Chapter: Case Study in Obstetrics and Gynaecology: Early Pregnancy
Case Study Reports: Bleeding in Early Pregnancy
BLEEDING IN EARLY PREGNANCY
History
A
31-year-old woman presents
with vaginal bleeding
at 5 weeks 6 days’ gestation. She has
had a previous left uterine
tubal ectopic pregnancy managed with laparoscopic sal- pingectomy. She is certain of her last menstrual period
date and has regular cycles.
Her last smear test
was normal and
she has not
used contraception since
her last pregnancy 3 years ago.
When she was 21 years she had an episode
of pelvic inflammatory disease treated with intravenous antibiotics. She is otherwise not
aware of having
had any sexually transmit- ted infections. She has been with her partner for 7 years.
She smokes 10 cigarettes per day and does not drink
alcohol. The bleeding
is described as very light
and she has not been aware of any pain.
She has not
felt dizzy or lightheaded and
has no shoulder-tip pain.
Examination
She
is warm and well perfused.
The blood pressure
is 136/78 mmHg and heart rate 75/min. The abdomen is not distended and no tenderness is elicited on palpation. The cervix is closed. The uterus feels
normal size, anteverted and mobile, and there is no cervical
exci- tation. Gentle adnexal
examination shows no significant tenderness.
Questions
·
What is the diagnosis?
·
What management options are
available and which management would be pre-
ferred in this particular case?
ANSWER
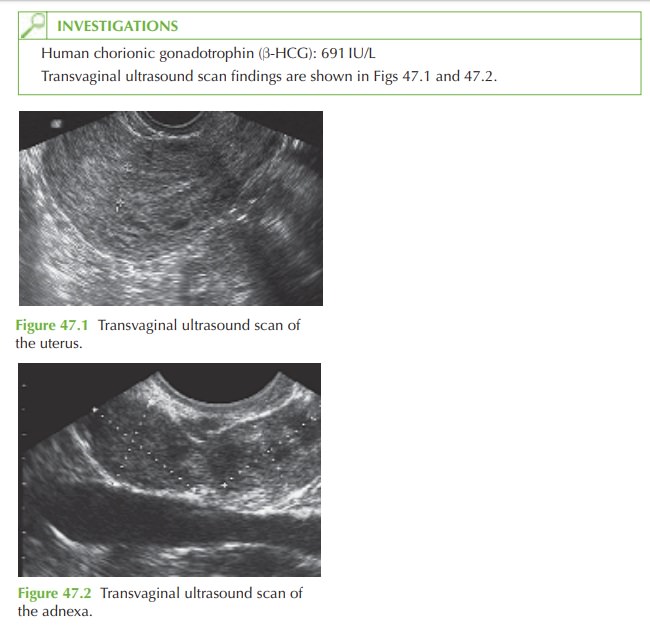
The
ultrasound scan shows
an empty uterus
and an adnexal mass adjacent
to the right ovary. The mass represents an ectopic pregnancy. No gestation sac or fetal
pole is visible and the pregnancy is therefore not considered ‘viable’. However
there is still
a possibility of rupture if
not treated.

Management
Three options might be appropriate to this woman:
·
surgical: laparoscopic excision of the tube (salpingectomy) or salpingotomy to incise
the tube and flush out the ectopic
pregnancy
·
medical: intramuscular methotrexate to destroy the
rapidly dividing trophoblast tissue, with regular HCG follow-up to confirm resolution
·
expectant: ‘wait and see’ approach,
suitable if the HCG at 48 h is decreasing spontaneously and the woman
remains asymptomatic.
In
this case the woman has previously had a uterine
tube removed and surgery might compromise the remaining tube,
so methotrexate treatment is preferred. However
if the tube is damaged but preserved, she may be at high risk of further ectopic
pregnancy. Prerequisites for methotrexate are normal full
blood count, renal
and liver function before treatment, compliance with the intense follow-up, and
understanding the need not to
become pregnant again
for at least 3 months
due to the potential teratogenic effects. Potential side-effects are abdominal pain (sometimes difficult to distinguish from pain
suggestive of tubal rupture), nausea, diarrhoea and, rarely, conjunctivitis and stomatitis.
Related Topics
