Chapter: Obstetrics and Gynecology: Assessment of Genetic Disorders in Obstetrics and Gynecology
Risk Factors For Genetic Disorders
RISK FACTORS FOR GENETIC DISORDERS
Several factors have been identified
that increase the risk of having a child with a chromosomal abnormality,
includ-ing maternal or paternal age and exposure to certain drugs. Other
factors, such as ethnicity or a family history of a disease, may indicate that
an individual carries a gene for a Mendelian disorder. The first step in
assessing risk is to document information about the patient’s family and
personal history (see Appendix 1, Antepartum Record). This record is an
effective method for obtaining informa-tion concerning personal and family
medical history, parental exposure to potentially harmful substances, or other
issues that may have an impact on risk assessment and management. This
information can be collected prior to conception during a preconception office
visit, or dur-ing the first prenatal visit in the first trimester.
Some infectious diseases,
including cytomegalovirus, rubella, and sexually transmitted diseases (see Infectious
Diseases in Pregnancy), as well as certain drugs (see Preconception and
Antepartum Care) have been linked to an increased risk of birth defects.
Preexisting diabetes mellitus may also predispose a fetus to a congenital
anomaly. Because these defects are not gene-based, family history and genetic
testing procedures, such as amniocen-tesis or CVS, cannot be used to detect
these abnormalities. Ultrasonography is the mainstay of surveillance for
infec-tious and teratogen-induced congenital abnormalities.
Advanced Maternal Age
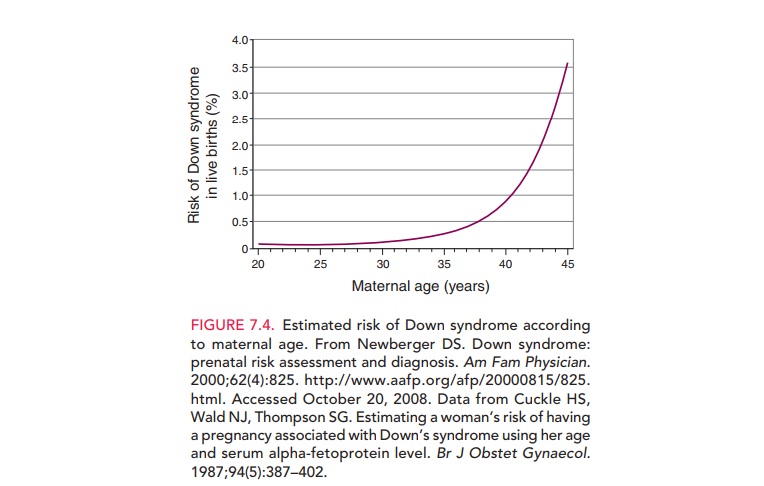
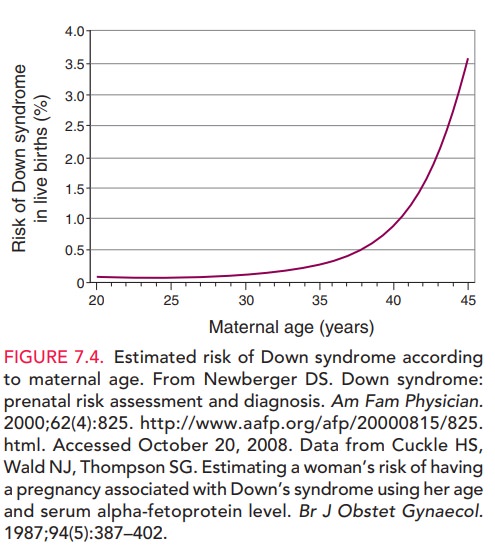
The incidence of trisomy 21 (Down
syndrome) among newborns of 35-year-old women is 1:385. Although the risk
increases with age, the majority of cases of Down syndrome occur in women
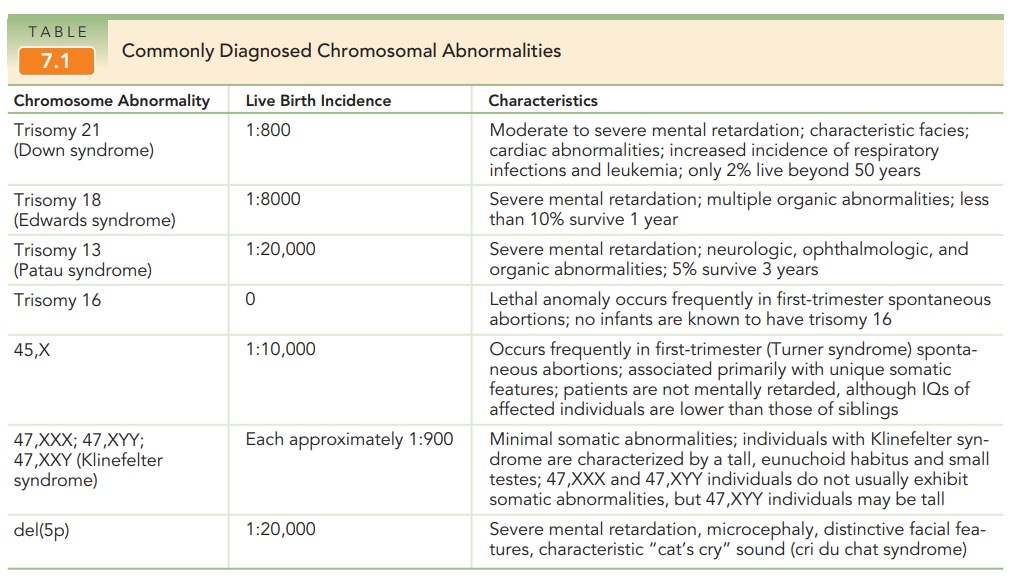
younger than 35 years of age (Fig. 7.4). In addition to Down syndrome, other
chromosomal abnor-malities increase in frequency with advanced maternal age
(see Table 7.1).
Previous Pregnancy Affected by Chromosomal Abnormality
