Chapter: Basic Radiology : The Physical Basis of Diagnostic Imaging
The Radiographic Image
The
Radiographic Image
For production of radiographic
images, the x-ray film is placed in a cassette and sandwiched between two
fluorescent screens that glow under x-ray exposure, and it is primarily the
light from these fluorescent screens that blackens the film. Although x-ray
film, which is quite similar to ordinary pho-tographic film, can be blackened
by direct x-ray exposure, the film does not absorb the penetrating x-rays very
efficiently, because the emulsion consists of silver halide crystals embed-ded
in a low-atomic-number gelatin base. The fluorescent screens, called
intensifying screens, are made of high-atomic-number materials, which therefore
absorb x-rays very efficiently and also emit hundreds of light photons per
x-ray absorbed. These light photons, in turn, are efficiently absorbed by the film.
As a result, x-ray exposure to the pa-tient is reduced by a factor on the order
of 100 compared to direct x-ray exposure of the film. The screens do produce a
loss of sharpness of the image due to the spreading out of the light from the
point of x-ray absorption before the light reaches the film. This effect can be
reduced by making the screen thinner; however, it then absorbs a smaller
fraction of the incident x-rays and therefore results in a “slower” system
(more patient exposure is required).
In recent years digital image
receptors have come into use. One type called CR (computed radiography)
utilizes a cas-sette with a photostimulable phosphor material that stores the
x-ray image in the form of trapped electrons for later readout by a scanned laser
beam, which releases the electrons from their traps. On release, these
electrons cause the phos-phor to emit light that has a shorter wavelength than
that of the laser beam. This light signal is read out and digitized, thereby
forming a digital image. Another type called DR (di-rect radiography) consists
of a flat-panel digital detector plate that is built into the x-ray unit
itself. In these, the x-ray image is converted to an electrical signal from a
fine matrix of thin-film transistor elements, which creates a digital image
having a pixel size of 0.2 mm or less. These digital images, which consist of
an array of numbers in a matrix, can be processed to improve image quality;
displayed and manipu-lated on a viewing monitor; and then printed onto film using
a laser film printer. The advantage of these digital systems is that the image
can be processed to improve contrast and pro-vide edge enhancement, and the
film can be printed to the appropriate darkness regardless of the x-ray
exposure.
Recall that the quantity of
x-rays produced during an ex-posure is proportional to
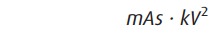
However, because the beam is more
penetrating at high kilo-voltage, the x-ray exposure that reaches the film
through a patient is roughly proportional to
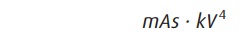
That is, it depends very strongly
on kilovoltage. The exposure time required to blacken the film is thus
proportional to
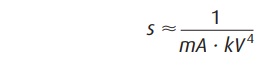
The heat deposited in the anode
is proportional to the prod-uct of kV and mAs.
Choice of an exposure technique
is generally made by first selecting the kilovoltage. A lower kilovoltage gives
greater image contrast but also higher patient exposure and requires a longer
exposure time at a given milliampere setting, because the x-ray beam is less
penetrating and x-ray production is lower at the lower kilovoltages. Thus, for
thick body parts, care must be taken not to choose too low a kilovoltage.
Generally, x-ray tubes have two
focal spot sizes produced by two different (selectable) filament sizes. That
is, they have a large and a small focal spot (eg, 1.25 and 0.6 mm). With the
small focal spot, however, the electron energy is deposited in a smaller area,
thereby creating a higher anode temperature; hence, at a given kilovoltage, the
maximum milliamperage that can be used without melting the anode is limited to
a lower value, thereby resulting in a longer exposure time. The small focal
spot will result in a sharper image, however, if the longer exposure time
required by its selection does not “stop” patient motion; then motion of the
patient during the expo-sure may blur out any sharpness gain realized by use of
the small focal spot. In any case, the small focal spot is useful only for
looking at fine detail, such as bony detail, and its use does not significantly
improve, for instance, an abdominal radi-ograph in which soft-tissue contrast
is the objective. The small focal spot might be used for radiographs of the
skull or extremities. The exposure time selected should be short enough to stop
the motion of the anatomic part being radi-ographed. A very short time would be
required for the heart and somewhat longer times for the abdomen or chest.
Expo-sure time is less critical for the head or extremities, which are not
subject to motion in most cases.
Having selected the kilovoltage and
exposure time, one must then select the milliamperage so that the
milliampere-seconds (the product of milliamperage and time) is large enough to
blacken the film suitably. If the milliamperage re-quired is above 200 mA to
300 mA, a small focal spot gener-ally cannot be used, because it will not allow
this high a value of milliamperage without melting the anode.
On many x-ray units, a phototimer
sensor (automatic ex-posure control) is used to automatically terminate the
expo-sure when a given x-ray exposure has been accumulated at the cassette
position. In this way, the film is blackened suffi-ciently regardless of
patient thickness and kilovoltage selec-tion. When using this feature, however,
the operator loses control of the exposure time. Choosing the highest
mil-liamperage allowable by the tube will ensure the minimum exposure time.
Related Topics