Chapter: Essentials of Anatomy and Physiology: The Digestive System
Structural Layers of the Alimentary Tube
STRUCTURAL LAYERS OF THE ALIMENTARY TUBE
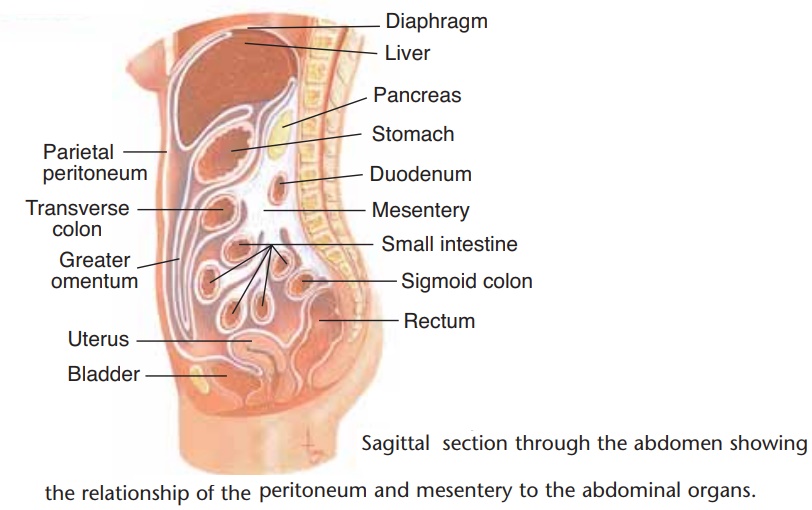
Before we continue with our discussion of the organs of digestion, we will first examine the typical structure of the alimentary tube. When viewed in cross-section, the alimentary tube has four layers (Fig. 16–4): the mucosa, submucosa, external muscle layer, and serosa. Each layer has a specific structure, and its functions contribute to the functioning of the organs of which it is a part.
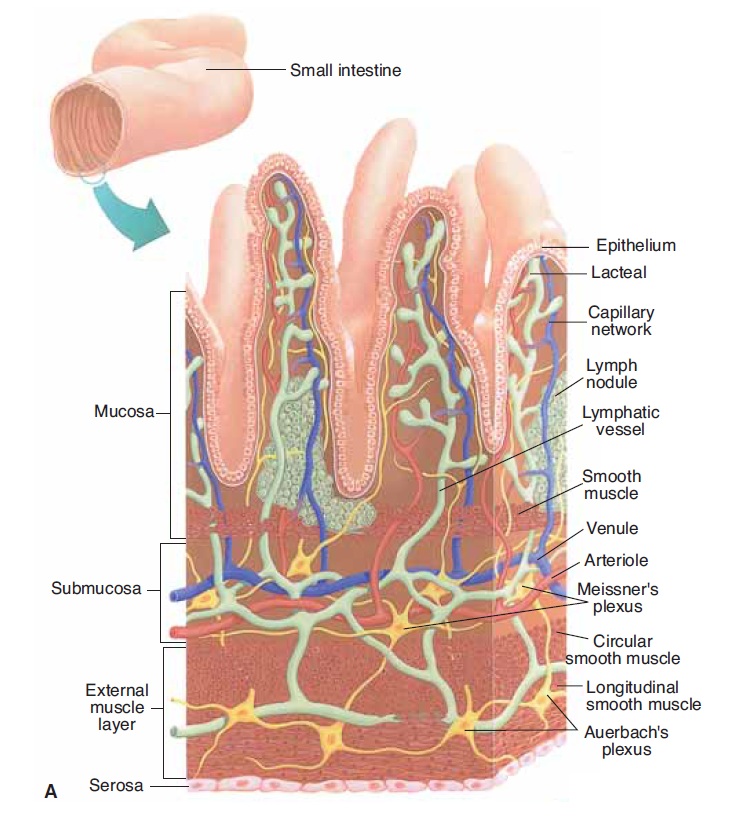
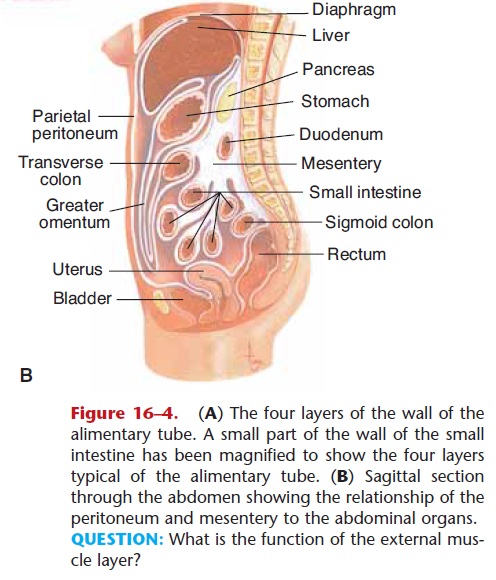
Figure 16–4. (A) The four layers of the wall of the alimentary tube. A small part of the wall of the small intestine has been magnified to show the four layers typical of the alimentary tube. (B) Sagittal section through the abdomen showing the relationship of the peritoneum and mesentery to the abdominal organs. QUESTION: What is the function of the external mus-cle layer?
