Chapter: Medical Surgical Nursing: Assessment of Cardiovascular Function
Assessment of Cardiovascular Function: Cardiac Auscultation - Physical Assessment
Cardiac Auscultation
All
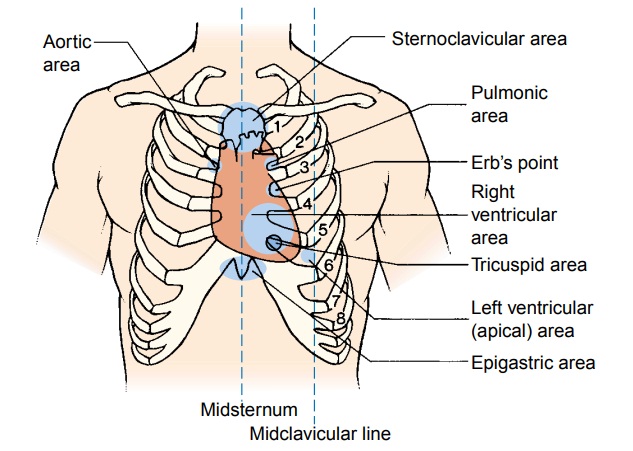
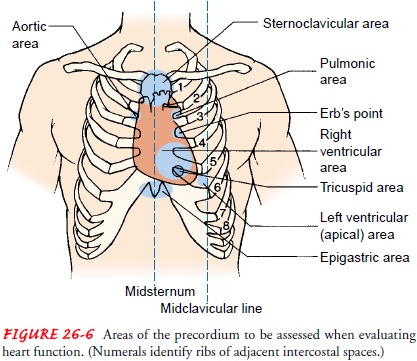
areas identified in Figure 26-6, except the epigastric area, are auscultated.
These include the aortic area, the pulmonary area, Erb’s point, the tricuspid
area, and the apical area. The actions of the four valves are uniquely
reflected at specific locations on the chest wall. These locations do not
correspond to the anatomic lo-cations of the valves within the chest; rather,
they reflect the pat-terns by which heart sounds radiate toward the chest wall.
Sound in vessels through which blood is flowing is always reflected downstream.
For example, the actions of the mitral valve are usu-ally heard best in the
fifth intercostal space at the midclavicular line. This is called the mitral
valve area.
HEART SOUNDS
The
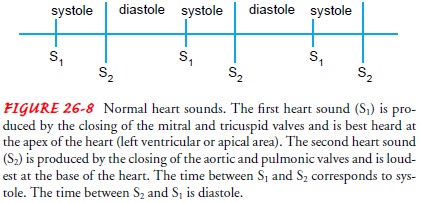
normal heart sounds, S1
and S2, are produced primarily by the
closing of the heart valves. The time between S1
and S2 cor-responds to systole (Fig.
26-8). This is normally shorter than the time between S2
and S1 (diastole). As the heart rate
increases, dias-tole shortens.
In
normal physiology, the periods of systole and diastole are silent. Ventricular
disease, however, can give rise to transient sounds in systole and diastole
that are called gallops, snaps, or clicks. Significant narrowing of the valve
orifices at times when they should be open, or residual gapping of valves at
times when they should be closed, gives rise to prolonged sounds called
murmurs.
S1—First Heart Sound. Closure of the mitral and tricuspid valvescreates the first heart sound (S1), although vibration of the myo-cardial wall also may contribute to this sound. Although S1 is heard over the entire precordium, it is heard best at the apex of the heart (apical area). Its intensity increases when the valve leaflets are made rigid by calcium in rheumatic heart disease and in any circumstance in which ventricular contraction occurs at a time when the valve is caught wide open. The latter circumstance occurs, for example, when a premature ventricular contraction in-terrupts the normal cardiac cycle. S1 varies in intensity from beat to beat when atrial contraction is not synchronous with ventric-ular contraction. This is because the valve may be fully or partially closed on one beat and open on the subsequent one as a function of irregular atrial activity. S1 is easily identifiable and serves as the point of reference for the remainder of the cardiac cycle.
S2—Second Heart Sound. Closing of the aortic
and pulmonicvalves produces the second heart sound (S2). Although these two valves close almost
simultaneously, the pulmonic valve usually lags slightly behind. Therefore,
under certain circumstances, the two components of the second sound may be
heard separately (split S2). The splitting is more likely to be accentuated on inspiration
and to disappear on exhalation. (More blood is ejected from the right ventricle
during inspiration than during exhalation.)
