Chapter: Essentials of Anatomy and Physiology: The Digestive System
Functions of the Liver
FUNCTIONS OF THE LIVER
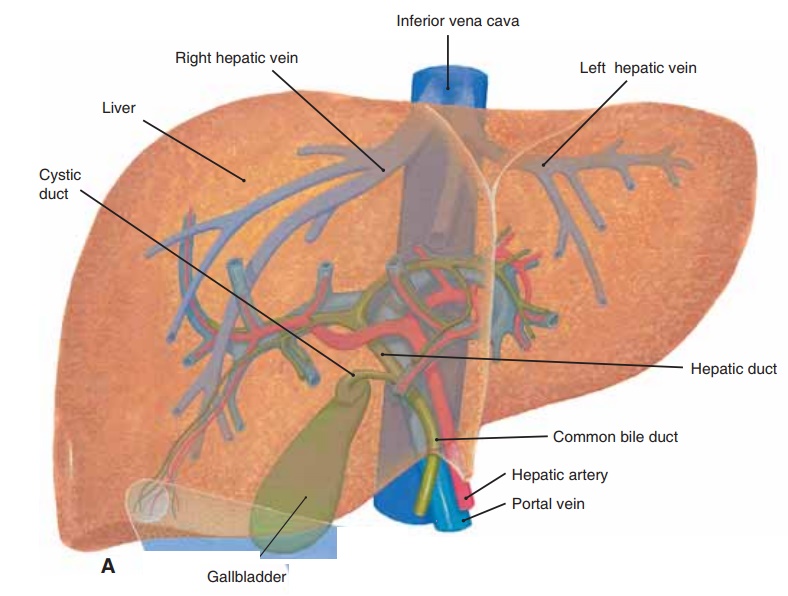
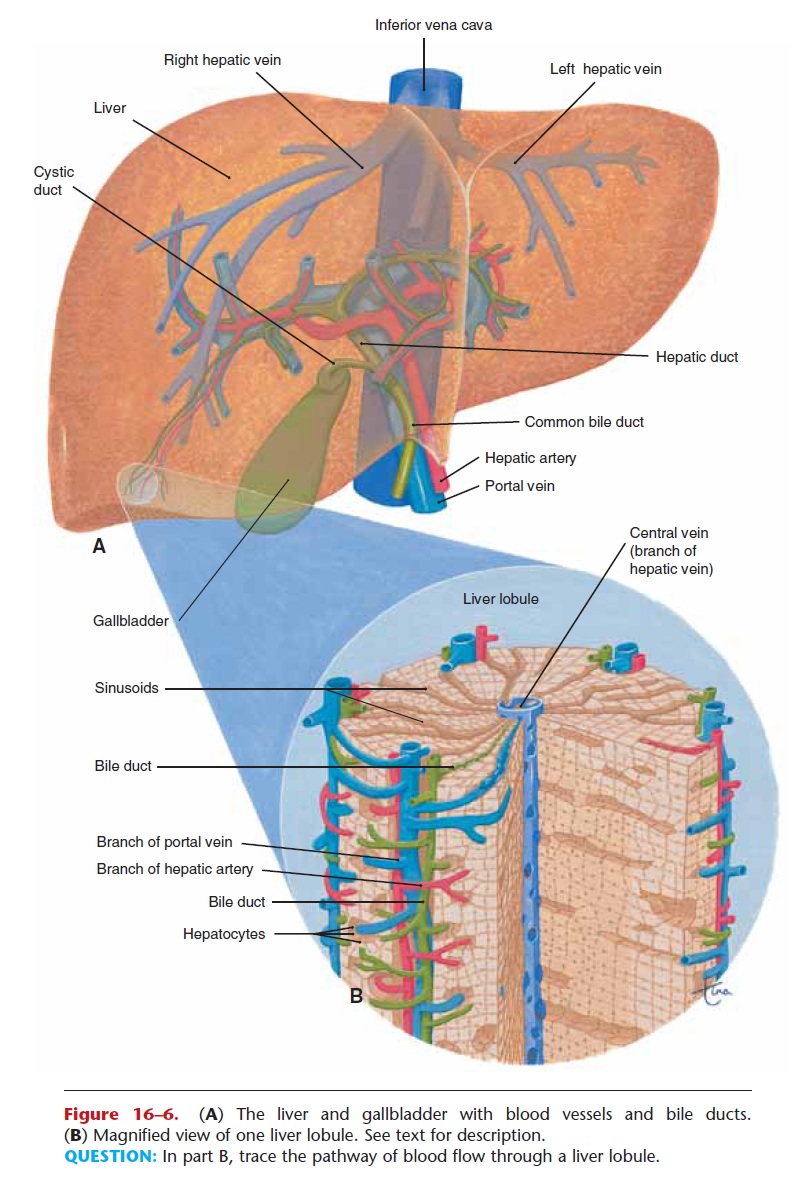
The liver is a remarkable organ, and only the brain is capable of a greater variety of functions. The liver cells (hepatocytes) produce many enzymes that cat-alyze many different chemical reactions. These reac-tions are the functions of the liver. As blood flows through the sinusoids (capillaries) of the liver (see Fig. 16–6), materials are removed by the liver cells, and the products of the liver cells are secreted into the blood. Some of the liver functions will already be familiar to you. Because the liver has such varied effects on so many body systems, we will use the categories below to summarize the liver functions.