MUCOSA
The mucosa, or lining, of the alimentary tube is made of epithelial tissue, areolar connective tissue, and two thin layers of smooth muscle. In the esophagus the epithelium is stratified squamous epithelium; in the stomach and intestines it is simple columnar epithe-lium. The epithelium secretes mucus, which lubricates the passage of food, and also secretes the digestive enzymes of the stomach and small intestine. Just below the epithelium, within the areolar connective tissue, are lymph nodules that contain lymphocytes to produce antibodies, and macrophages to phagocytize bacteria or other foreign material that get through the epithelium. The thin layers of smooth muscle create folds in the mucosa, and ripples, so that all of the epithelial cells are in touch with the contents of the organ. In the stomach and small intestine this is important for absorption.
SUBMUCOSA
The submucosa is made of areolar connective tissue with many blood vessels and lymphatic vessels. Many millions of nerve fibers are also present, part of what is called the enteric nervous system, or the “brain of the gut,” which extends the entire length of the ali-mentary tube. The nerve networks in the submucosa are called Meissner’s plexus (or submucosal plexus), and they innervate the mucosa to regulate secretions. Parasympathetic impulses increase secretions, whereas sympathetic impulses decrease secretions. Sensory neurons are also present to the smooth muscle (a stretched or cramping gut is painful), as are motor neurons to blood vessels, to regulate vessel diameter and blood flow.
EXTERNAL MUSCLE LAYER
The external muscle layer typically contains two layers of smooth muscle: an inner, circular layer and an outer, longitudinal layer. Variations from the typical do occur, however. In the esophagus, this layer is striated muscle in the upper third, which gradually changes to smooth muscle in the lower portions. The stomach has three layers of smooth muscle, rather than two.
Contractions of this muscle layer help break up food and mix it with digestive juices. The one-way contractions of peristalsis move the food toward the anus. Auerbach’s plexus (or myenteric plexus) is the portion of the enteric nervous system in this layer, and some of its millions of neurons are autonomic. Sympa-thetic impulses decrease contractions and peristalsis, whereas parasympathetic impulses increase contrac- tions and peristalsis, promoting normal digestion. The parasympathetic nerves are the vagus (10th cranial) nerves; they truly live up to the meaning of vagus, which is “wanderer.”
SEROSA
Above the diaphragm, for the esophagus, the serosa, the outermost layer, is fibrous connective tissue. Below the diaphragm, the serosa is the mesentery or visceral peritoneum, a serous membrane. Lining the abdomi-nal cavity is the parietal peritoneum, usually simply called the peritoneum. The peritoneum-mesentery is actually one continuous membrane (see Fig. 16–4). The serous fluid between the peritoneum and mesen-tery prevents friction when the alimentary tube con-tracts and the organs slide against one another.
The preceding descriptions are typical of the layers of the alimentary tube. As noted, variations are possi-ble, and any important differences are mentioned in the sections that follow on specific organs.
Related Topics