Chapter: Surgical Pathology Dissection : The Female Genital System
Uterus : Surgical Pathology Dissection
Uterus
The
uterus is removed for a wide variety of reasons. Common indications for
hysterectomy include uterine prolapse, leiomyomas, endometrial hyperplasia,
cervical cancer, and endometrial cancer. Given the diverse nature of these
pro-cesses and the variation in the appearance of the uterus due to the
hormonal environment, it is important to know both the clinical indica-tion for
the surgery and the patient’s reproduc-tive status when evaluating a
hysterectomy specimen.
The
uterus is traditionally divided into two components: (1) the uterine corpus and
(2) the uterine cervix. The uterine corpus (or body) ex-tends from the
superiorly located fundus to the point of maximal narrowing which corresponds
to the location of the internal os. The right and left cornual regions are
located superolaterally, at the insertion of the fallopian tubes. The inferior
1 to 2 cm of the corpus is referred to as the isthmus or lower uterine segment
(LUS). This region is a ‘‘bridge’’ between the cervix and the uterus and
demonstrates a gradual transition from endocer-vical to endometrial mucosa. The
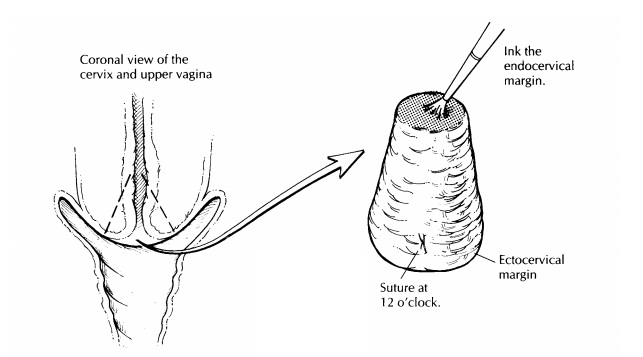
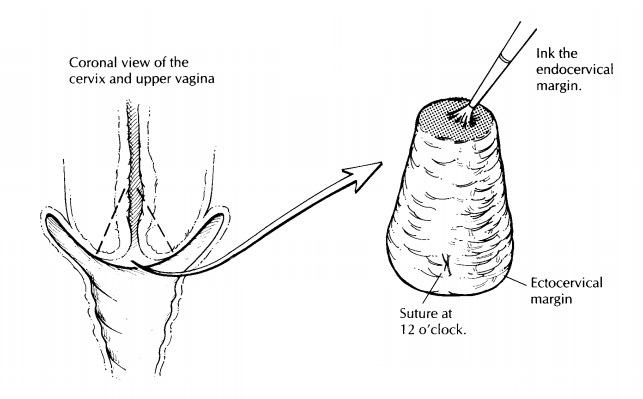
cervix encom-passes the lower portion of the uterus, beginning at the internal
os. The cervix is composed of an inner endocervical canal lined by columnar
epi-thelium and a rounded outer ectocervix covered by squamous epithelium. The
location of the squamocolumnar junction moves in and out of the cervical canal
with age and parity. It is within this region that most intraepithelial lesions
arise. Although the exact limits of this region are not visible grossly, the
term ‘‘transformation zone’’ encompasses this entire transition area including
the squamocolumnar junction.
This
section provides an approach to the eval-uation of hysterectomy specimens in
four cate-gories: (1) hysterectomies for nonmalignant disease, (2)
hysterectomies for endometrial can-cer, (3) radical hysterectomies for cervical
cancer, and (4) pelvic exenterations with vaginectomies for vaginal cancer or
recurrent cervical cancer.
Related Topics