Chapter: Microbiology and Immunology: Virology, Virus: Herpesviruses
Clinical Syndromes - Herpes Simplex Virus
Clinical Syndromes
Herpes simplex virus causes a wide variety of clinical manifes-tations. The clinical manifestations depend on (a) the age of patient, (b) immune status of the host, (c) previous immunity of the patient to autologous or heterologous viruses, (d) anti-genic type of the virus, and (e) anatomical site of involvement.
Generally, HSV-1 produces the lesions above the waist, and HSV-2 produces lesions below the waist. HSV-1 infection is normally associated with orofacial infections and encephalitis, whereas HSV-2 is associated with genital infections. Primary infection with either virus is typically associated with systemic signs, prolonged duration, increased severity of illness, and more complications.
◗ HSV-1 infections
HSV-1 can cause a wide variety of clinical entities. These include (a) acute herpetic gingivostomatitis, (b) acute herpetic pharyngotonsillitis, (c) herpes labialis, (d) herpes encephalitis, (e) eczema herpeticum, and (f) herpetic whitlow.
Acute herpetic gingivostomatitis: Acute herpetic gingivosto-matitis is the manifestation of primary HSV-1 infection occurring in children between 6 months and 5 years. Saliva from infected child or an adult is the source of infection. This condition has an incubation period of 3–6 days. The condition has an abrupt onset with high temperature. Gingivitis is the most impor-tant manifestation with marked lip swelling and erythematous and friable gums. Vesicular lesions appear on the oral mucosa, tongue, and lips. These lesions subsequently rupture and coalesce together, leaving behind ulcerated plaques. The acute disease lasts for 5–7 days, and the symptoms subside in 2 weeks. Viral sheddings from the saliva may continue for 3 weeks or more.
Acute herpetic pharyngotonsillitis: HSV-1 causes pharyngi-tis and tonsillitis in adults more frequently than gingivostoma-titis. The condition manifests as fever, malaise, headache, and sore throat. The vesicular lesions on the tonsils and the pos-terior pharynx usually rupture to form ulcers. Associated oral and labial lesions can be found in less than 10% of the patients.
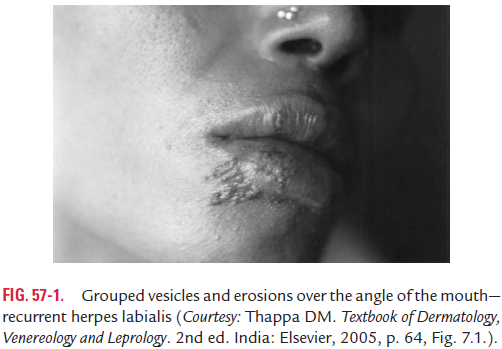
Herpes labialis: Herpes labialis is the most common clinicalmanifestation of recurrent HSV-1 infection (Fig. 57-1, Color Photo 56). Pain, burning, and tingling sensation at the site of infection are presenting features. An intraepidermal vesicle that later becomes pustular and ulcerate is the typical lesion. Usually, two or less recurrences manifest each year in most patients. But in some patients, even monthly recurrence is seen.
Herpes encephalitis: Herpes encephalitis is an acutefebrile disease that is usually caused by HSV-1. This may be a manifestation of primary or recurrent infection with the virus. The infection may have an insidious or an abrupt onset. Focal neurological manifestations, such as seizures, hemiparesis, aphasia, and paresthesia may be seen during acute condition. In some patients, the infection may rapidly progress from stupor to coma to death, without having any localized neurological symptoms.
Eczema herpeticum: Eczema herpeticum is seen in childrenwith active eczema. The vesicular lesions appear briefly on previ-ous eczematous areas with extensive ulceration. Subsequently, the infection may be disseminated by blood to the adrenal glands, liver, and other organs, resulting in fatal consequences.
Herpetic whitlow: Herpetic whitlow is an infection of thefinger caused by entry of the virus through cuts or abrasions on the skin. The condition often occurs in doctors and nurses who are exposed to patients with HSV infection and to patients who have genital infection. The vesicular lesions are usually produced on the skin of the finger but may also be seen on the skin of the head and neck.
◗ HSV-2 infections
HSV-2 causes (a) genital herpes, (b) neonatal infection, and (c) aseptic meningitis.