S2
is heard loudest at the base of the heart. The aortic compo-nent of S2
is heard clearly in both the aortic and pulmonic areas, and less clearly at the
apex. The pulmonic component of S2, if
present, may be heard only over the pulmonic area. Therefore, one may hear a
“single” S2 in the aortic area and a split S2
in the pulmonic area.
Gallop Sounds. If
the blood filling the ventricle is impededduring diastole, as occurs in certain
disease states, then a tem-porary vibration may occur in diastole that is
similar to, although usually softer than, S1 and S2. The heart sounds then come in triplets and have the acoustic
effect of a galloping horse; they are called gallops. This may occur early in
diastole, during the rapid-filling phase of the cardiac cycle, or later at the
time of atrial contraction.
A
gallop sound occurring during rapid ventricular filling is called a third heart
sound (S3); it represents a normal finding in
children and young adults (Fig. 26-9A). Such a sound is heard in patients who
have myocardial disease or in those who have HF and whose ventricles fail to
eject all of their blood during systole. An S3
gallop is heard best with the patient lying on the left side.
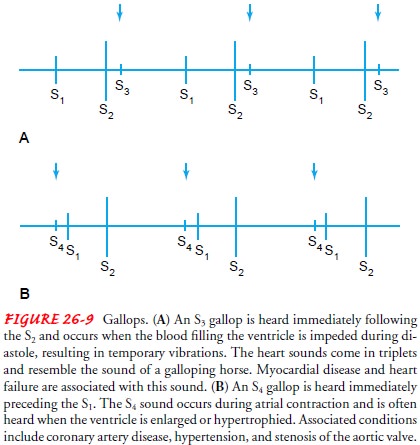
Gallop
sounds heard during atrial contraction are called fourth heart sounds (S4)
(see Fig. 26-9B). An S4 is often
heard when the ventricle is enlarged or hypertrophied and therefore resistant
to filling. Such a circumstance may be associated with CAD, hyper-tension, or
stenosis of the aortic valve. On rare occasions, all four heart sounds are
heard within a single cardiac cycle, giving rise to what is called a quadruple
rhythm.
Gallop
sounds are very low-frequency sounds and may be heard only with the bell of the
stethoscope placed very lightly against the chest. They are heard best at the
apex, although occa-sionally, when emanating from the right ventricle, they may
be heard to the left of the sternum.
Snaps and Clicks. Stenosis
of the mitral valve resulting fromrheumatic heart disease gives rise to an
unusual sound very early in diastole that is high-pitched and is best heard
along the left sternal border. The sound is caused by high pressure in the left
atrium with abrupt displacement of a rigid mitral valve. The sound is called an
opening snap. It occurs too long after S2 to be mistaken for a split S2 and too early in diastole to be mistaken for a gallop. It almost
always is associated with the murmur of mitral stenosis and is specific to this
disorder.
In
a similar manner, stenosis of the aortic valve gives rise to a short,
high-pitched sound immediately after S1
that is called an ejection click. This is caused by very high pressure within
the ven-tricle, displacing a rigid and calcified aortic valve.
Murmurs. Murmursare
created by the turbulent flow of blood.The causes of the turbulence may be a
critically narrowed valve, a malfunctioning valve that allows regurgitant blood
flow, a con-genital defect of the ventricular wall, a defect between the aorta
and the pulmonary artery, or an increased flow of blood through a normal
structure (eg, with fever, pregnancy, hyperthyroidism). Murmurs are
characterized and consequently described by several characteristics, including timing
in the cardiac cycle, location on the chest wall, intensity, pitch, quality,
and pattern of radiation (Chart 26-3).

Friction Rub. In
pericarditis, a harsh, grating sound that can beheard in both systole and
diastole is called a friction rub. It is caused by abrasion of the pericardial
surfaces during the cardiac cycle. Because a friction rub may be confused with
a murmur, care should be taken to identify the sound and to distinguish it from
murmurs that may be heard in both systole and diastole. A peri-cardial friction
rub can be heard best using the diaphragm of the stethoscope, with the patient
sitting up and leaning forward.
AUSCULTATION PROCEDURE
During
auscultation, the patient remains supine and the exam-ining room is as quiet as
possible. A stethoscope with a diaphragm and a bell is necessary for accurate
auscultation of the heart.
