Chapter: Medical Surgical Nursing: Assessment of Cardiovascular Function
Assessment of Cardiovascular Function: Health History and Clinical Manifestations
HEALTH HISTORY AND CLINICAL MANIFESTATIONS
For
the patient experiencing an acute MI, the nurse obtains the health history
using a few specific questions about the onset and severity of chest
discomfort, associated symptoms, current med-ications, and allergies. At the
same time, the nurse observes the patient’s general appearance and evaluates
hemodynamic status (heart rate and rhythm, BP). Once the condition of the
patient stabilizes, a more extensive history can be obtained.
With stable patients, a complete health history is obtained during the initial contact. Often, it is helpful to have the patient’s spouse or partner available during the health history interview. Initially, demographic information regarding age, gender, and ethnic origin is obtained. The family history, as well as the physi-cal examination, should include assessment for genetic abnormal-ities associated with cardiovascular disorders (see Genetics in Nursing Practice box). Height, current weight, and usual weight (if there has been a recent weight loss or gain) are established. Dur-ing the interview, the nurse conveys sensitivity to the cultural background and religious practices of the patient. This removes barriers to communication that may result if the interview is based only on the nurse’s personal frame of reference. Patients from different cultural and ethnic groups may have different ways of describing symptoms such as pain and may engage in different health practices before seeking formal medical attention.
