Chapter: Medical Electronics : Bio-Chemical and Non Electrical Parameter Measurement
Blood Pressure
BLOOD PRESSURE
One of
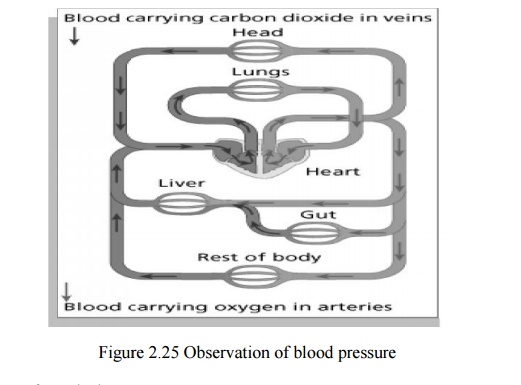
the oldest physiological measurements.Observation of blood pressure allows
dynamic tracking of pathology and physiology affecting to the cardiovascular
system, which has profound effects to all other organs of the body
·
Originates from the heart
·
Commonly refers to arter ial blood pressure
Value depends on 3 factors:
·
cardiac output diameter o f arteries the quantity
of blood
·
Values should be lower than 120 / 80 mmHg(systolic
pressure (SP) / diastolic pressure (DP))
·
High
value increases the risk of heart attack and strokes
·
Low value
increases
the r isk of lower oxygen perfusion e.g. in brains.
However,
the ’normal values’ differ from person to another
Pulse
Pressure(PP ) = SP - DP
Mean pressure (MP)
Average
pressure during one cardiac cycle driving force of the periph eral perfusion.
an estimate can be done by using an empirical formula:
M P =
DP+PP/3
SP and DP
may vary significan tly throughout the arterial system but MP is quite uniform
(in normal situations)
1. Non-Invasive
Palpatory
Method(Riva- Rocci Method)
Auscultatory
Method
Ultrasonic
Method
Oscillometric
Method
Tonometry
2. Invasive
Extravascular
Sensor
Intravascular
Sensor
General
on System Para meters
1. INDIRECT METHODS IN BLOOD
PRESSURE MEASUREMENTS
Indirect measurement = non-invasive measurement
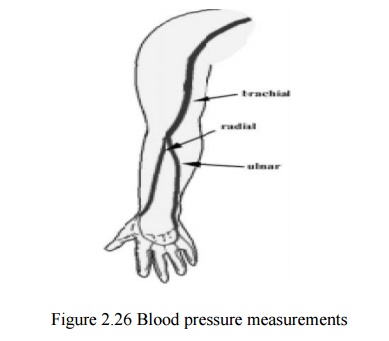
Brachial artery is the most comm on measurement site
Close to heart
Convenient measurement
Other sites are e.g.:
forearm / radial artery wrist (tends to give much higher SP)
The most
common indirect methods are auscultation and oscillometry an occlusive cuff is
placed on arm and inflated to P > SP. Then the cuff is deflated gradually
and the measurement of blood flow is done .
The
occlusive cuff should be of a correct size in order to transmit the pressure to
the artery evenly and thus to obtain accurate results .A short cuff requires
special attention in placement. Longercuff reduces this problem. The cuff
should be placed at the heart level in order to minimize the hydrostatic effects .
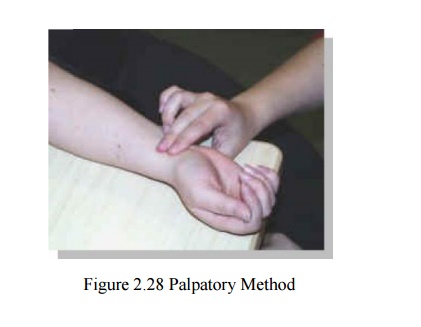
1.1 PALPATORY METHOD (RIVA-ROCCI METHOD)
When the
cuff is deflated, there is a palpable pulse in the wrist. P = BP .Several
measurements should be done as the respiration and vasomotor waves modulate the
blood pressure levels
Advantages
The blood
pressure can be measured in noisy environment too
Technique
does not requi re much equipment
Disadvantages
Only the
systolic pressur e can be measured (not DP)
The
technique does not give accurate results for infants and hypotensive patients
1.2 AUSCULTATORY METHOD
Pulse
waves that propag ate through the brachial artery, generate Kor otkoff sounds.