Using
the diaphragm of the stethoscope, the examiner starts at the apical area and
progresses upward along the left sternal bor-der to the pulmonic and aortic
areas. If desired, the examiner may choose to begin the examination at the
aortic and pulmonic areas and progress downward to the apex of the heart.
Initially, S1 is identified and evaluated with
respect to its intensity and splitting. Next, S2
is identified, and its intensity and any splitting are noted. After
concentrating on S1 and S2,
the examiner listens for extra sounds in systole and then in diastole.
Sometimes
it helps to ask the following questions: Do I hear snapping or clicking sounds?
Do I hear any high-pitched blowing sounds? Is this sound in systole, or
diastole, or both? The examiner again proceeds to move the stethoscope to all
of the designated areas of the precordium, listening carefully for these
sounds. Finally, the patient is turned on the left side and the stethoscope is
placed on the apical area, where an S3,
an S4, and a mitral murmur are more
readily detected.
Once an abnormality is heard, the entire chest surface is re-examined to determine the exact location of the sound and its radiation. Also, the patient, who may be concerned about the prolonged examination, must be supported and reassured. The auscultatory findings, particularly murmurs, are documented by identifying the following characteristics:
·
Location on chest wall.
·
Timing of sound as either during
systole or during diastole; described as early, middle, or late. (If heard
throughout the systole, the sound is often referred to as pansystolic or
holosystolic.)
·
Intensity of the sound (I, very
faint; II, quiet; III, moder-ately loud; IV, loud; V, very loud; or VI, heard
with stetho-scope removed from the chest).
·
Pitch, desrcribed as high, medium,
or low.
·
Quality of the sound, commonly
described as blowing, harsh, or musical.
·
Location of radiation of the sound
away from where it is heard the loudest.
INTERPRETATION OF CARDIAC SOUNDS
Interpreting
cardiac sounds requires detailed knowledge of car-diac physiology and the
pathophysiology of cardiac diseases. There are different levels of performance
at which the nurse may be expected to function. The first level is simply
recognizing that what one is hearing is not normal—such as a third heart sound,
a murmur in systole or diastole, a pericardial friction rub over the
midsternum, or a second heart sound that is widely split. These findings are
reported to the physician and acted on accordingly. This level of function is
useful in screening. It is the kind of ac-tivity involved in performing
physical examinations in schools on normal children or in performing routine
physical examinations or screening examinations.
The
second level involves recognizing patterns. The nurse cor-rectly observes the
findings and can recognize the constellation of sounds and the diagnostic
significance of common ones.
At
its most sophisticated level, cardiac diagnosis can be inter-pretive. Highly
skilled nurses can differentiate among dysrhyth-mias and respond accordingly.
They can determine the significance of the appearance and disappearance of
gallops during the treat-ment of patients who have had MIs or who have HF. This
is the role that the coronary care nurse and the cardiovascular advanced
practice nurse assume. They function with a team of other health care
professionals who have highly tuned skills of cardiovascular assessment and
diagnosis.
Inspection of the Extremities
The
hands, arms, legs, and feet are observed for skin and vascu-lar changes. The
most noteworthy changes include the following:
·
Decreased capillary refill time
indicates a slower peripheral flow rate from sluggish reperfusion and is often
observed in patients with hypotension or HF. Capillary refill time pro-vides
the basis for estimating the rate of peripheral blood flow. To test capillary
refill, briefly compress the nailbed so that it blanches, and then release the
pressure. Normally, reperfusion occurs within 3 seconds, as evidenced by the
re-turn of color.
·
Vascular changes from decreased
arterial circulation include decrease in quality or loss of pulse, discomfort
or pain, paresthesia, numbness, decrease in temperature, pallor, and loss of
movement. During the first few hours after invasive cardiac procedures (eg,
cardiac catheterization), affected ex-tremities should be assessed for vascular
changes frequently.
·
Hematoma, or a localized collection
of clotted blood in the tissue, may be observed in patients who have undergone
in-vasive cardiac procedures such as cardiac catheterization, PTCA, or cardiac
electrophysiology testing. Major blood vessels of the arms and legs are
selected for catheter insertion. During these procedures, systemic
anticoagulation with heparin is necessary, and minor or small hematomas may
occur at the catheter puncture site. However, large hematomas are a serious
complication that can compromise circulating blood volume and cardiac output,
requiring blood trans-fusions. All patients who have undergone these procedures
must have their puncture sites frequently observed until hemostasis is
adequately achieved.
