Chapter: Medical Surgical Nursing: Assessment of Respiratory Function
Anatomy of the Lower Respiratory Tract: Lungs
ANATOMY OF THE LOWER RESPIRATORY TRACT: LUNGS
The lower respiratory tract consists of
the lungs, which contain the bronchial and alveolar structures needed for gas
exchange.
Lungs
The
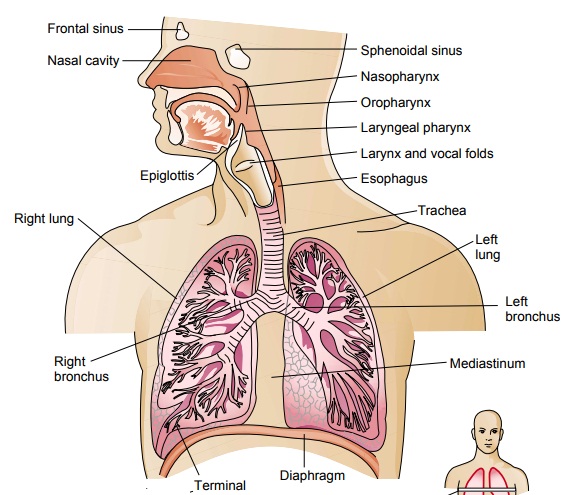
lungs are paired elastic structures enclosed in the thoracic cage, which is an
airtight chamber with distensible walls (Fig. 21-3). Ventilation requires
movement of the walls of the thoracic cage and of its floor, the diaphragm. The
effect of these movements is alter-nately to increase and decrease the capacity
of the chest. When the capacity of the chest is increased, air enters through
the trachea (in-spiration) because of the lowered pressure within and inflates
the lungs. When the chest wall and diaphragm return to their previous positions
(expiration), the lungs recoil and force the air out through the bronchi and
trachea. The inspiratory phase of respiration nor-mally requires energy; the
expiratory phase is normally passive. In-spiration occurs during the first
third of the respiratory cycle, expiration during the latter two thirds.
PLEURA
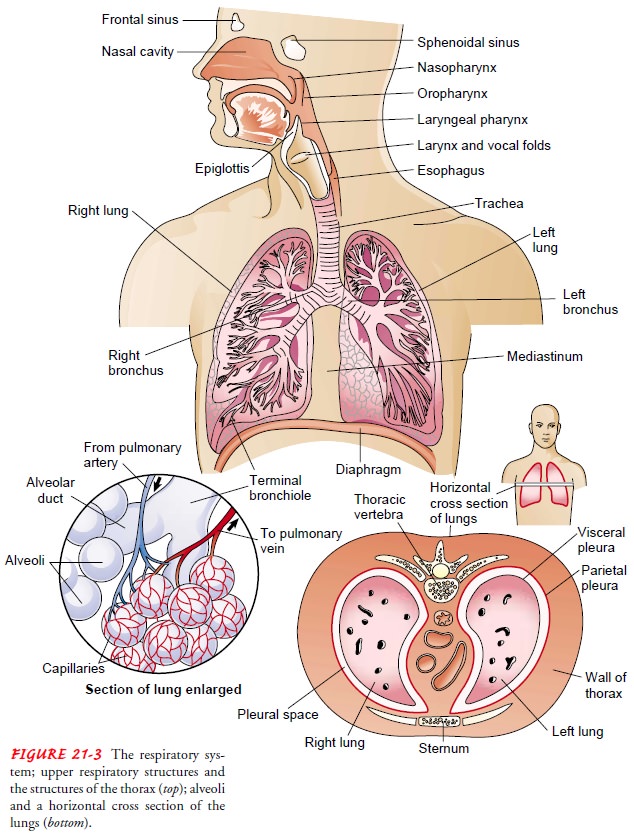
The lungs and wall of the thorax are
lined with a serous mem-brane called the pleura. The visceral pleura covers the
lungs; the parietal pleura lines the thorax. The visceral and parietal pleura
and the small amount of pleural fluid between these two mem-branes serve to
lubricate the thorax and lungs and permit smooth motion of the lungs within the
thoracic cavity with each breath.