There are 5 distinct phases in the Korotkoff sounds, which define SP and DP The
Korotkoff sounds are ausculted with a stethoscope or microphone (automatic
measurement
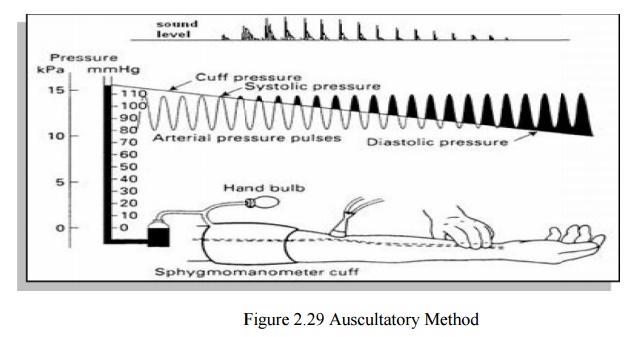
The
frequency range is 20-300 Hz and the accuracy is +/- 2mmHg (SP) and +/- 4mmHg
(DP). Also with this method, several m easurements should be done.
Advantages
Auscultatory
technique iss simple and does not require much equipmen t
Disadvantages
Auscultatory
tecnique ca nnot be used in noisy environment The observations differ f rom
observer to another
A
mechanical error might be introduced into the system e.g. mercury leakage, air
leakage, obstruction in the cuff etc.
The
observations do not always correspond with intra-arterial pressure
The
technique does not give accurate results for infants and hypotensive patients
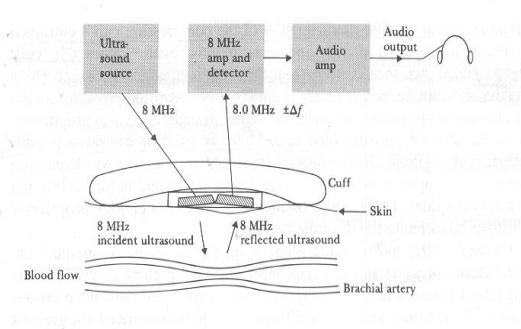
1.3 ULTRASONIC MET HOD
A
transcutaneous (through the skin) Doppler sensor is applied here. T he motion
of blood-vessel walls in various states of occlusion is measured. The vessel
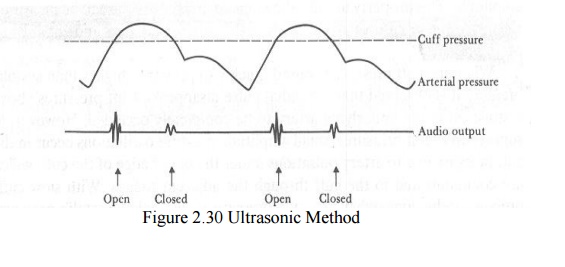
opens and closes with each heartbeat when DP < P < SP .
The
frequency difference between transmitted (8 MHz) and received signal is 40-500
Hz and it is proportional to velocities of the wall motion and the blood. As
the cuff pressure is increased, the time between opening and closing decreases
until they coincide.
Advantages & Disadvantages
Can be
also used in noisy environment
Can be
used with infants and hypotensive individuals
Subject’s
movements change the path from sensor to vessel
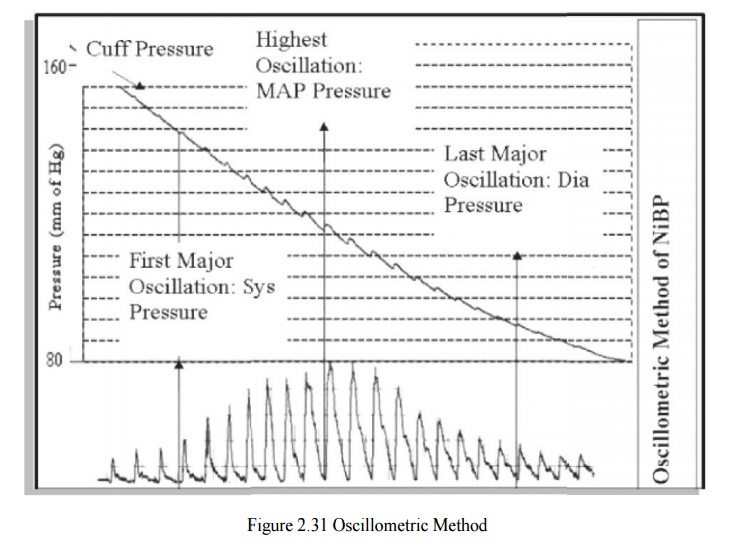
1.4 OSCILLOMETRIC METHOD
The
intra-arterial pulsation is transmitted via cuff to transducer (e.g.
piezo-electric) .The cuff pressure is deflated either linearly or stepwise. The
arterial pressure oscillations (which can be detected throughout the
measurement i.e. when P > SP and P < DP) are superimposed on the cuff
pressure SP and DP are estimated from the amplitudes of the oscillation by
using a (proprietary) empirical algorithm .
Advantages
In the
recent years, oscillometric methods have become popular for their simplicity
of use and reliability.
