Chapter: Essentials of Anatomy and Physiology: Endocrine System
Pancreas, Insulin, and Diabetes - Endocrine Glands and Their Hormones
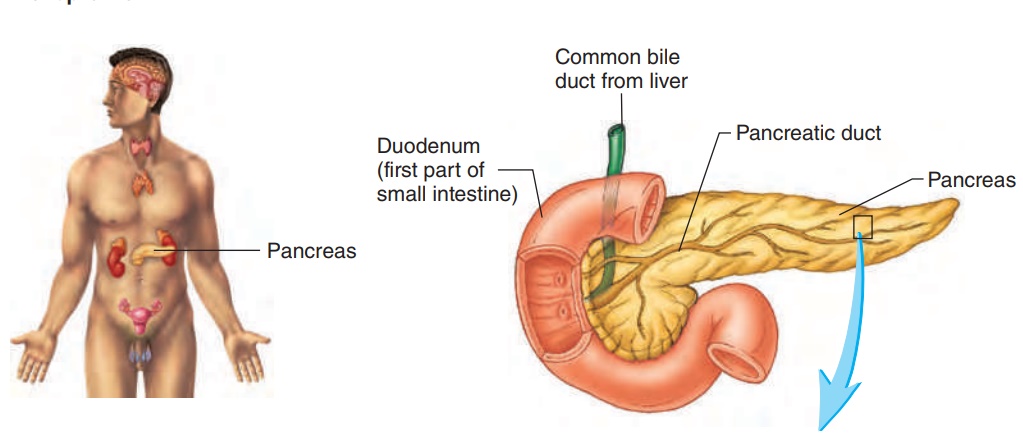
Pancreas, Insulin, and Diabetes
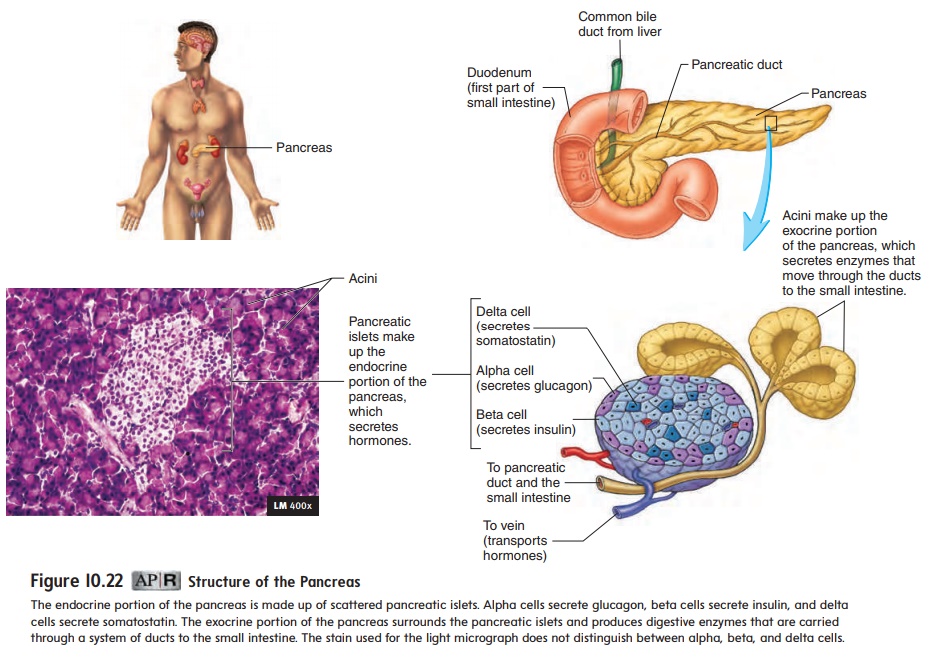
The endocrine part of the pancreas (pan′ krē-as) consists of pan-creatic islets (islets of Langerhans), which are dispersed through-out the exocrine portion of the pancreas (figure 10.22). The islets secrete three hormones—insulin, glucagon, and somatostatin— which help regulate the blood levels of nutrients, especially glu-cose (table 10.3). Alpha cells secrete glucagon, beta cells secrete insulin, and delta cells secrete somatostatin.
