Chapter: Clinical Cases in Anesthesia : Malignant Hyperthermia
Describe the oral hypoglycemic agents and insulin preparations available to treat DM
Describe
the oral hypoglycemic agents and insulin preparations available to treat DM.
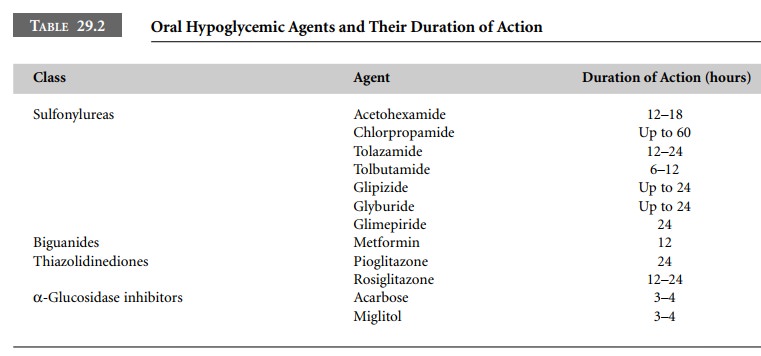
Oral hypoglycemic agents fall into four broad classes depending on their mechanism of action. Table 29.2 summarizes the commonly used agents and their anticipated duration of action. All these drugs are ineffective in IDDM.
·
The
sulfonylureas (tolbutamide, glyburide, glipizide, and glimepiride) and
meglitinides (repaglinide and netaglinide) increase insulin secretion by the
pancreas and reduce insulin resistance. Hypoglycemia is the major complication
associated with sulfonylurea therapy. There has also been concern that some of
the sulfonylureas increase the incidence of myocardial infarction.
· Biguanides (metformin) decrease gluconeogenesis in the liver. Other beneficial effects, which make metformin a popular treatment, include weight loss, a decrease in triglycerides and low-density lipoproteins, and an increase in high-density lipoproteins. Metformin has been shown to decrease the incidence of myocardial infarction in obese patients with type II DM.
· Thiazolidinediones (pioglitazone and
rosiglitazone), the newest hypoglycemic agents, improve insulin sensitivity of
muscle and fat cells.
·
α-Glucosidase inhibitors (acarbose and miglitol)
inhibit intestinal α-glucoside, thus the absorption of glucose is
delayed in the intestine. Hypoglycemia does not occur if these drugs are used
alone.
Insulin therapy is necessary for all IDDM
patients, and NIDDM patients inadequately treated with oral hypo-glycemics.
Insulin comes in two concentrations: 100 U/mL and 500 U/mL (U-100 and U-500,
respectively). Insulin preparations differ in their source (e.g., pork,
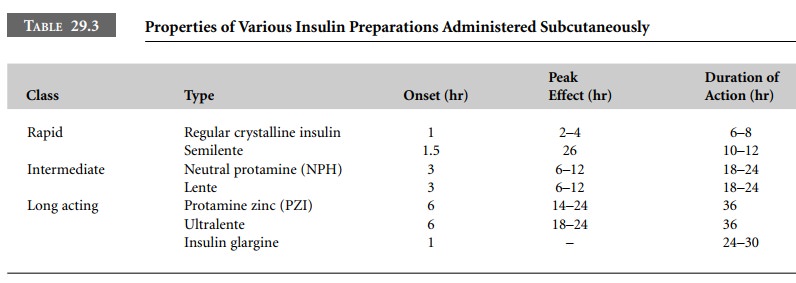
recombinant human), degree of purity, and time course of action. Table 29.3
lists the characteristics of insulin preparations. The half-life of intravenous
regular insulin is approxi-mately 5 minutes; the effect lasts about 1 hour.
Related Topics