Morphology, Pathogenesis, Animal Infection, Laboratory Diagnosis, Antirabic Vaccines, Passive Immunisation, Vaccines for Animals - Rabies Virus | 12th Microbiology : Chapter 10 : Medical Virology
Chapter: 12th Microbiology : Chapter 10 : Medical Virology
Rabies Virus
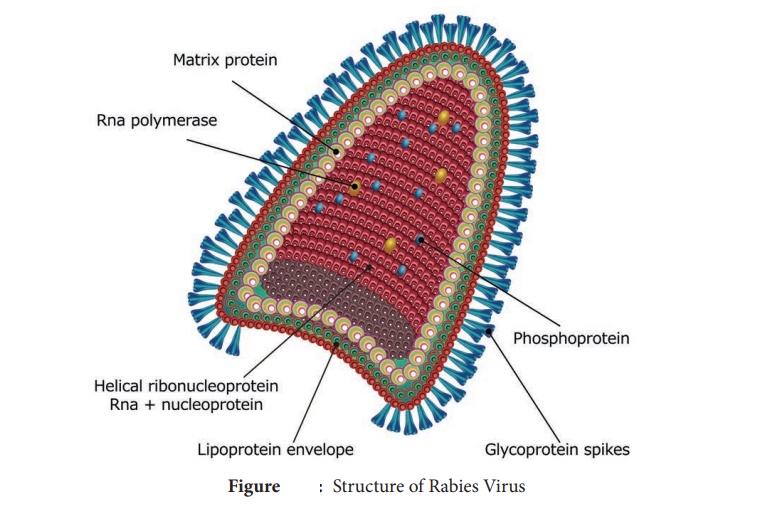
Rabies Virus
The
Family Rhabdoviridae contains viruses that infects
mammals, reptiles, birds, fishes,
insects and plants. The disease
in human being is called hydrophobia because
the patient exhibits fear of water,
being incapable of drinking though subject to intolerable thirst.
Pasteur established that the rabies virus was present in the brain
of infected animals. By serial intracerebral passage in rabbits, he
demonstrated fixed virus that could
be rendered immune by a series of
injections. Vaccine was prepared by drying pieces of spinal card from rabbits infected with
the fixed virus.
Joseph Meister a nine year old boy, severely bitten by a rabid dog and in
grave risk of developing rabies, was given a course of 13 inoculations of the infected cord vaccine by
Pasteur.
The boy survived. This dramatic event
was a mile stone in the development
of medicine.
Morphology
The
rabies virus is bullet shaped, with
one end rounded or conical and the other planar or concave. The lipoprotein
envelope, carries knob like spikes,
composed of glycoprotein G
responsible for pathogenesis, virulence and immunity beneath the envelope is
the matrix (M) protein layer which may be invaginated at the planar end. The membrane may project outwards forming a bleb. The genome is unsegmented linear
RNA (Figure 10.6).

The
rabies virus isolated from natural human or animal infection is termed ‘the street virus’. Rabies has been recognized from very ancient times as a disease transmitted to humans and
animals by the bite of ‘mad dogs’.
The name rabies comes from the Latin
word rabidus, meaning ‘mad’, derived
from the Sanskrit root rabhas, for frenzy
Pathogenesis
Human
infection is usually caused by the bite
of rabid dogs or other animals. The virus
present in the saliva of the animal is deposited
in the wound (Figure 10.7). Rarely,
infection can also occur following non-bite
exposures such as licks or aerosols.
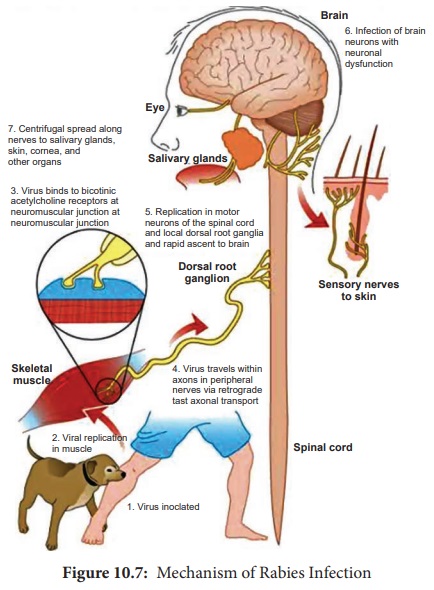
The virus
appears to multiply in the muscles,
connective tissue or nerves at the site of deposition for 48-72 hours. It
penetrates the nerve endings and
travels in the axoplasm towards the spinal
cord and brain , at speed of
about 3 mm per hour. The virus
multiples and spreads centrifugally along the nerve trunks to various parts of the body including
the salivary glands. It multiplies in the salivary glands and is shed in the saliva. The virus reaches every tissue in the body and
dissemination may be interrupted at any stage by death. In humans the
incubation period is usually from 1–3
months, short as 7 days or as long as three years. The incubation period is
usually short in persons bitten on the face or head and long in those bitten on
the legs. This may be related to the distance the virus has to travel to reach
the brain. The incubation period is generally shorter in children than in
adults.
