Chapter: Clinical Cases in Anesthesia : Malignant Hyperthermia
Distinguish among the major types of diabetes mellitus (DM)
Distinguish
among the major types of diabetes mellitus (DM).
DM is the presence of elevated plasma glucose
under fasting conditions. Type I, or insulin-dependent DM (IDDM), occurs in
about 10% of all diabetics in the Western world (Table 29.1). Classically, this
type of DM presents in child-hood or early adolescence; however, it can
manifest at any age. The presentation is usually abrupt, with onset of symptoms
secondary to severe insulin insufficiency. Type I DM patients are prone to
ketosis and are usually thin. The pathogenesis of IDDM is thought to involve
certain histocompatibility locus antigens (HLA) on chromosome 6. In the most
common form of IDDM (type IA), environ-mental factors, such as viral
infections, are postulated to combine with genetic factors to cause
cell-mediated autoimmune destruction of pancreatic beta cells. The sec-ond type
of IDDM (type IB) is found in about 10% of all IDDM patients and is thought to
involve primary auto-immune damage. This type of IDDM is associated with other
autoimmune endocrinopathies such as Hashimoto’s thyroiditis, Graves’ disease,
and other nonendocrine autoimmune disorders.
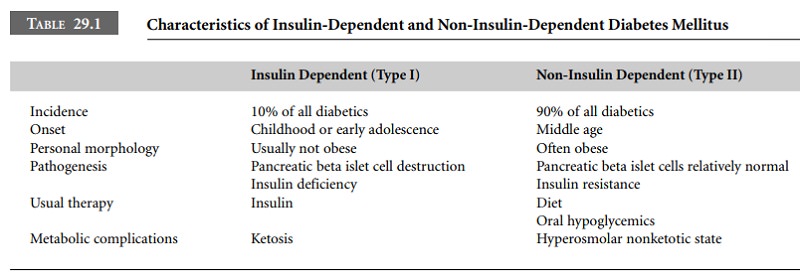
Type II DM, or non-insulin-dependent DM
(NIDDM), occurs in 90% of all diabetics. However, the name may be misleading
since some patients may require insulin to cor-rect persistent fasting
hyperglycemia if diet and oral agents fail to do so. The requirement of insulin
for glucose control does not distinguish between IDDM and NIDDM. Although these
patients are not ketosis prone, they still may develop ketosis under
circumstances of severe stress. The pathogenesis of NIDDM is also thought to
involve genetic factors as expressed by a strong familial pattern for NIDDM.
There appears to be a difference between obese and non-obese NIDDM patients.
Sixty to eighty percent of NIDDM patients have insulin resistance resulting
from weight gain and obesity. In most patients, a diagnosis of NIDDM is made
during middle age. In a subclass of patients, DM presents during childhood or
adolescence, which is known as maturity onset-type diabetes of the young
(MODY). This has an established autosomal dominant inheritance pattern.
Gestational DM (GDM) is defined as the onset of glucose intolerance during
pregnancy. About 2% of all pregnancies are associated with GDM, which is
related to an increase in perinatal morbid-ity and mortality. Although most
patients return to a state of normal glucose tolerance following parturition,
about 60% will develop DM within 15 years.
Other forms of DM include malnutrition-related
DM, which is a non-ketosis-prone form associated with severe protein
malnutrition and emaciation. Most cases require insulin for preservation of
life. DM may also be secondary to other endocrine diseases (e.g., Cushing
syndrome), drug administration (e.g., antihypertensive drugs, estro-gens), and
many genetic syndromes. DM may also result from severe pancreatic disease or
resection of pancreatic tissue.
Related Topics