The
baseline information derived from the history assists in identifying pertinent
issues related to the patient’s condition and educational and self-care needs.
Once these problems are clearly identified, a plan of care is instituted.
During subsequent contacts or visits with the patient, a more focused health
history is per-formed to determine whether goals have been met, whether the
plan needs to be modified, and whether new problems have de-veloped. During the
interview, the nurse asks questions to evalu-ate cardiac symptoms and health
status.
Cardiac Signs and Symptoms
Patients
with cardiovascular disorders commonly have one or more of the following signs
and symptoms:
·
Chest pain or discomfort (angina
pectoris, MI, valvular heart disease)
·
Shortness of breath or dyspnea (MI,
left ventricular fail-ure, HF)
·
Edema and weight gain (right
ventricular failure, HF)
·
Palpitations (dysrhythmias resulting
from myocardial is-chemia, valvular heart disease, ventricular aneurysm,
stress, electrolyte imbalance)
·
Fatigue (earliest symptom associated
with several cardio-vascular disorders)
·
Dizziness and syncope or loss of
consciousness (postural hypotension, dysrhythmias, vasovagal effect,
cerebrovascular disorders)
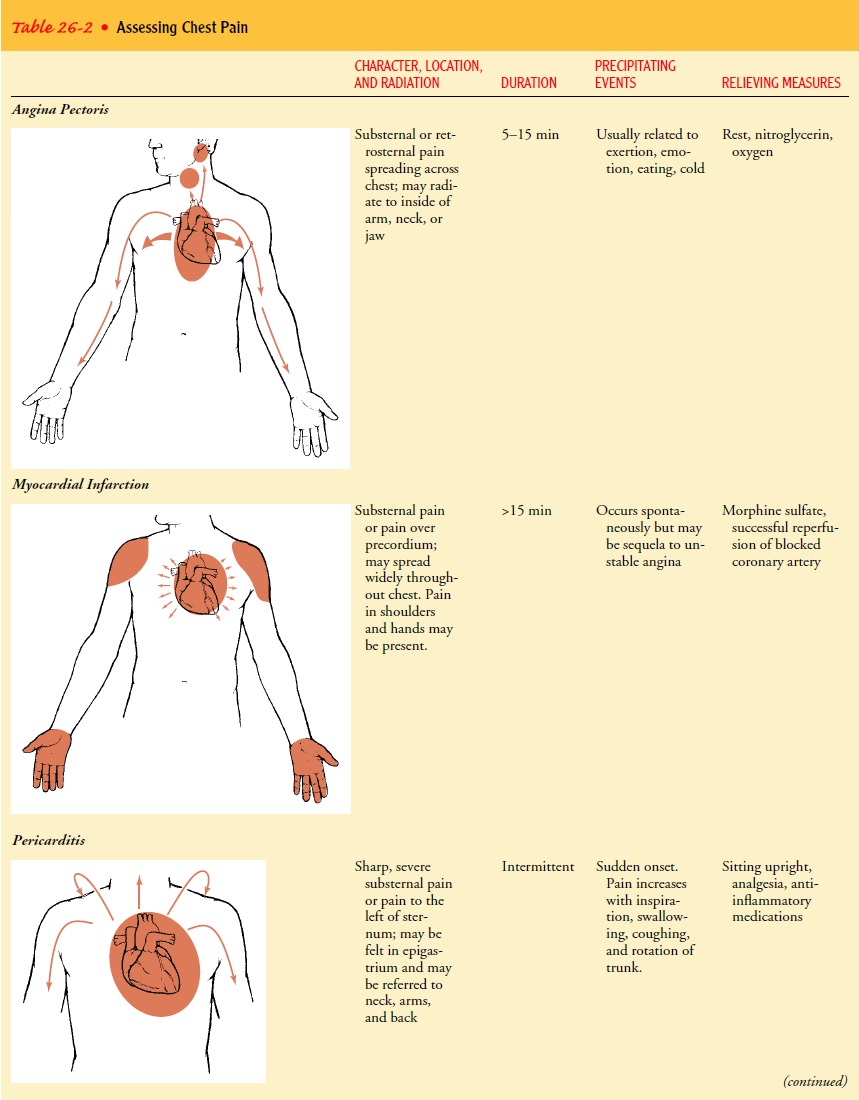
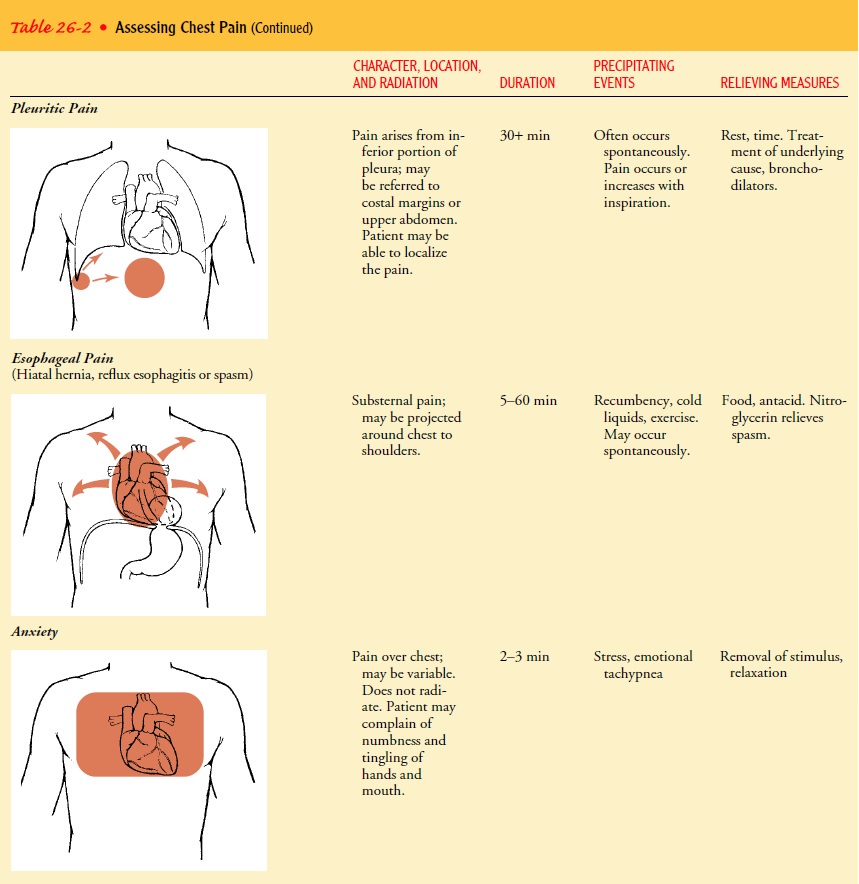
Not
all chest discomfort is related to myocardial ischemia. When a patient has
chest discomfort, questions should focus on differentiating a serious,
life-threatening condition such as MI from conditions that are less serious or
that would be treated differently (see Table 26-2).