MEDIASTINUM
The mediastinum is in the middle of the thorax, between the pleural sacs that contain the two lungs. It extends from the ster-num to the vertebral column and contains all the thoracic tissue outside the lungs.
LOBES
Each
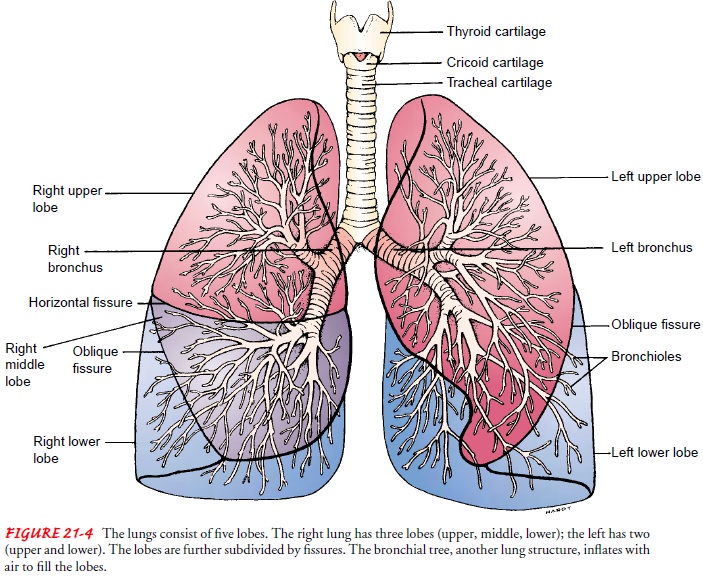
lung is divided into lobes. The left lung consists of an upper and lower lobe,
whereas the right lung has an upper, middle, and lower lobe (Fig. 21-4). Each
lobe is further subdivided into two to five segments separated by fissures,
which are extensions of the pleura.
BRONCHI AND BRONCHIOLES
There
are several divisions of the bronchi within each lobe of the lung. First are
the lobar bronchi (three in the right lung and two in the left lung). Lobar
bronchi divide into segmental bronchi (10 on the right and 8 on the left),
which are the structures iden-tified when choosing the most effective postural
drainage posi-tion for a given patient. Segmental bronchi then divide into
subsegmental bronchi. These bronchi are surrounded by con-nective tissue that
contains arteries, lymphatics, and nerves.
The
subsegmental bronchi then branch into bronchioles, which have no cartilage in
their walls. Their patency depends en-tirely on the elastic recoil of the
surrounding smooth muscle and on
the alveolar pressure. The bronchioles contain submucosal glands, which produce
mucus that covers the inside lining of the airways. The bronchi and bronchioles
are lined also with cells that have surfaces covered with cilia. These cilia
create a constant whipping motion that propels mucus and foreign substances
away from the lung toward the larynx.
The bronchioles then branch into
terminal bronchioles, which do not have mucous glands or cilia. Terminal
bronchioles then become respiratory bronchioles, which are considered to be the
transitional passageways between the conducting airways and the gas exchange
airways. Up to this point, the conducting airways contain about 150 mL of air
in the tracheobronchial tree that does not participate in gas exchange. This is
known as physio-logic dead space.
The respiratory bronchioles then lead into alve-olar ducts and alveolar sacs
and then alveoli. Oxygen and carbon dioxide exchange takes place in the
alveoli.
ALVEOLI
The lung is made up of about 300 million alveoli, which are arranged in clusters of 15 to 20. These alveoli are so numerous that if their surfaces were united to form one sheet, it would cover 70 square meters—the size of a tennis court.
There
are three types of alveolar cells. Type I alveolar cells are epithelial cells
that form the alveolar walls. Type II alveolar cells are metabolically active.
These cells secrete surfactant, a phos-pholipid that lines the inner surface
and prevents alveolar col-lapse. Type III alveolar cell macrophages are large
phagocytic cells that ingest foreign matter (eg, mucus, bacteria) and act as an
im-portant defense mechanism.
Related Topics