·
Peripheral edema is fluid
accumulation in dependent areas of the body (feet and legs, sacrum in the
bedridden patient). Assess for pitting edema (a depression over an area of pres
sure) by pressing firmly for 5 seconds with the thumb over the dorsum of each
foot, behind each medial malleolus, and over the shins. Pitting edema is graded
as absent or as present on a scale from slight (1+ = 0 to 2
mm) to very marked (4+ = more than 8 mm). Peripheral edema is observed in pa-tients
with HF and in those with peripheral vascular diseases such as deep vein
thrombosis or chronic venous insufficiency.
·
Clubbing of the fingers and toes
implies chronic hemoglo-bin desaturation, as in congenital heart disease.
·
Lower extremity ulcers are observed
in patients with arte-rial or venous insufficiency.
Other Systems
LUNGS
Findings
frequently exhibited by cardiac patients include the following:
Tachypnea: Rapid,
shallow breathing may be noted in patientswho have HF or pain, and in those who
are extremely anxious.
Cheyne-Stokes respirations: Patients
with severe left ventricularfailure may exhibit Cheyne-Stokes breathing, a
pattern of rapid respirations alternating with apnea. It is important to note
the duration of the apnea.
Hemoptysis: Pink,
frothy sputum is indicative of acute pul-monary edema.
Cough: A dry,
hacking cough from irritation of small airways iscommon in patients with
pulmonary congestion from HF.
Crackles: HF
or atelectasis associated with bed rest, splintingfrom ischemic pain, or the
effects of pain medications and sedatives often results in the development of
crackles. Typically, crackles are first noted at the bases (because of
gravity’s effect on fluid accumulation and decreased venti-lation of basilar
tissue), but they may progress to all portions of the lung fields.
Wheezes: Compression
of the small airways by interstitial pul-monary edema may cause wheezing.
Beta-adrenergic block-ing agents (beta-blockers), such as propranolol
(Inderal), may precipitate airway narrowing, especially in patients with
underlying pulmonary disease.
ABDOMEN
For
the cardiac patient, two components of the abdominal ex-amination are
frequently performed.
Hepatojugular reflux: Liver
engorgement occurs because of de-creased venous return secondary to right
ventricular failure. The liver is enlarged, firm, nontender, and smooth. The
hepatojugular reflux may be demonstrated by pressing firmly over the right
upper quadrant of the abdomen for 30 to 60 seconds and noting a rise of 1 cm or
more in jugular venous pressure. This rise indicates an inability of the right
side of the heart to accommodate increased volume.
Bladder distention: Urine
output is an important indicator ofcardiac function, especially when urine
output is reduced. This may indicate inadequate renal perfusion or a less
seri-ous problem such as one caused by urinary retention. When the urine output
is decreased, the patient needs to be assessed for a distended bladder or
difficulty voiding. The bladder may be assessed with an ultrasound scanner or
the suprapubic area palpated for an oval mass and per-cussed for dullness,
indicative of a full bladder.
Gerontologic Considerations
When
performing a cardiovascular examination on an elderly patient, the nurse may
note such differences as more readily palpable peripheral pulses because of
increased hardness of the arteries and a loss of adjacent connective tissue.
Palpation of the precordium in the elderly is affected by the changes in the
shape of the chest. For example, a cardiac impulse may not be pal-pable in
patients with chronic obstructive pulmonary disease, because these patients
usually have an increased anterior-posterior chest diameter. Kyphoscoliosis, a
spinal deformity that occurs fre-quently in elderly patients, may dislocate the
cardiac apex down-ward so that the diagnostic significance of palpating the apical
impulse is obscured.
Systolic
BP increases with age, but diastolic BP usually plateaus after 50 years.
Medication therapy is usually initiated for high BP when consistent systolic
readings of 160 mm Hg or diastolic read-ings of 95 mm Hg are observed. For the
elderly patient, however, many factors are considered before initiating
treatment. Ortho-static hypotension may reflect a decreasing sensitivity of
postural reflexes, which must be considered when medication therapy is
prescribed.
An
S4 is heard in about 90% of elderly
patients; this is thought to be caused by decreased compliance of the left
ventri-cle. The S2 is
usually split. At least 60% of elderly patients have murmurs, the most common
being a soft systolic ejection mur-mur resulting from sclerotic changes of the
aortic leaflets (see Table 26-1).

Related Topics