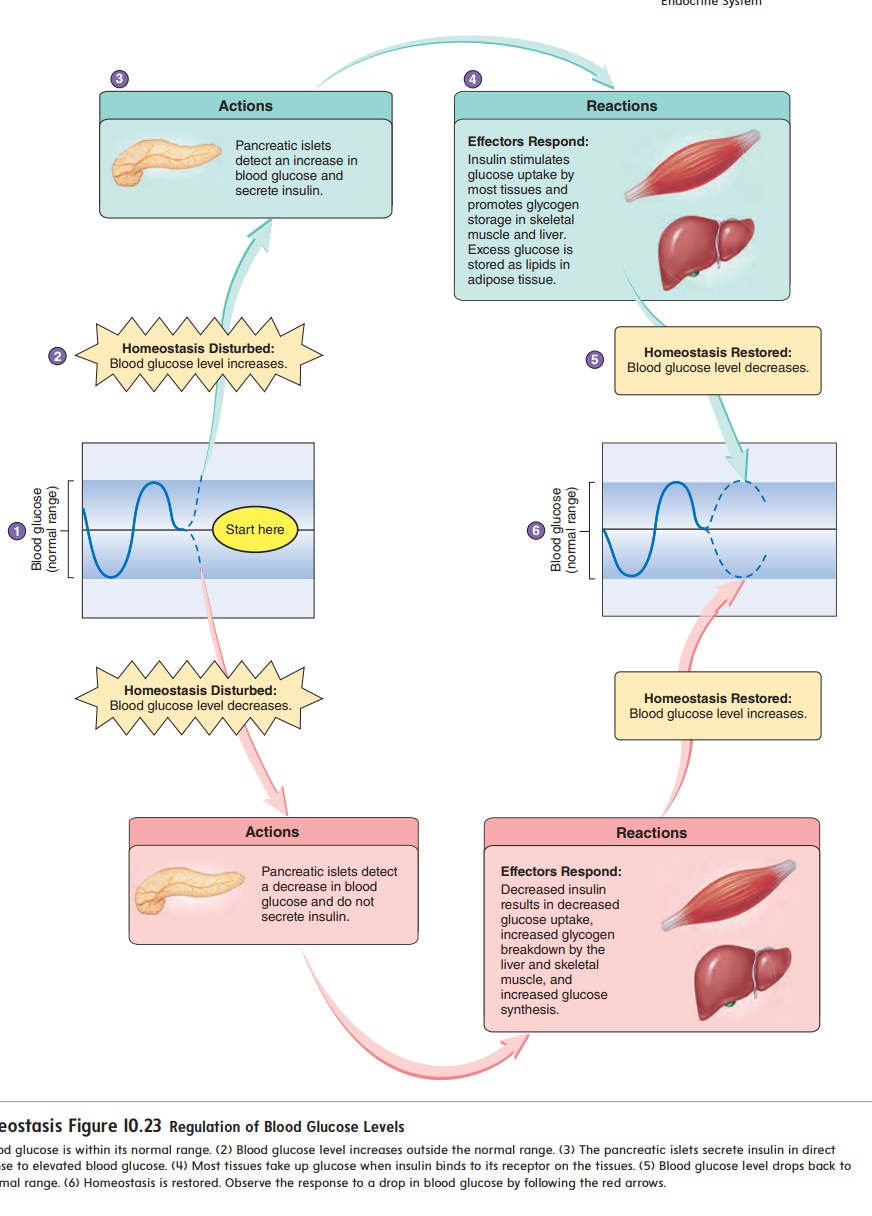
It is very important to maintain blood glucose levels within a normal range (figure 10.23). A below-normal blood glucose level causes the nervous system to malfunction because glucose is the nervous system’s main source of energy. When blood glucose decreases, other tissues rapidly break down lipids and proteins to provide an alternative energy source. As lipids are broken down, the liver converts some of the fatty acids to acidic ketones (kē′ tōnz), which are released into the blood. When blood glucose levels are very low, the breakdown of lipids can cause the release of enough fatty acids and ketones to reduce the pH of the body fluids below normal, a condition called acidosis (as-i-dō′ sis). The amino acids of proteins are broken down and used by the liver to synthesize glucose.
If blood glucose levels are too high, the kidneys produce large volumes of urine containing substantial amounts of glucose. Because of the rapid loss of water in the form of urine, dehydra-tion can result.
The hormone insulin (in′ sŭ-lin) is released from the beta cells primarily in response to the elevated blood glucose levels and increased parasympathetic stimulation associated with digestion of a meal. Increased blood levels of certain amino acids also stimulate insulin secretion. Decreased insulin secretion results from decreasing blood glucose levels and from stimulation of the pancreas by the sympathetic division of the nervous system, which occurs during physical activity. Decreased insulin levels allow blood glucose to be conserved to provide the brain with adequate glucose and to allow other tissues to metabolize fatty acids and glycogen stored in the cells.