The
following points should be remembered when assessing patients with cardiac
symptoms:
·
Women are more likely to present
with atypical symptoms of MI than are men.
·
There is little correlation between
the severity of the chest discomfort and the gravity of its cause. Elderly
people and those with diabetes may not have pain with angina or MI because of
neuropathies. Fatigue and shortness of breath may be the predominant symptoms
in these patients.
·
There is poor correlation between
the location of chest dis-comfort and its source.
·
The patient may have more than one
clinical condition oc-curring simultaneously.
·
In a patient with a history of CAD,
the chest discomfort should be assumed to be secondary to ischemia until proven
otherwise.
HEALTH PERCEPTION AND MANAGEMENT
In
an effort to determine how patients perceive their current health status. The
nurse might ask some of the following questions:
Do
you have any health problems? If so, what do you think caused them?
How
has your health been recently? Have you noticed any changes from last year?
from 5 years ago?
Do
you have a cardiologist or primary health care provider?
How
often do you go for checkups?
Do
you use tobacco or consume alcohol?
What
are your risk factors for heart disease? What do you do to stay healthy and
take care of your heart?
What
prescription and over-the-counter medications are you taking? Do you take
vitamins or herbal supplements?
Some
patients may not be aware of their own medical diag-nosis. For example,
patients may not realize that their heart attack was caused by CAD. Patients
who do not understand that their be-haviors or diagnoses pose a threat to their
health may be less moti-vated to make lifestyle changes or to manage their
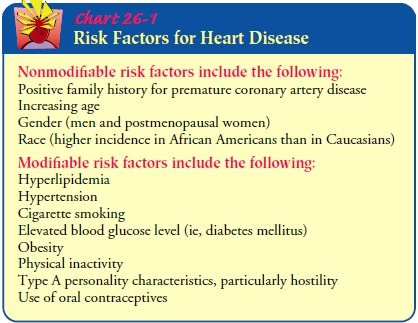
illness effectively. On the other hand, patients who perceive that their
modifiable cardiovascular risk factors have contributed to their health
con-ditions may be more likely to change these behaviors (Chart 26-1).

The patient’s ability to recognize cardiac symptoms and to know what to do when they occur is essential for effective self-care management.
All too often, patients’ new symptoms or symptoms of progressing cardiac
dysfunction go unrecognized. This results in prolonged delays in seeking
life-saving treatment. Major bar-riers to seeking prompt medical care include
lack of knowledge about symptoms to expect with heart disease, attribution of
symptoms to a benign source, psychological factors such as denial of symptom
significance, and social factors, specifically feeling embarrassed about having
symptoms (Zerwic, 1999).
An
additional issue to consider is the patient’s medication his-tory, dosages, and
schedules. Is the patient independent in taking medications? Are the
medications taken as prescribed? Does the patient understand why the medication
regimen is important? Are doses ever forgotten or skipped, or does the patient
ever decide to stop taking a medication? An aspirin a day is a common
non-prescription medication that improves patient outcomes after an MI.
However, if patients are not aware of this benefit, they may be inclined to
stop taking aspirin if they think it is a trivial medication. A careful
medication history will often uncover common medica-tion errors and causes for
nonadherence to the medication regimen.
Table
26-2 summarizes the characteristics and patterns of the more common cardiac and
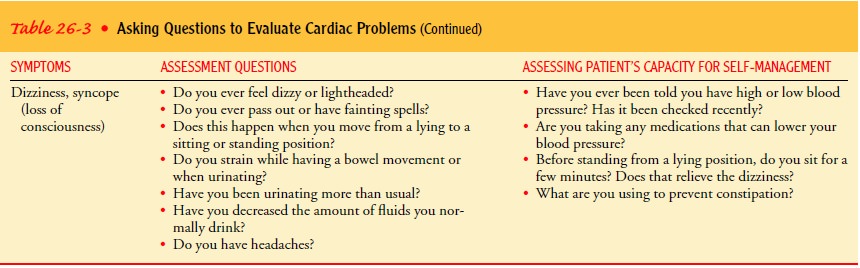
noncardiac causes of chest pain. Table 26-3 identifies typical questions nurses
use to assess cardiac signs and symptoms, as well as those used to determine
the patient’s ability to recognize and manage them. Some of the patient’s
responses may require further clarification and follow-up.