The four stages of the disease are as
follows, prodrome, acute encephalitic
phase, coma and death. The onset is marked by symptoms such as fever,
headache, malaise, fatigue and anorexia, anxiety, agitation, irritability,
nervousness, insomnia or depression. The neurological phase begins with hyperactivity.
Attempts to drink during such painful spasms of the pharynx and larynx produce
choking or gagging that patients develop a dread of even the sight or sound of
water (hydrophobia).
Animal Infection
In dogs,
the incubation period is usually 3–6 weeks but it may range from 10 days to a year. The initial signs are an alert, troubled air and restlessness, snapping at imaginary objects, licking or
gnawing at the site of the bite.
After 2–3
days of this prodromal stage, the disease develops into either the furious or
dumb types of rabies. In furious rabies,
dog runs biting without provocation,
the lower jaw droops and saliva drools from the mouth. Paralysis convulsions
and death follow. In dumb rabies, is
the paralytic form, animals lies huddled,
unable to feed. About 60% of rabid dogs shed the virus in saliva. Rabid dogs
usually die in 3-5days
Laboratory Diagnosis
Human Rabies
The
specimens tested are corneal smears and skin biopsy. Commonly used method for diagnosis is the demonstration of rabies virus antigens by immuno fluorescence. Direct immunofluorescence is done using antirabies serum tagged with fluorescein isothiocyanate.
Negri bodies in the brain, are demonstrated, Isolation of the virus by intracerebral inoculation in mice can be attempted from the brain, CSF, saliva and urine. The mice are examined for signs of illness, and their brains are examined after death.
Animal Rabies
The whole carcass of the animal suspended
to have died of rabies may be sent to the laboratory. The brain may be removed sent for biological test and
microscopy respectively. The portion of brain sent should include the hippocampus and cerebellum as negri bodies are
most abundant. The following tests
are done in the laboratory.
1. Demonstration of rabies virus antigen by immuno
fluorescence
2. Demonstration
of inclusion bodies - Negri bodies are seen as intracytoplasmic, round or oval
purplish pink with characteristic basophilic inner granules. Negribodies vary
in size from 3.27 Mm.
Infobits
Local Treatment for rabies
• Prompt cauterization of the wounds helps to destroy the virus.
• Antirabic serum may be applied topically.
• Antitetanus measures and antibiotics to prevent sepsis.
Antirabic Vaccines
Antirabic
vaccines fall into two main categories neural and non-neural.
Neural Vaccines
Suspension’s
of nervous tissues of animals infected with the fixed rabies virus. Following
are the modified forms.
1. Semple
Vaccine: Vaccine developed by semple
(1911). It is a 5% suspension of sheep
brain infected with fixed virus and inactivated with phenol at 37°C leaving
noresidual live virus.
2. Beta
propiolactone (BPL) Vaccine: Beta propiolactone is used as the inactivating agent instead of Phenol.
3. Infant Brain Vaccine: The enceptalitogenic factor in brain
tissue is a basic protein associated with myelin. Vaccines were developed using
infant mouse, rat or rabbit brain. Infant brain vaccine is impractical in
India.
Non-neural Vaccines
Non-neural
vaccines includes
1. Egg
Vaccines
2. Tissue
Culture Vaccines
3. Subunit
Vaccine
Passive Immunisation
Human
rabies immune globulin (HRIG) is
free from the danger of sensitization but should be ensured free from HIV and
hepatitis viruses.
Vaccines for Animals
Antirabies immunization in
animals is to be done as pre
-exposure prophylaxis concentrated cell culture vaccines – inactivated virus
gives good protection after a single Intramuscular
injection. Injections are given at 12 weeks of age and repeated at 1–3 years
intervals.
Related Topics