Chapter: Medical Surgical Nursing: Shock and Multisystem Failure
Circulatory Shock
Circulatory Shock
Circulatory or distributive shock occurs when blood volume is abnormally
displaced in the vasculature—for example, when blood volume pools in peripheral
blood vessels. The displacement of blood volume causes a relative hypovolemia
because not enough blood returns to the heart, which leads to subsequent
in-adequate tissue perfusion. The ability of the blood vessels to con-strict
helps return the blood to the heart. Thus, the vascular tone is determined both
by central regulatory mechanisms, as in blood pressure regulation, and by local
regulatory mechanisms, as in tis-sue demands for oxygen and nutrients.
Therefore, circulatory shock can be caused either by a loss of sympathetic tone
or by re-lease of biochemical mediators from cells.
The varied mechanisms
leading to the initial vasodilation in circulatory shock further subdivide this
classification of shock into three types: (1) septic shock, (2) neurogenic
shock, and anaphylactic shock.
The different types of circulatory shock cause variations in the
pathophysiologic chain of events and are explained here separately. In all
types of circulatory shock, massive arterial and venous dila-tion allows blood
to pool peripherally. Arterial dilation reduces sys-temic vascular resistance.
Initially, cardiac output can be high in circulatory shock, both from the
reduction in afterload (systemic vascular resistance) and from the heart
muscle’s increased effort to maintain perfusion despite the incompetent
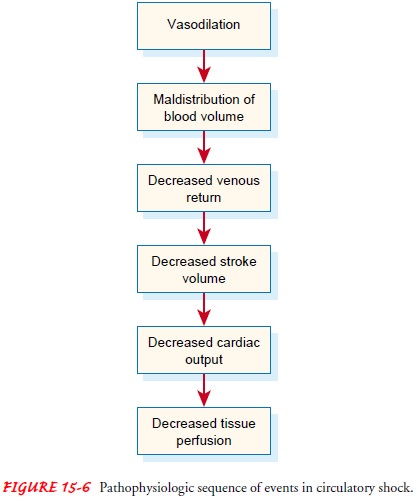
vasculature secondary to arterial dilation. Pooling of blood in the periphery
results in de-creased venous return. Decreased venous return results in
de-creased stroke volume and decreased cardiac output. Decreased cardiac
output, in turn, causes decreased blood pressure and ulti-mately decreased
tissue perfusion. Figure 15-6 presents the patho-physiologic sequence of events
in circulatory shock.
Related Topics