NUTRITION AND METABOLISM
Dietary
modifications, exercise, weight loss, and careful monitor-ing are important
strategies for managing three major cardiovascu-lar risk factors:
hyperlipidemia, hypertension, and hyperglycemia (diabetes mellitus). Diets that
are restricted in sodium, fat, choles-terol, and/or calories are commonly
prescribed. The nurse should obtain the following information:
·
The patient’s current height and
weight (to determine body mass index), waist measurement (assessment for
obesity), BP, and any laboratory test results such as blood glucose,
glycosylated hemoglobin (diabetes), total blood cholesterol, high-density and
low-density lipoprotein levels, and triglyc-eride levels (hyperlipidemia).
·
How often the patient self-monitors
BP, blood glucose, and weight as appropriate to the medical diagnoses.
·
The patient’s level of awareness
regarding his or her target goals for each of the risk factors and any problems
achiev-ing or maintaining these goals.
·
What the patient normally eats and
drinks in a typical day and any food preferences (including cultural or ethnic
preferences).
·
Eating habits (canned or
commercially prepared foods ver-sus fresh foods, restaurant cooking versus home
cooking, assessing for high sodium foods, dietary intake of fats).
·
Who shops for groceries and prepares
meals.
ELIMINATION
Typical bowel and bladder habits need to
be identified. Nocturia (awakening at night to urinate) is common for patients
with HF. Fluid collected in the dependent tissues (extremities) during the day
redistributes into the circulatory system once the patient is recumbent at
night. The increased circulatory volume is excreted by the kidneys (increased
urine production). Patients need to be aware of their response to diuretic
therapy and any changes in uri-nation. This is vitally important for patients
with HF. Patients may be taught to modify (titrate) their dose of diuretics
based on urinary pattern, daily weight, and symptoms of dyspnea.
To avoid straining, patients who become
easily constipated need to establish a regular bowel regimen. When straining,
the pa-tient tends to bear down (the Valsalva maneuver), which momen-tarily
increases pressure on the baroreceptors. This triggers a vagal response,
causing the heart rate to slow down and resulting in syncope in some patients.
For the same reason, straining during urination should be avoided. Because many
cardiac medications can cause gastrointestinal side effects or bleeding, the nurse
asks about bloating, diarrhea, constipation, stomach upset, heart-burn, loss of
appetite, nausea, and vomiting. Patients taking platelet-inhibiting medications
such as aspirin and clopidogrel (Plavix); intravenous GP IIb/IIIa platelet
aggregation inhibitors such as abciximab (ReoPro), eptifibatide (Integrilin),
and tirofiban (Aggrastat); and anticoagulants such as low-molecular-weight heparin
(ie, dalteparin [Fragmin]), enoxaparin (Lovenox), heparin, or warfarin
(Coumadin) are screened for bloody urine or stools.
ACTIVITY AND EXERCISE
As the nurse assesses the patient’s activity and exercise history, it is important to note that decreases in activity tolerance are typically gradual and may go unnoticed by the patient. Therefore, the nurse needs to determine whether there has been a change in the activ-ity pattern during the last 6 to 12 months. The patient’s subjec-tive response to activity is an essential assessment parameter. New symptoms or a change in the usual angina or angina equivalent during activity is a significant finding. Fatigue, associated with low ejection fraction and certain medications (eg, beta-blockers), can result in activity intolerance. Patients with fatigue may benefit from having their medications adjusted and learning energy con-servation techniques.
Additional
areas to ask about include possible architectural bar-riers and challenges in
the home, and what the patient does for exercise. If the patient exercises, the
nurse asks additional questions: What is the intensity, and how long and how
often is exercise per-formed? Has the patient ever participated in a cardiac
rehabilitation program? Functional levels are known to improve for almost all
pa-tients who participate in a cardiac rehabilitation program, and at-tendance
is highly recommended (Smith et al., 2001). Patients with disabilities may
require an individually tailored exercise program.
