Chapter: Medical Physiology: Cardiac Output, Venous Return, and Their Regulation
Low Cardiac Output
Low Cardiac Output
Figure 20–6 shows at the far right several conditions that cause abnormally low cardiac output. These conditions fall into two categories: (1) those abnormalities that cause the pumping effectiveness of the heart to fall too low and (2) those that cause venous return to fall too low.
Decreased Cardiac Output Caused by Cardiac Factors. When-ever the heart becomes severely damaged, regardless of the cause, its limited level of pumping may fall below that needed for adequate blood flow to the tissues. Some examples of this include (1) severe coronary blood vesselblockage and consequent myocardial infarction, (2) severe valvular heart disease, (3) myocarditis, (4) cardiac tamponade, and (5) cardiac metabolic derangements.
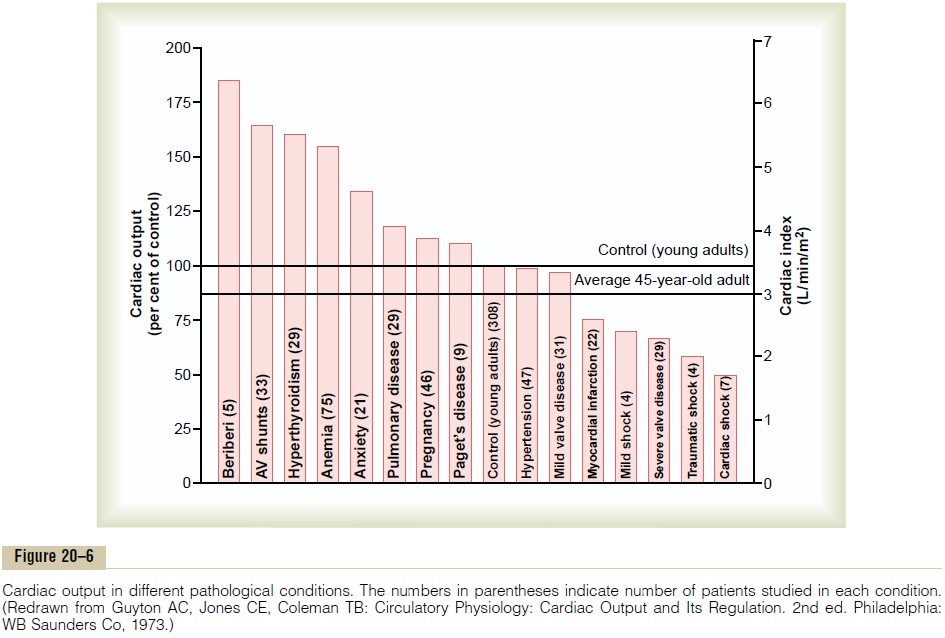
The effects of several of these are shown on the right in Figure 20–6, demonstrating the low cardiac outputs that result.
When the cardiac output falls so low that the tissues throughout the body begin to suffer nutritional defi-ciency, the condition is calledcardiac shock.
Decrease in Cardiac Output Caused by Non-cardiac Peripheral Factors—Decreased Venous Return. Anything that inter-feres with venous return also can lead to decreased cardiac output. Some of these factors are the following:
1. Decreased blood volume. By far, the mostcommon non-cardiac peripheral factor that leads to decreased cardiac output is decreased blood volume, resulting most often from hemorrhage.
It is clear why this condition decreases the cardiac output: Loss of blood decreases the filling of the vascular system to such a low level that there is not enough blood in the peripheral vessels to create peripheral vascular pressures high enough to push the blood back to the heart.
2. Acute venous dilation. On some occasions, theperipheral veins become acutely vasodilated. This results most often when the sympathetic nervous system suddenly becomes inactive. For instance, fainting often results from sudden loss of sympathetic nervous system activity, which causes the peripheral capacitative vessels, especially the veins, to dilate markedly. This decreases the filling pressure of the vascular system because the blood volume can no longer create adequate pressure in the now flaccid peripheral blood vessels. As a result, the blood “pools” in the vessels and does not return to the heart.
3. Obstruction of the large veins. On rare occasions,the large veins leading into the heart become obstructed, so that the blood in the peripheral vessels cannot flow back into the heart. Consequently, the cardiac output falls markedly.
4. Decreased tissue mass, especially decreased skeletal muscle mass. With normal aging or with prolongedperiods of physical inactivity, there is usually a reduction in the size of the skeletal muscles. This, in turn, decreases the total oxygen consumption and blood flow needs of the muscles, resulting in decreases in skeletal muscle blood flow and cardiac output.
Regardless of the cause of low cardiac output, whether it be a peripheral factor or a cardiac factor, if ever the cardiac output falls below that level required for adequate nutrition of the tissues, the person is said to suffer circulatory shock. This condition can be lethal within a few minutes to a few hours. Circulatory shock is such an important clinical problem.
Related Topics