The major target tissues for insulin are the liver, adipose tissue, muscles, and the area of the hypothalamus that controls appetite, called the satiety (sa-tı̄′ -ĕ-tē; fulfillment of hunger) center.
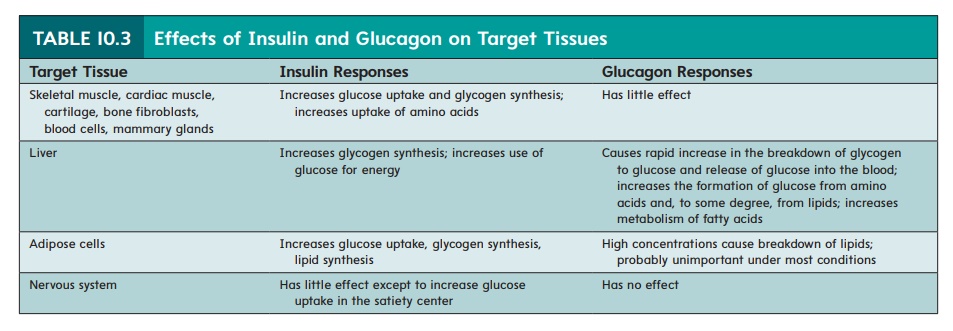
Insulin binds to membrane-bound receptors and, either directly or indirectly, increases the rate of glucose and amino acid uptake in these tissues. Glucose is converted to glycogen or lipids, and the amino acids are used to synthesize protein. The effects of insulin on target tissues are summarized in table 10.3.
Diabetes mellitus (dı̄-ă-bē′tēz′me-lı̄′tŭs; much urine honey or sweetened) has several causes. Type 1 diabetes mellitus occurs when too little insulin is secreted from the pancreas, and type 2 diabetes mellitus is caused by insufficient numbers of insu- lin receptors on target cells or by defective receptors that do not respond normally to insulin.
In type 1 diabetes mellitus, tissues cannot take up glucose effectively, causing blood glucose levels to become very high, a condition called hyperglycemia (hı̄′ per-glı̄-sē′ mē-ă; hyper, above + glycemia, blood glucose). Because glucose cannot enter the cells of the satiety center in the brain without insulin, the satiety center responds as if there were very little blood glucose, result- ing in an exaggerated appetite. The excess glucose in the blood is excreted in the urine, making the urine volume much greater than normal. Because of excessive urine production, the person has a tendency to become dehydrated and thirsty. Even though blood glucose levels are high, lipids and proteins are broken down to provide an energy source for metabolism, resulting in the wasting away of body tissues, acidosis, and ketosis. People with this condi- tion also exhibit a lack of energy. Insulin must be injected regularly to adequately control blood glucose levels. When too much insulin is present, as occurs when a diabetic is injected with too much insu- lin or has not eaten after an insulin injection, blood glucose levels become very low. The brain, which depends primarily on glucose for an energy source, malfunctions. This condition, called insulin shock, can cause disorientation and convulsions and may result in loss of consciousness. Fortunately genetic engineering has allowed synthetic insulin to become widely available to diabetics.
Glucagon (gloo′kă-gon) is released from the alpha cellswhen blood glucose levels are low. Glucagon binds to membrane-bound receptors primarily in the liver, causing the glycogen stored in the liver to be converted to glucose. The glucose is then released into the blood to increase blood glucose levels. After a meal, when blood glucose levels are elevated, glucagon secretion is reduced.
Somatostatin (sō′mă-tō′statı̆n) is released by the delta cellsin response to food intake. Somatostatin inhibits the secretion of insulin and glucagon and inhibits gastric tract activity.
Insulin and glucagon together regulate blood glucose levels (see figure 10.23). When blood glucose levels increase, insulin secretion increases, and glucagon secretion decreases. When blood glucose levels decrease, the rate of insulin secretion declines, and the rate of glucagon secretion increases. Other hormones, such as epinephrine, cortisol, and growth hormone, also maintain blood levels of nutrients. When blood glucose levels decrease, these hormones are secreted at a greater rate. Epinephrine and cortisol cause the breakdown of protein and lipids and the synthesis of glu-cose to help increase blood levels of nutrients. Growth hormone slows protein breakdown and favors lipid breakdown.
Related Topics