SLEEP AND REST
Clues
to worsening cardiac disease, especially HF, can be revealed by sleep-related
events. Determining where the patient sleeps or rests is important. Recent
changes, such as sleeping upright in a chair instead of in bed, increasing the
number of pillows used, awakening short of breath at night (paroxysmal
nocturnal dys-pnea [PND]), or awakening with angina (nocturnal angina), are all
indicative of worsening HF.
COGNITION AND PERCEPTION
Evaluating
cognitive ability helps to determine whether the pa-tient has the mental
capacity to manage safe and effective self-care. Is the patient’s short-term
memory intact? Is there any history of dementia? Is there evidence of
depression or anxiety? Can the patient read? Can the patient read English? What
is the patient’s reading level? What is the patient’s preferred learning style?
What information does the patient perceive as important?
Providing
the patient with written information can be a valu-able part of patient
education, but only if the patient can read and comprehend the information.
Related assessments include possi-ble hearing or visual impairments. If vision
is impaired, patients with HF may not be able to weigh themselves independently
nor keep records of weight, BP, pulse, or other data requested by the health
care team.
SELF-PERCEPTION AND SELF-CONCEPT
Personality
factors are associated with the development of and re-covery from CAD. Most
commonly cited is “type A behavior,” which is characterized by competitive,
hard-driving behaviors and a sense of time urgency. Although this behavior is not
an in-dependent risk factor for CAD, anger and hostility (personality traits
common in people with “type A behavior”) do affect the heart. People with these
traits react to frustrating situations with an increase in BP, heart rate, and
neuroendocrine responses. This physiologic activation, called cardiac
reactivity, is thought to trig-ger acute cardiovascular events (Woods et al.,
1999).
During
the health history, the nurse discovers how patients feel about themselves by
asking questions such as: How would you describe yourself? Have you changed the
way you feel about yourself since your heart attack or surgery? Do you find
that you are easily angered or hostile? How do you feel right now? What helps
to manage these feelings? To fully evaluate this health pat-tern, assistance
from a psychiatric clinical nurse specialist, psycho-logist, or psychiatrist
may be necessary.
ROLES AND RELATIONSHIPS
Determining
the patient’s social support systems is vitally im-portant in today’s health
care environment. Hospital stays for cardiac illnesses have shortened. Many
invasive diagnostic cardiac procedures, such as cardiac catheterization and
percutaneous transluminal coronary angioplasty (PTCA) are performed as
out-patient procedures. Patients are discharged back into the com-munity with
activity limitations, such as driving restrictions, and with greater nursing
care and educational needs. These needs have significant implications for
people who are independent under normal circumstances, and for people who are
at higher risk for problems, such as older adults.
To
assess support systems, the nurse needs to ask: Who is the primary caregiver?
With whom does the patient live? Are there adequate services in place to
provide a safe home environment? The nurse also assesses for any significant
effects the cardiac ill-ness has had on the patient’s role in the family. Are
there adequate finances and health insurance? The answers to these questions
will assist the nurse in developing a plan to meet the patient’s home care needs.
SEXUALITY AND REPRODUCTION
Although
people recovering from cardiac illnesses or procedures are concerned about
sexual activity, they are less likely to ask their nurse or other health care
provider for information to help them resume their normal sex life. Lack of
correct information and fear lead to reduced frequency and satisfaction with
sexual activity. Therefore, nurses need to initiate this discussion with
patients and not wait for them to bring it up in conversation. At first,
in-form the patient that it is common for people with similar heart problems to
worry about resuming sexual activity. Then ask the patient to talk about his or
her concerns.
The
most commonly cited reasons for changes in sexual ac-tivity are fear of another
heart attack or sudden death; untoward symptoms such as angina, dyspnea, or
palpitations; and problems with impotence or depression. In men, impotence may
develop as a side effect of cardiac medications (beta-adrenergic blocking
agents) and may prompt patients to stop taking them. Other medications can be
substituted, so patients should be encouraged to discuss this problem with
their health care provider. Often, patients and their partners do not have
adequate information about the physical demands related to sexual activity and
ways in which these demands can be modified. The physiologic demands are
greatest during orgasm, reaching 5 or 6 metabolic equivalents (METs). This
level of activity is equivalent to walking 3 to 4 miles per hour on a
treadmill. The METs expended before and after or-gasm are considerably less, at
3.7 METs (Steinke, 2000). Having this information may make patients and their
partners more com-fortable with resuming sexual activity.