Genital herpes: Genital herpes is mostly caused by HSV-2 butcan also be caused by HSV-1. The latter causes less than 10% of genital infections. Most primary genital infections are asymp-tomatic. The clinical manifestations of primary genital herpes caused by HSV-1 and HSV-2 are similar, but recurrences are more common with HSV-2.
In symptomatic men, the herpetic vesicles appear in the glans penis, the prepuce, shaft of the penis, and sometimes on the scrotum, thighs, and buttocks. Herpetic proctitis involv-ing the perianal area and rectum are seen in the persons who engage in anal intercourse. In women, the vesicles appear on the external genitalia, labia majora, labia minora, vaginal vesti-bule, and introitus. The vesicles subsequently rupture, leaving behind extremely painful ulcers. Cervicitis, urethritis, and dys-uria may also be present in some women.
In both men and women, the primary infection may be asso-ciated with constitutional symptoms, such as fever, headache, malaise, and myalgia. In both the sexes, the ulcerative lesions persist from 4 to 15 days until crusting and re-epithelization occur. The virus continues to shed in the ulcerative lesions for more than 12 days.
Recurrent genital herpes are more common with HSV-2 as compared to HSV-1. The condition is shorter in duration and less severe than the primary genital herpes. Recurrent genital herpes in men may present as one or more numbers of clustered vesicles on the shaft of the penis, prepuce, or glans. Relatively, pain is mild and urethritis is uncommon. The lesions heal in 7–10 days. In women, the vesicular lesions are found on the labia majora, labia minora, or perineum. These lesions are very painful. Fever and constitu-tional symptoms are uncommon. The lesions heal in 8–10 days.
Neonatal infection: Neonatal infection is a most serious andusually fatal disease caused mostly by HSV-2. It usually occurs due to shedding of HSV-2 from the cervix during vaginal deliv-ery. It can also occur from an ascending in-utero infection dur-ing a primary infection of the mother. The infection can also be acquired postnatally from family members or hospital staff.
Since CMI is poorly developed in neonates, the virus causes a disseminated disease with involvement of liver, lung, as well as the organs of the CNS. The condition has a high mortality of 80%. Progression of the infection to the CNS results in mental retardation or neurological disabilities even with treatment, or may finally lead to death.
Aseptic meningitis: Aseptic meningitis may occur as a com-plication of genital HSV-2 infection.
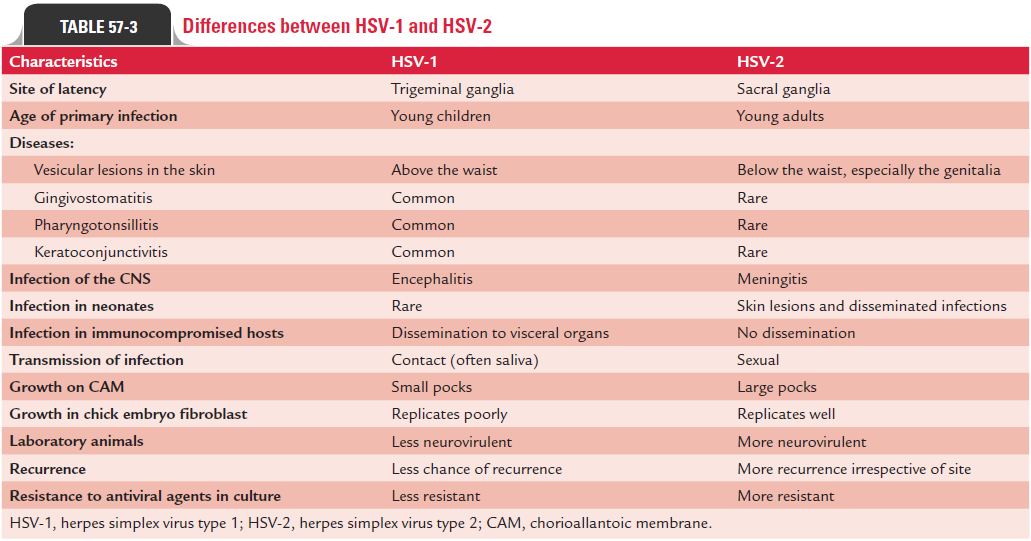
Differences between HSV-1 and HSV-2 infections are sum-marized in Table 57-3.
Related Topics