Chapter: Biology of Disease: The Nature and Investigation of Diseases
Hospital Laboratory Tests
HOSPITAL LABORATORY TESTS
Hospital laboratories routinely offer a wide range of
clinical tests all of which must undergo a thorough evaluation for both
analytical and clinical performance. The clinical demand for the test has to be
established and its clinical relevance is subject to review. In addition to
thorough evaluation of analytical methods, other aspects, such as the stability
of samples, needs to be considered. For example, some samples must be assayed
immediately while others can be stored at an appropriate temperature. All
laboratory staff must be appropriately trained to ensure high analytical
standards and produce valid data. This usually means that control urine and
sera are run through the analyzers at regular intervals to check that the
methods are working properly and reproducibly. Many of the companies that
supply apparatus and reagents also supply standard sera for example, which are
tested in laboratories all over the country, and the results are recorded in a
nationwide database so that comparisons can be made and laboratories can check
that their methods are all giving the same results.
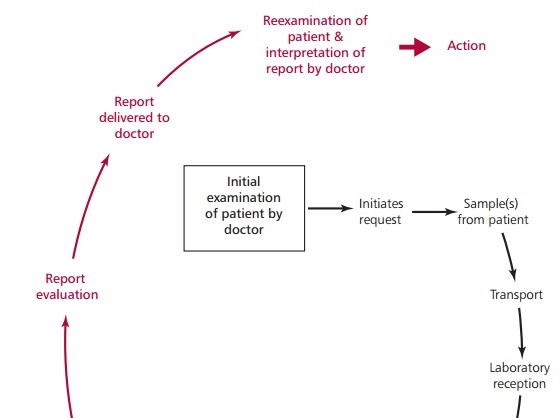
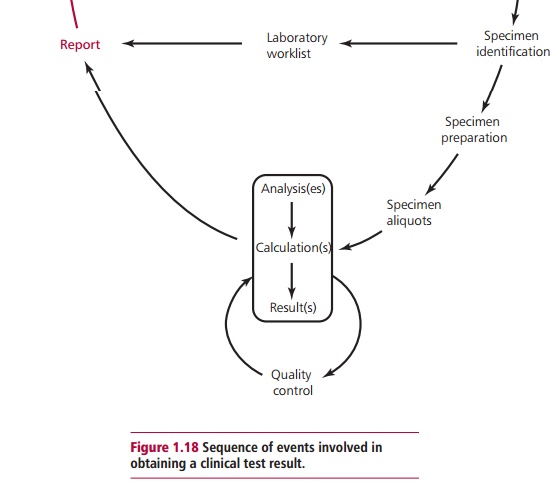
Figure 1.18 illustrates the
overall procedure routinely followed when a clinicianrequires a hospital test.
Note that this procedure can be divided into a number of distinct steps:
•
request for the test ( a form; patient’s details
recorded);
•
specimen collection, labeling, transport and storage
(instructions);
•
analysis (obtaining the results);
•
interpretation (the results are often printed out with the range
of values to help the doctor make an interpretation).
Prior to any test being requested, careful thought should be
given as to whether the test is necessary and how its results will affect the
management of the disease for the benefit of the patient. If this is not the
case, then one has to consider the value in requesting and performing the test.
Unfortunately clinicians sometimes request clinical tests that are unnecessary
and will not be of benefit in treating the patient. This problem often occurs
when using forms on which tests can be requested simply by ticking a box.
Requesting unnecessary tests poses a number of problems for the patients,
clinicians, the biomedical scientists (medical technologists in the USA) and
the hospital. The test means that the patient is put to an inconvenience, as
extra specimens are required. Unnecessary tests can be misleading and result in
poor patient management while imposing a financial burden on the hospital. The
increased workload for laboratory scientific staff may make the clinician in
question rather unpopular! However, set against this is the fact that many of
the machines used in the hospital for clinical analysis routinely test for a
number of analytes, whether they are asked to or not, since it is easier to set
up the machine in this way rather than to adjust them for individual patients.
Specimens are collected in a variety of ways (Figure 1.19) from the collection of
blood using a simple thumbprick or, more usually a syringe, to surgery to
obtain a biopsy, where a small piece
of tissue is taken from the patient.

Blood needs to be collected with care . If too many erythrocytes
burst, this is known as hemolysis;
the specimen will be unsuitable for the determination of some analytes: for
example, the value obtained for ‘serum K+’ will not be a true value
since potassium is released from hemolyzed blood cells. Blood should not be
collected from an arm that is receiving an infusion as a drip, since this will
dilute the blood. Often, in such cases, the measured concentrations of electrolytes
and glucose in the blood samples resemble those of the infusion fluid.
For some analytes, the blood must be collected into a tube
containing an anticoagulant or preservative. Specimens of blood for glucose
determination must be collected into a tube containing fluoride ions (F–)
since this inhibits glycolysis and prevents the utilization of serum glucose by
blood cells. Occasionally blood is collected into the wrong tube and then
decanted into the correct tube. This can cause a number of problems. For
example, blood collected into a tube containing ethylene diamine tetraacetate
(EDTA) will be unsuitable for the determination of serum Ca2+, since
EDTA is an anticoagulant, works by chelating and removing available Ca2+.
The transport of specimens and their storage must be considered
carefully since an inappropriate environment can influence the values of
clinical test results. Swabs, for example, obtained during a microbiological
investigation of an affected site, contain only a small volume of specimen and
dry easily. They therefore need to be transported to the laboratory as quickly
as possible
Blood specimens that have been stored
overnight may show erroneously high concentrations of serum K+,
phosphate and activities of erythrocyte enzymes because these all leak from the
cells during storage. To prevent this happening, the serum should be separated
from blood cells immediately following collection and stored separately if it
is to be analyzed the following day.
Certain samples require a timed collection, for example, the
collection of urine specimens over a 24-hour period for determination of
creatinine clearance values or the collection of stools over a three-day period
for fecal fat determination to assess malabsorption . The results obtained for
such tests often lack accuracy because of the practical difficulties in
obtaining accurately timed specimens from the patient.
Related Topics