Chapter: Microbiology and Immunology: Virology, Virus: Herpesviruses
Laboratory Diagnosis - Epstein Barr Virus Infections
Laboratory Diagnosis
The laboratory diagnosis of EBV-induced infectious mononucleosis is based on the three classic criteria:
· Presence of lymphocytosis.
· Presence of at least 10% atypical lymphocytes in peripheral blood smear.
· Presence of heterophilic antibodies and antibodies to viral antigens.
These criteria are supplemented by direct detection of viral antigens or EBV genomes in clinical specimens.
◗ Specimens
These include lymphoid tissues, nasopharyngeal carcinoma tissue and saliva (for direct detection of viral antigens or EBV genomes), and blood (for serological tests) and peripheral blood (for blood smear).
◗ Direct antigen detection
Direct immunofluorescent antibody using specific viral anti-bodies is used to detect EBV in clinical specimens.
◗ Isolation of the virus
EBV can be isolated from saliva, peripheral blood, or lym-phoid tissue by transformation of normal human lympho-cytes obtained from umbilical blood. However, the procedure is tedious and time-consuming, hence seldom used. Attempt has also been made to culture “spontaneously transformed” B lymphocytes from EBV DNA or virus-infected patients.
◗ Serodiagnosis
Epstein–Barr virus infection stimulates production of a wide range of antibodies including the heterophilic antibodies. These heterophilic antibodies are IgM antibodies that recog-nize Paul–Bunnell antigen on sheep, horse, and bovine RBCs. Therefore, serum from patients with acute mononucleosis agglutinates sheep, horse, or bovine erythrocytes.
Heterophile antibody test
Paul–Bunnell test: Paul–Bunnell test was first described byPaul and Bunnell for demonstration of heterophile antibodies in patients with infectious mononucleosis in 1932. This heterophile antibody, which is an IgM antibody, is not directed against EBV or EBV-infected cells, but is produced due to polyclonal activation of B cells by EBV. Such heterophilic antibodies are also found in serum sickness during drug reaction and naturally occurring antibodies to the Forssman antigen. These antibodies are absent or present in a very low titer in serum of healthy individuals.
The human blood to be tested is first absorbed by guinea pig kidney and then it is tested for agglutination activities that are directed against horse, sheep, or cow erythrocytes. The serum is inactivated at 56°C for 30 minutes and in dou-bling dilution is mixed with equal volume of a 1% suspension of sheep RBCs. The test is incubated at 37°C for 4 hours and is examined for agglutination. A serum titer of 100 or greater is considered a positive test and is suggestive of infectious mononucleosis.
Differential absorption of agglutinin with guinea pig and cow red cells is necessary for confirmation of the diagnosis. Cow RBCs absorb infectious mononucleosis heterophile anti-bodies from serum but not Forssman antibodies. Guinea pig kidney cells absorb Forssman antibodies, but not the infectious mononucleosis heterophile antibodies. Both guinea pig kidney cells and bovine RBCs absorb the antibodies produced in serum sickness. A serum titer of 1:100 after adsorption with guinea pig cells is considered positive and is suggestive of acute infectious mononucleosis.
The heterophile antibodies are present in serum of 40–60% of patients with infectious mononucleosis in the first week of illness and in 80–90% of cases by the third or fourth week. These heterophile antibodies are usually present for 3 months but may persist for even as long as a year.
Monospot test: Monospot test is a rapid slide agglutinationtest, which uses either horse RBCs or bovine RBCs. Bovine RBCs are more specific for acute infectious mononucleosis heterophile antibodies; hence they do not require differential absorption. Monospot test shows a specificity of 63–80%. It may show rare false positive reaction in patients with lymphoma or hepatitis.
EBV-specific antibody tests
Epstein–Barr virus infection is characterized by development of specific antibodies against different viral antigens, which appear during different stages of infection. Antibodies are pro-duced against viral capsid antigens (VCA), early antigens (EAs), and Epstein–Barr nuclear antigen (EBNAs). Viral capsid anti-gen and membrane antigens are produced late in the lytic cycle, whereas EBNA is expressed in the latently infected cells. EAs are always expressed early in the lytic cycle.
Indirect immunofluorescence test, ELISA, and Western blot are frequently used methods to detect antibodies against these antigens.
· Demonstration of IgM VCA antibodies as well as antibod-ies against EAs in the serum indicates current infection with EBV.
· Demonstration of IgG VCA antibodies indicates past infection.
· Demonstration of antibodies to EBNA antigens is also sug-gestive of past infection.
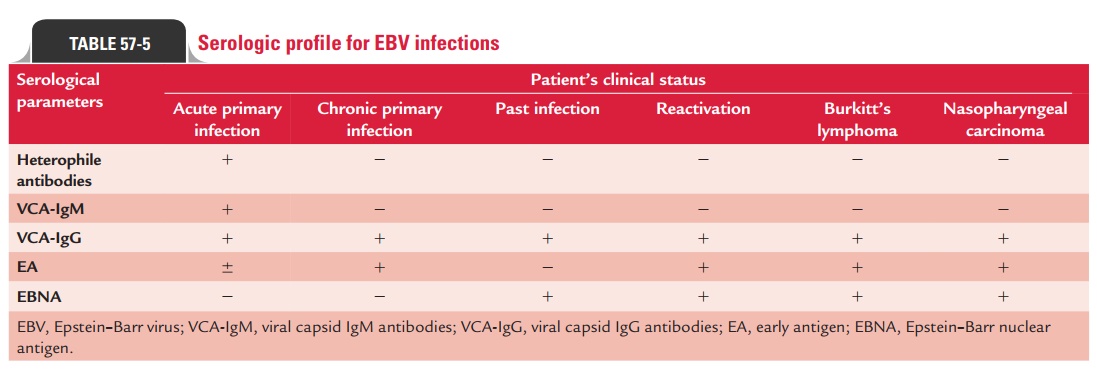
Serological profile of EBV infections is summarized in Table 57-5.
◗ Other tests
Complete blood count: Presence of atypical lymphocytesis the characteristic feature of infection with EBV. Usually 20–40% of lymphocytes are atypical. These atypical lympho-cytes of Downy type III are larger and have a less dense mucus than normal lymphocytes. Lymphocytosis (more than 50% lymphocytes) is seen in approximately 80–90% of patients. Lymphocytosis is well marked during the second or third week of illness and persists for 2–6 weeks.
Related Topics