Women who have had a previous
pregnancy complicated by trisomy 21, 18, or 13 or any other trisomy in which
the fetus survived at least to the second trimester, are at risk of having
another pregnancy complicated by the same or different trisomy. The risk of
trisomy recurrence is 1.6 to 8.2 times the maternal age risk, depending on
several factors: the type of trisomy, whether the index pregnancy was a
spontaneous abortion, maternal age at initial occurrence, and maternal age at
subsequent prenatal diagnosis.
Some, but not all, sex-chromosome
abnormalities carry an increased risk of recurrence. A pregnancy compli-cated
by fetal XXX or XXY increases the recurrence risk by 1.6% to 2.5% the maternal
age risk. Turner syndrome (monosomy X; XO) and XYY karyotypes impart a nominal
risk of recurrence.
History of Early Pregnancy Loss
At least half of all
first-trimester pregnancy losses result from fetal chromosomal abnormalities.
The most common are monosomy X; polyploidy (triploidy or tetraploidy); and
trisomies 13, 16, 18, 21, and 22.
Advanced Paternal Age
Increasing paternal age,
particularly after age 50 years, predisposes the fetus to an increase in gene
mutations that can affect X-linked recessive and autosomal dominant dis-orders,
such as neurofibromatosis, achondroplasia, Apert syndrome, and Marfan syndrome.
Ethnicity
Many Mendelian disorders occur
more frequently in cer-tain groups. African Americans are at increased risk of
sickle cell disease, the most common hemoglobinopathy in the United States.
Approximately 8% of African Americans carry the sickle hemoglobin gene, which
is also found with increased frequency in those of Mediterranean, Caribbean,
Latin American, or Middle Eastern descent. Caucasians of Northern European
descent are at increased risk of cystic fibrosis, with an estimated carrier
percentage of 1 in 22. Tay-Sachs, Gaucher, and Niemann-Pick diseases occur with
greater frequency in individuals of Ashkenazi Jewish descent. Other diseases
associated with certain ethnic groups are β-thalassemia, found at increased
frequency in individuals of Mediterranean origin and α-thalassemia in individuals of
Asian origin.
Related Topics