Chapter: Microbiology and Immunology: Virology, Virus: Arboviruses
Pathogenesis and Immunity - Hepatitis A Virus
Pathogenesis and Immunity
Hepatitis A virus infection is transmitted by the fecal–oral route and is associated with hepatic injury; however, the patho-genesis of HAV infection is not completely understood.
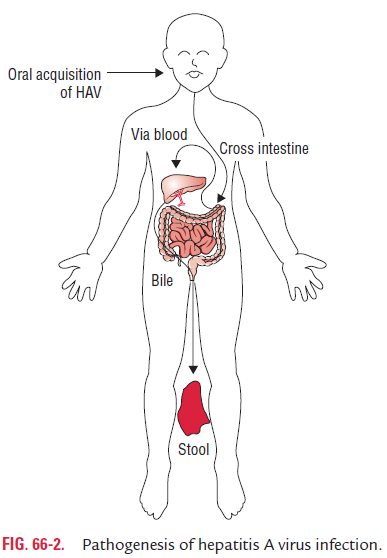
◗ Pathogenesis of hepatitis A virus infection
The virus appears to replicate first in the gastrointestinal tract and then spreads to the liver (Fig. 66-2). The viruses in the liver infect hepatocytes and cause damage to hepatocytes. But the mechanism by which HAV causes cytopathic effect is not known. Cytotoxic T cells appear to cause damage to hepa-tocytes; hence once the infection is cleared, the cell damage is repaired and no chronic infection occurs. The classic findings in the hepatocytes include mononuclear infiltrate, balloon-ing, degeneration, and acidophilic (Councilman-like) bodies. The liver pathology caused by HAV cannot be distinguished histologically from that caused by other hepatitis viruses.
◗ Host immunity
Host immunity is mediated primarily by circulating anti-bodies. Acute infection is characterized by the appearance of IgM anti-HAV, which is detectable at the time of appear-ance of jaundice in the initial stage of infection. But the IgM antibody disappears several months after jaundice. The IgG antibody appears 1–3 weeks after appearance of IgM anti-bodies. IgG antibody appears to provide lifelong immunity against recurrent HAV infection.
Related Topics