Chapter: Medical Surgical Nursing: Management of Patients With Upper Respiratory Tract Disorders
Rhinitis - Upper Airway Infections
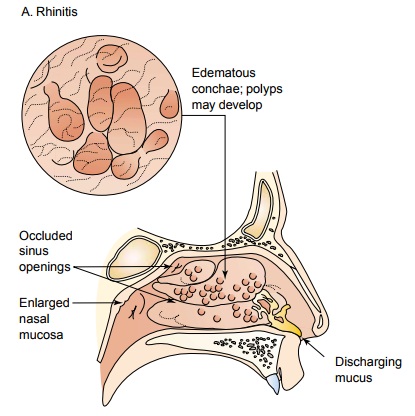
RHINITIS
Rhinitis is a group of disorders
characterized by inflammation and irritation of the mucous membranes of the
nose. It may be classified as nonallergic or allergic. It is estimated that 10%
to 15% of the population of the United States has allergic rhinitis
(Middletonet al., 1998). Rhinitis may be an acute or chronic condition.
Pathophysiology
Nonallergic rhinitis may be caused by a
variety of factors, including environmental factors such as changes in
temperature or humidity, odors, or foods; infection; age; systemic disease;
drugs (cocaine) or prescribed medications; or the presence of a foreign body.
Drug-induced rhinitis is associated with use of antihyper- tensive agents and
oral contraceptives and chronic use of nasal decongestants. Rhinitis also may
be a manifestation of an allergy, in which case it is referred to as allergic
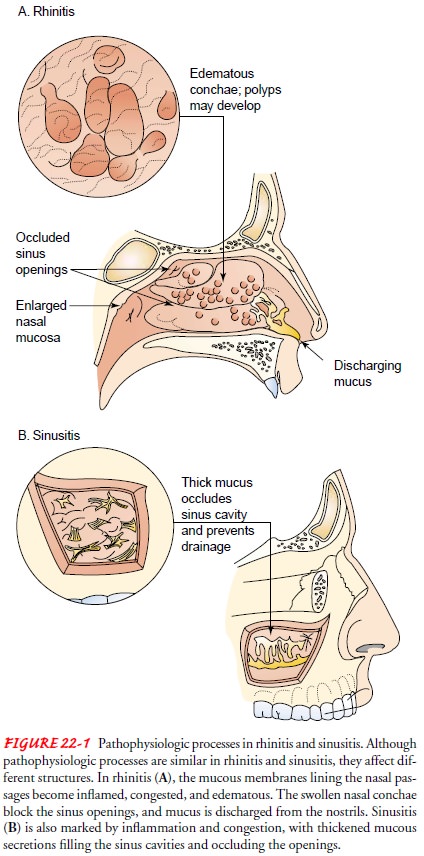
rhinitis.Figure 22-1 shows the pathological processes involved in rhinitis and
sinusitis.
Clinical Manifestations
The signs and symptoms of rhinitis
include rhinorrhea (excessive nasal drainage, runny nose), nasal congestion,
nasal discharge(purulent with bacterial rhinitis), nasal itchiness, and
sneezing. Headache may occur, particularly if sinusitis is also present
Medical Management
The management of rhinitis depends on
the cause, which may be identified in the history and physical examination. The
examiner asks the patient about recent symptoms as well as possible exposure to
allergens in the home, environment, or workplace. If viral rhinitis is the
cause, medications are given to relieve the symptoms. In allergic rhinitis,
tests may be performed to identify possible allergens. Depending on the
severity of the allergy, desensitizing immunizations and corticosteroids may be
required. If symptoms suggest a bacterial infection, an antimicrobial agent
will be used (see “Medical Management of Sinusitis”).
PHARMACOLOGIC THERAPY
Medication therapy for allergic and
nonallergic rhinitis focuses on symptom relief. Antihistamines are administered
for sneezing,itching, and rhinorrhea. Oral decongestant agents are used for
nasal obstruction. In addition, intranasal corticosteroids may be used for
severe congestion, and ophthalmic agents are used to relieve irritation, itching,
and redness of the eyes.
Nursing Management
TEACHING PATIENTS SELF-CARE
The nurse instructs the patient with allergic rhinitis to avoid or reduce exposure to allergens and irritants, such as dusts, molds, animals, fumes, odors, powders, sprays, and tobacco smoke. The patient is instructed about the importance of controlling the environment at home and work. Saline nasal or aerosol sprays may be helpful in soothing mucous membranes, softening crusted secretions, and removing irritants. The nurse instructs the patient in the proper use of and technique for administrating nasal medications. To achieve maximal relief, the patient is instructed toblow the nose before applying any medication into the nasal cavity. In the case of infectious rhinitis, the nurse reviews with the patient hand hygiene technique as a measure to prevent transmission of organisms. The nurse teaches methods to treat symptoms of the viral rhinitis. In the elderly and other highrisk populations, the nurse reviews the value of receiving a vaccination in the fall in order to achieve immunity prior to the beginning of the “flu season.”
Related Topics