Chapter: Paediatrics: Endocrinology and diabetes
Paediatrics: Hypocalcaemia
Hypocalcaemia
Most causes of low calcium
(hypocalcaemia) can be explained by abnor-malities of vitamin D or PTH
metabolism or by disordered kidney func-tion. The principal manifestations of
hypocalcaemia are related to neuro-muscular irritability and include tetany and
paraesthesiae.
· Hypocalcaemic seizures (grand-mal
type) or laryngeal spasm may occur acutely.
· Cardiac conduction abnormalities
(prolonged QT interval, QRS and ST changes, and ventricular arrhythmias) may be
seen.
Chronic hypocalcaemia may be
asymptomatic. The child’s age is helpful in determining the differential
diagnosis of hypocalcaemia.
Causes of hypocalcaemia
Early neonatal causes
· Prematurity
· Maternal diabetes
· Maternal pre-eclampsia
· RDS
Late neonatal causes
· Cow’s milk hyperphosphataemia
· Maternal hypercalcaemia
· Congenital hypoparathyroidism
Causes in infancy
· Nutritional rickets
· Pseudohypoparathroidism type 1a
Childhood causes
· Pseudohypoparathyroidism type 1b
· Hypoparathyroidism
Iatrogenic causes
· Chemotherapy agents, e.g.
cisplatin
· Anticonvulsant agents, e.g.
phenytoin
Investigations
· Plasma calcium.
· Plasma phosphate.
· Serum PTH. Note: Low or even normal PTH concentration implies failure of PTH
secretion.
· Plasma vitamin D.
· Plasma magnesium.
· X-ray of skull. Chronic
hypocalcaemia: basal ganglia calcification may be seen.
Treatment
Acute treatment
Chronic treatment
·Should be directed at the
underlying cause.
·Oral calcium supplements, together
with oral vitamin D therapy in the form of calcitriol (1-A calcidiol) are often required to
maintain plasma calcium levels within the normal range.
Hypoparathyroidism
Low serum parathyroid hormone
levels in childhood may be due to the following:
·Failure
in parathyroid development (agenesis/dysgenesis):
· isolated defect: X-linked
recessive;
· associated with other
abnormalities, e.g. DiGeorge syndrome, Kearnes–Sayre syndrome.
·Destruction
of parathyroid glands:
· autoimmune—type 1 autoimmune
polyendocrinopathy;
· surgery (post-thyroidectomy);
· radiotherapy.
·Failure
in PTH secretion: magnesium deficiency.
·Failure
in PTH action: pseudohypoparathyrodism.
Investigations
·Plasma
calcium: low.
·Plasma
phosphate: high.
·Serum
PTH: low.
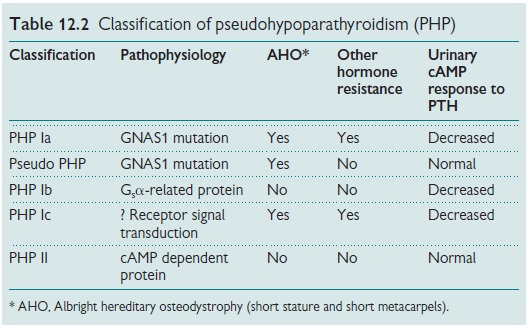
Pseudohypoparathyroidism (PHP)
Characterized by end-organ
resistance to the actions of PTH. It is a genet-ic disorder due to a defect in
the Gs A-adenylate
cyclase signalling system common to the PTH receptor and other endocrine
receptors belonging to the G protein-receptor family (e.g. TSH, LH, FSH). See
Table 12.2.
Related Topics