MP can be
measured reliably even in the case of hypotension
Disadvantage
Many
devices use fixed algorithms leading to large variance in blood pressures
1.5 TONOMETRY
Linear
array of pressure sensors is pressed against a superficial artery, which is
supported from below by a bone (radial artery). A sensor array is used here,
because at least one of the pressure sensors must lay directly above the
artery .When the blood vessel is partly collapsed, the surrounding pressure
equals the artery pressure
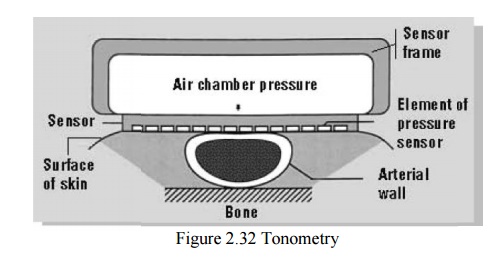
The
pressure is increased continuously and the measurements are ma de when the
artery is half collapsed. The hold-down pressure varies between individuals and
therefore a ’calibration’
must be
done
Advantages
Can be
used for non-inv asive, non-painful, continuous measurement
Disadvantages
Relatively
high cost
The wrist
movement and tendons result in measurement inaccuracies
2. DIRECT METHODS INN BLOOD
PRESSURE MEASUREMENTS
Direct
measurement = Invasive measurement
A vessel
is punctured an d a catheter (a flexible tube) is guided in The most common
sites are brachial and radial arteries but also other sites can be used e.g.
femoral artery A division is made into extravascular and intr avascular sensor
systems .This method is precise but it is also a complex procedure involving
many risks Used only when essential to determine the blood pressure
continuously and accurately in dynamic circumstances
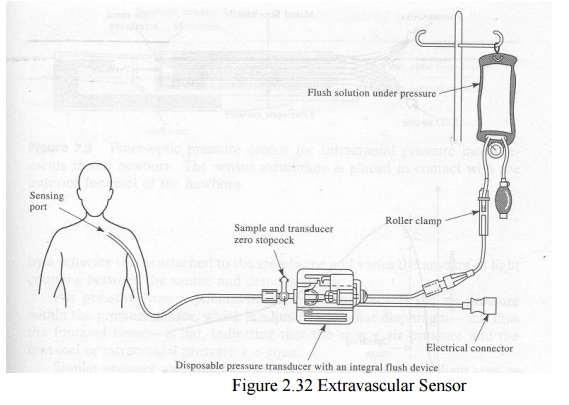
2.1 EXTRAVASCULAR SENSOR
The
sensor is located be hind the catheter and the vascular pressure is transmitted
via this liquid-filled catheter.
The
actual pressure sensor can be e.g. strain gage, variable inductance,variable
capacitance Optoelectronic, piezoelectric, etc…
The
hydraylic link is the major source of errors. The system’s natural frequency
may be damped and degraded due (e.g.):
too
narrow catheter too long tubing
various
narrow connections air bubbles in the catheter
The
catheter-sensor system mus t be flushed with saline-heparine solution every few
minutes in order to prevent blood from clotting at the tip.
Normally
the interesting frequency range is 0 – 100 Hz. If only MP is measured the
bandwidth is 20 Hz (harmonics > 10 are ignored)
2.2 INTRAVASCULAR SENSOR
sensor is
located in the tip of the catheter. This way the hydraulic connection is
replaced with an electrical or optical connection .The dispacement of the
diaphragm is measured .The frequency response is not limited by the hydraulic
properties of the system.
No time
delay.
Electrical
safety and isolation when using fiber optics Breaks easily
More
expensive
Disposable Sensors
Disposable
sensors decrease the risk of patient cross-contamination and reduce the amount
of handling by hospital personnel
Cheaper
and more reliable than reusable pressure sensors
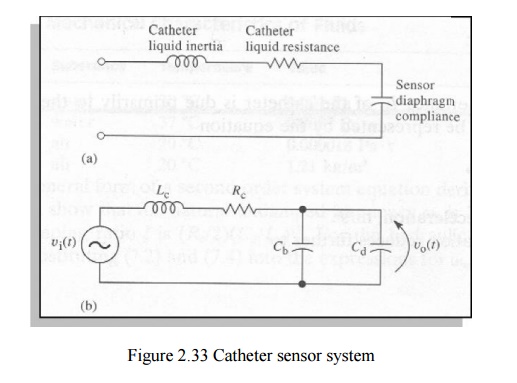
2.3 GENERAL ON SYSTEM PARAMETERS
Even
minute air bubbles in catheter have a dramatic effect on frequency response The
natural frequency and the length of the catheter have a following relationship:
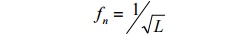
The
catheter diameter has a linear relationship to natural frequency Stiffer
catheters have a higher frequency response
Related Topics