Chapter: Clinical Anesthesiology: Clinical Pharmacology: Neuromuscular Blocking Agents
Neuromuscular Blocking Agents: Mechanism Of Action
Distinctions Between Depolarizing & Nondepolarizing Blockade
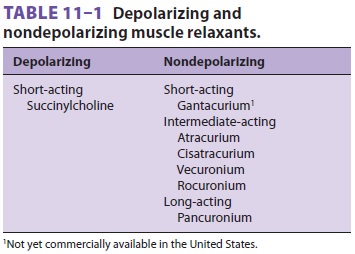
Neuromuscular blocking agents are
divided into two classes: depolarizing and nondepolarizing (Table 11–1).
This division reflects distinct dif-ferences in the mechanism of action,
response to peripheral nerve stimulation, and reversal of block.
MECHANISM OF ACTION
Similar to ACh, all neuromuscular blocking agents are quaternary ammonium compounds whose positively charged nitrogen imparts an affinity to nicotinic ACh receptors. Whereas most agents have two quaternary ammonium atoms, a few have one quaternary ammonium cation and one tertiary amine that is protonated at physiological pH.
Depolarizing muscle relaxants very
closely resemble ACh and readily bind to ACh receptors, generating a muscle
action potential. Unlike ACh, however, these drugs are not metabolized by ace-tylcholinesterase, and their concentration
in the synaptic cleft does not fall as rapidly, resulting in a prolonged
depolarization of the muscle end-plate.
Continuous end-plate depolarization
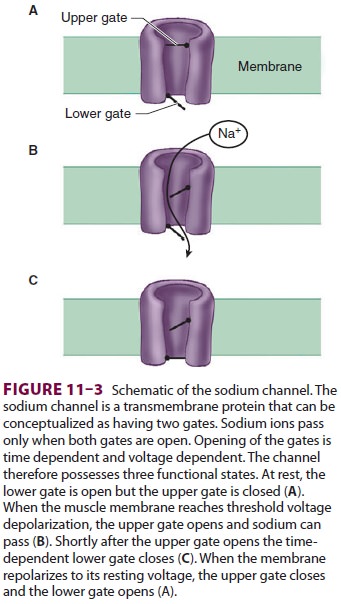
causes muscle relaxation because opening of perijunctional sodium channels is
time limited (sodium channels rapidly “inactivate” with continuing
depolarization) (Figure 11–3). After the initial excitation and open-ing
(Figure 11–3B), these sodium channels inacti-vate (Figure 11–3C) and cannot
reopen until the end-plate repolarizes. The end-plate cannot repolar-ize as
long as the depolarizing muscle relaxant con-tinues to bind to ACh receptors;
this is called a phase I block. After a period of time, prolonged end-plate
depolarization can cause poorly understood changes in the ACh receptor that
result in a phase II block, which clinically resembles that of nondepolarizing
muscle relaxants.
Nondepolarizing muscle relaxants bind
ACh receptors but are incapable of inducing the confor-mational change
necessary for ion channel opening. Because ACh is prevented from binding to its
recep-tors, no end-plate potential develops. Neuromuscular blockade occurs even
if only one α subunit is blocked. Thus, depolarizing muscle
relaxants act as ACh receptor agonists, whereas nondepolarizing muscle
relaxants function as competitive antago-nists. This basic difference in
mechanism of action explains their varying effects in certain disease states.
For example, conditions associated with a chronic decrease in ACh release (eg,
muscle denervation injuries) stimulate a compensatory increase in the number of
ACh receptors within muscle membranes. These states also promote the expression
of the imma-ture (extrajunctional) isoform of the ACh receptor, which displays
low channel conductance properties and prolonged open-channel time. This
up-regulation causes an exaggerated response to depolarizing mus-cle relaxants
(with more receptors being depolarized), but a resistance to nondepolarizing
relaxants (more receptors that must be blocked). In contrast, condi-tions
associated with fewer ACh receptors (eg, down-regulation in myasthenia gravis)
demonstrate a resistance to depolarizing relaxants and an increased sensitivity
to nondepolarizing relaxants.
Related Topics