic factor, and mucus. The pyloricglands secrete mainly mucus for protection of the pyloric mucosa from the stomach acid. They also secrete the hormone gastrin.
The oxyntic glands are located on the inside surfaces of the body and fundus of the stomach, constituting the proximal 80 per cent of the stomach. The pyloric glands are located in the antral portion of the stomach, the distal 20 per cent of the stomach.
Secretions from the Oxyntic (Gastric) Glands
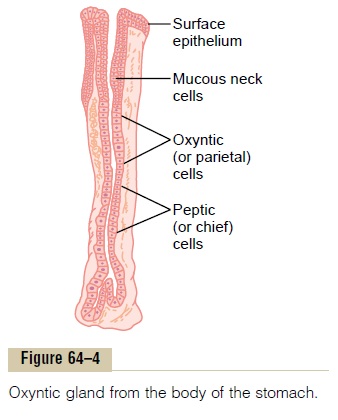
A typical stomach oxyntic gland is shown in Figure 64–4. It is composed of three types of cells: (1) mucousneck cells, which secrete mainly mucus; (2) peptic (or chief) cells, which secrete large quantities of pepsinogen; and (3) parietal (or oxyntic) cells, whichsecrete hydrochloric acid and intrinsic factor. Secretion of hydrochloric acid by the parietal cells involves special mechanisms, as follows.
Basic Mechanism of Hydrochloric Acid Secretion. Whenstimulated, the parietal cells secrete an acid solution that contains about 160 millimoles of hydrochloric acid per liter, which is almost exactly isotonic with the body fluids. The pH of this acid is about 0.8, demonstrating its extreme acidity. At this pH, the hydrogen ion con-centration is about 3 million times that of the arterial blood. To concentrate the hydrogen ions this tre-mendous amount requires more than 1500 calories of energy per liter of gastric juice.
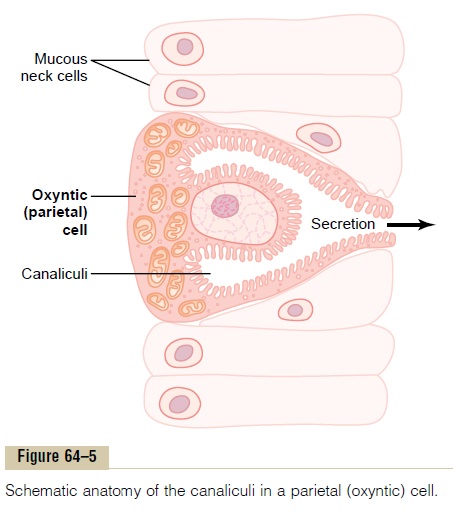
Figure 64–5 shows schematically the functional structure of a parietal cell (also called oxyntic cell), demonstrating that it contains large branching intra-cellular canaliculi. The hydrochloric acid is formed at the villus-like projections inside these canaliculi and is then conducted through the canaliculi to the secretory end of the cell.
Different suggestions for the chemical mechanism of hydrochloric acid formation have been offered. One of these, shown in Figure 64–6, consists of the following steps:
1. Chloride ion is actively transported from the cytoplasm of the parietal cell into the lumen of the canaliculus, and sodium ions are actively transported out of the canaliculus into the cytoplasm of the parietal cell. These two effects together create a negative potential of -40 to -70 millivolts in the canaliculus, which in turn causes diffusion of positively charged potassium ions and a small number of sodium ions from the cell cytoplasm into the canaliculus. Thus, in effect, mainly potassium chloride and much smaller amounts of sodium chloride enter the canaliculus.
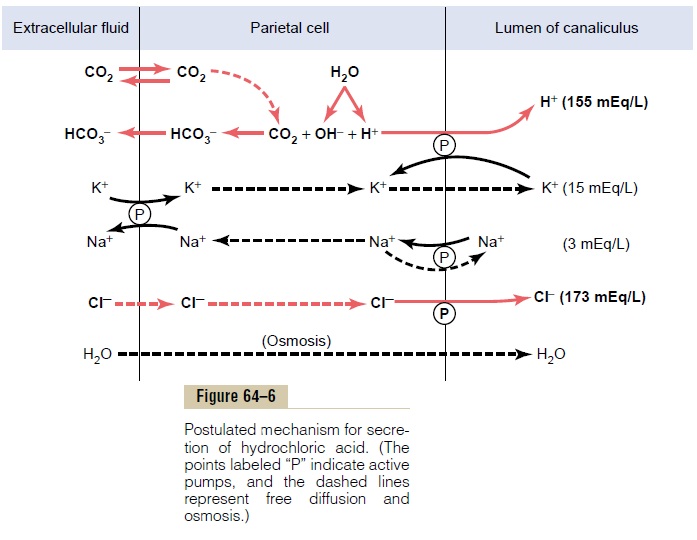
2. Water becomes dissociated into hydrogen ions and hydroxyl ions in the cell cytoplasm. The hydrogen ions are then actively secreted into the canaliculus in exchange for potassium ions: this active exchange process is catalyzed by H+,K+-ATPase. In addition, the sodium ions are actively reabsorbed by a separate sodium pump. Thus, most of the potassium and sodium ions that had diffused into the canaliculus are reabsorbed into the cell cytoplasm, and hydrogen ions take their place in the canaliculus, giving a strong solution of hydrochloric acid in the canaliculus. The hydrochloric acid is then secreted outward through the open end of the canaliculus into the lumen of the gland.
3. Water passes into the canaliculus by osmosis because of extra ions secreted into the canaliculus. Thus, the final secretion from the canaliculus contains water, hydrochloric acid at a concentration of about 150 to 160 mEq/L, potassium chloride at a concentration of 15 mEq/ L, and a small amount of sodium chloride.
4. Finally, carbon dioxide, either formed during metabolism in the cell or entering the cell from the blood, combines under the influence of carbonic anhydrase with the hydroxyl ions (from step 2) to form bicarbonate ions. These then diffuse out of the cell cytoplasm into the extracellular fluid in exchange for chloride ions that enter the cell from the extracellular fluid and are later secreted into the canaliculus.
Secretion and Activation of Pepsinogen. Several slightlydifferent types of pepsinogen are secreted by the peptic and mucous cells of the gastric glands. Even so, all the pepsinogens perform the same functions.
When pepsinogen is first secreted, it has no diges-tive activity. However, as soon as it comes in contact with hydrochloric acid, it is activated to form active pepsin. In this process, the pepsinogen molecule,having a molecular weight of about 42,500, is split to form a pepsin molecule, having a molecular weight of about 35,000.
Pepsin functions as an active proteolytic enzyme in a highly acid medium (optimum pH 1.8 to 3.5), but above a pH of about 5 it has almost no proteolytic activity and becomes completely inactivated in a short time. Hydrochloric acid is as necessary as pepsin for protein digestion in the stomach;
Secretion of Intrinsic Factor. The substanceintrinsic factor,essential for absorption of vitamin B12 in the ileum, is secreted by the parietal cells along with the secretion of hydrochloric acid. When the acid-producing parietal cells of the stomach are destroyed, which frequently occurs in chronic gastritis, the person develops not only achlorhydria (lack of stomach acid secretion) but oftenalso pernicious anemia because of failure of maturation of the red blood cells in the absence of vitamin B12 stim-ulation of the bone marrow.
Related Topics