Chapter: Paediatrics: Community child health
Paediatrics: Health surveillance and promotion
Health surveillance and promotion
Disease prevention includes the
following:
•
Primary prevention: immunizations; accident
prevention; dental care.
•
Secondary prevention: screening for inherited
conditions.
•
Tertiary prevention: reducing impairments and
disabilities, e.g. hip dislocation in
CP, hypothyroidism and hearing problems in children with Down syndrome.
Primary prevention programmes
These are designed to reduce the
number of new cases of disease and disorder presenting within the community.
Examples of primary prevention programmes
•
Reducing
the incidence of infectious diseases—immunization programme
•
Reducing
the risk of sudden infant death
•
Reducing
parental smoking
•
Preventing
accidents and poisonings
•
Improving
nutrition—breastfeeding promotion
•
Preventing
dental disease
•
Promoting
child development
•
Preventing
child abuse
There is also a range of early
intervention programmes designed to pro-mote child development, reduce the risks
of child abuse and accidental injury, and improve parents’ mental health.
Children’s centres provide a variety of services to preschool children and
their families, and often are a base for different organizations and services.
Primary prevention programmes may
be aimed at parents and the family (e.g. poor housing, poverty, illness,
disability). Many programmes are also targeted towards at-risk groups (e.g. LBW
babies, mothers with postnatal depression, families living in poverty).
There are well established group
parenting support programmes on offer which focus on behaviour management
particularly. Some are intensively delivered by skilled professionals for
at-risk young first time mothers.3
Secondary prevention
These programmes reduce the prevalence
of disease. The Child Health Promotion Programme in the UK has been the remit
of the primary care team, and recent government guidance2 recommends
a much more focused universal approach, with additional services for those with
specific needs and risks
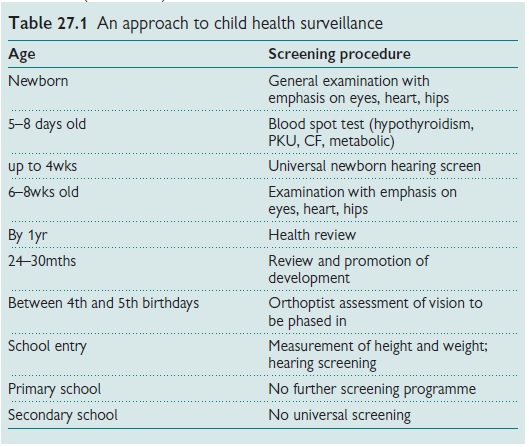
Antenatal screening is a very
important component of this, beginning in early pregnancy and is universal at
28wks gestation with an increased focus on those women at higher risk or
families requiring extra support or services.(Table 27.1).
Other opportunities for health
professional contact include immuniza-tions. Early detection of health problems
is achieved by:
•
Follow-up
of babies at risk (e.g. low birth weight, premature).
•
Follow-up
of children with neurological problems or post-trauma.
•
Targeted
observation or follow-up of children with a strong family history of genetic
disorders, e.g. hearing, vision, dislocated hips, learning difficulties,
familial hypercholesterolaemia.
•
Detection
by parents or health professionals (i.e. neglect).
•
Detection
by professionals in the course of their work (particularly playgroup,
nurseries, and schools, as well as health professionals).
Within each district the preschool
programme will vary according to what families need and will be targeted to
those who are ‘high risk’.
Particular concerns for preschool programmes
•
First
pregnancies and first time mothers
•
Isolated
mothers
•
Mother
with postnatal depression
· Unsupported, young parent living
in poverty
•
Domestic
violence; drug or alcohol abuse
•
Parents
with learning disability
•
Concern
about child neglect or abuse
•
Infant
with difficult feeding, sleeping, or temperament
•
Premature
baby or child who is disabled
•
Refugee
families
•
Smoking
(pregnancy or postnatal)
•
Obesity
in parents
Poor attachment and inconsistent
care
Related Topics