A
reproductive history is necessary for women of childbearing age, particularly
those with seriously compromised cardiac func-tion. These women may be advised
by their physicians not to be-come pregnant. The reproductive history includes
information about previous pregnancies, plans for future pregnancies, oral
contraceptive use (especially in women older than 35 years of age who are
smokers), and use of hormone replacement therapy.
COPING AND STRESS TOLERANCE
It
is important to determine the presence of psychosocial factors that adversely
affect cardiac health. Anxiety, depression, and stress are known to influence
both the development of and recovery from CAD. High levels of anxiety are
associated with an increased incidence of CAD and increased in-hospital
complication rates after MI. People with depression have an increased risk of
MI-and heart disease–related death, compared to people without de-pression. It
is postulated that people who are depressed feel hope-less and are less
motivated to make lifestyle changes and follow treatment plans, explaining the
association between mortality and depression (Buselli & Stuart, 1999).
Stress
initiates a variety of physiologic responses, including in-creases in the
circulation of catecholamines and cortisol, and has been strongly linked to
cardiovascular events. Therefore, patients need to be assessed for presence of
negative and positive emo-tions, as well as sources of stress. This is achieved
by asking ques-tions about recent or ongoing stressors, previous coping styles
and effectiveness, and the patient’s perception of his or her current mood and
coping ability. To adequately evaluate this health pat-tern, consultation with
a psychiatric clinical nurse specialist, psy-chologist, or psychiatrist may be
indicated.
PREVENTION STRATEGIES
Additional
features of the health history include identification of risk factors and
measures taken by the patient to prevent disease. The nurse’s questions need to
focus on the patient’s health pro-motion practices. Epidemiologic studies show
that certain con-ditions or behaviors (ie, risk factors) are associated with a
greater incidence of coronary artery, peripheral vascular, and cerebrovas-cular
disease. Risk factors are classified by the extent to which they can be
modified by changing one’s lifestyle or modifying personal behaviors.
Once
a patient’s risk factors are determined, the nurse assesses whether the patient
has a plan for making necessary behavioral changes and whether assistance is
needed to support these lifestyle changes. For example, tobacco use is the most
common avoidable cause of CAD. The first step in treating this health risk is
to iden-tify patients who use tobacco products and those who have re-cently
quit. Because 70% of smokers visit a health care facility each year, nurses
have ample opportunities to assess patients for tobacco use. For those who use
tobacco, it is imperative to ask whether they are willing to quit. Provide
cessation advice, motivation to quit, and relapse prevention strategies, as
outlined in a U.S. Pub-lic Health Service report (The Tobacco Use and Dependence
Clinical Practice Guideline Update Panel, Staff, and Consortium
Representatives, 2000), can be delivered. For patients who have obesity,
hyperlipidemia, hypertension, and diabetes, the nurse de-termines any problems
the patient may be having following the prescribed management plan (ie, diet,
exercise, and medications). It may be necessary to clarify the patient’s
responsibilities, assist with finding additional resources, or make alternative
plans for risk factor modification.
Comprehensive
secondary prevention strategies (early diag-nosis and prompt intervention to
halt or slow the disease process and its consequences) aimed at reducing
cardiovascular risk fac-tors improve overall survival, improve quality of life,
reduce the need for revascularization procedures (coronary artery bypass
surgery and PTCA), and reduce the incidence of subsequent MIs. The overall
benefits of secondary prevention also apply to other patient groups with
atherosclerotic vascular disease, including pa-tients with transient ischemic
attacks, stroke, and peripheral vas-cular disease (the leading cause of
disability and death in these patients being CAD). Despite these findings, only
one third of eligible patients, over the long term, adhere to risk factor
inter-ventions. Patient compliance increases significantly with a team approach
that includes long-term follow-up with office or clinic visits and telephone
contact (Smith et al., 2001).
Related Topics