1. Carbohydrate metabolism—As you know, the liver regulates the blood glucose level. Excess glu-cose is converted to glycogen (glycogenesis) when blood glucose is high; the hormones insulin and cortisol facilitate this process. During hypo-glycemia or stress situations, glycogen is converted back to glucose (glycogenolysis) to raise the blood glucose level. Epinephrine and glucagon are the hormones that facilitate this process.
The liver also changes other monosaccharides to glucose. Fructose and galactose, for example, are end products of the digestion of sucrose and lac-tose. Because most cells, however, cannot readily use fructose and galactose as energy sources, they are converted by the liver to glucose, which is eas-ily used by cells.
2. Amino acid metabolism—The liver regulates blood levels of amino acids based on tissue needs for protein synthesis. Of the 20 different amino acids needed for the production of human proteins, the liver is able to synthesize 12, called the non-essential amino acids. The chemical process by which this is done is called transamination, the transfer of an amino group (NH2) from an amino acid present in excess to a free carbon chain that forms a complete, new amino acid molecule. The other eight amino acids, which the liver cannot synthesize, are called the essential amino acids. In this case, “essential” means that the amino acids must be supplied by our food, because the liver cannot manufacture them. Similarly, “non-essen-tial” means that the amino acids do not have to be supplied in our food because the liver can make them. All 20 amino acids are required in order to make our body proteins.
Excess amino acids, those not needed right away for protein synthesis, cannot be stored. However, they do serve another useful purpose. By the process of deamination, which also occurs in the liver, the NH2 group is removed from an amino acid, and the remaining carbon chain may be con-verted to a simple carbohydrate molecule or to fat. Thus, excess amino acids are utilized for energy production: either for immediate energy or for the potential energy stored as fat in adipose tissue. The NH2 groups that were detached from the original amino acids are combined to form urea, a waste product that will be removed from the blood by the kidneys and excreted in urine.
3. Lipid metabolism—The liver forms lipoproteins, which as their name tells us, are molecules of lipids and proteins, for the transport of fats in the blood to other tissues. The liver also synthesizes choles-terol and excretes excess cholesterol into bile to be eliminated in feces.
Fatty acids are a potential source of energy, but in order to be used in cell respiration they must be broken down to smaller molecules. In the process of beta-oxidation, the long carbon chains of fatty acids are split into two-carbon molecules called acetyl groups, which are simple carbohydrates. These acetyl groups may be used by the liver cells to produce ATP or may be combined to form ketones to be transported in the blood to other cells. These other cells then use the ketones to pro-duce ATP in cell respiration.
4. Synthesis of plasma proteins—This is a liver function that you will probably remember The liver synthesizes many of the pro-teins that circulate in the blood. Albumin, the most abundant plasma protein, helps maintain blood vol-ume by pulling tissue fluid into capillaries.
The clotting factors are also produced by the liver. These, as you recall, include prothrombin, fibrinogen, and Factor 8, which circulate in the blood until needed in the chemical clotting mech-anism. The liver also synthesizes alpha and beta globulins, which are proteins that serve as carriers for other molecules, such as fats, in the blood.
5. Formation of bilirubin—This is another familiar function: The liver contains fixed macrophages that phagocytize old red blood cells (RBCs). Bilirubin is then formed from the heme portion of the hemoglobin. The liver also removes from the blood the bilirubin formed in the spleen and red bone marrow and excretes it into bile to be elimi-nated in feces.
6. Phagocytosis by Kupffer cells—The fixed macrophages of the liver are called Kupffer cells (or stellate reticuloendothelial cells). Besides destroying old RBCs, Kupffer cells phagocytize pathogens or other foreign material that circulate through the liver. Many of the bacteria that get to the liver come from the colon. These bacteria are part of the normal flora of the colon but would be very harmful elsewhere in the body. The bacteria that enter the blood with the water absorbed by the colon are carried to the liver by way of portal cir-culation. The Kupffer cells in the liver phagocytize and destroy these bacteria, removing them from the blood before the blood returns to the heart.
7. Storage—The liver stores the fat-soluble vitamins A, D, E, and K, and the water-soluble vitamin B12. Up to a 6- to 12-month supply of vitamins A and D may be stored, and beef or chicken liver is an excel-lent dietary source of these vitamins.
Also stored by the liver are the minerals iron and copper. You already know that iron is needed for hemoglobin and myoglobin and enables these pro- teins to bond to oxygen. Copper (as well as iron) is part of some of the proteins needed for cell respi-ration, and is part of some of the enzymes neces-sary for hemoglobin synthesis.
8. Detoxification—The liver is capable of synthesiz-ing enzymes that will detoxify harmful substances, that is, change them to less harmful ones. Alcohol, for example, is changed to acetate, which is a two-carbon molecule (an acetyl group) that can be used in cell respiration.
Medications are all potentially toxic, but the liver produces enzymes that break them down or change them. When given in a proper dosage, a medication exerts its therapeutic effect but is then changed to less active substances that are usually excreted by the kidneys. An overdose of a drug means that there is too much of it for the liver to detoxify in a given time, and the drug will remain in the body with possibly harmful effects. This is why alcohol should never be consumed when tak-ing medication. Such a combination may cause the liver’s detoxification ability to be overworked and ineffective, with the result that both the alcohol and the medication will remain toxic for a longer time. Barbiturates taken as sleeping pills after con-sumption of alcohol have too often proved fatal for just this reason.
Ammonia is a toxic substance produced by the bacteria in the colon. Because it is soluble in water, some ammonia is absorbed into the blood, but it is carried first to the liver by portal circulation. The liver converts ammonia to urea, a less toxic sub-stance, before the ammonia can circulate and dam-age other organs, especially the brain. The urea formed is excreted by the kidneys.
Related Topics