Chapter: 11th Zoology : Chapter 7 : Body Fluids and Circulation
Human circulatory system
Human
circulatory system
The
structure of the heart was described by Raymond de viessens, in 1706. Human
heart is made of special type of muscle called the cardiac muscle. It is
situated in the thoracic cavity and its apex portion is slightly tilted towards
left. It weighs about 300g in an adult. The size of our heart is roughly equal
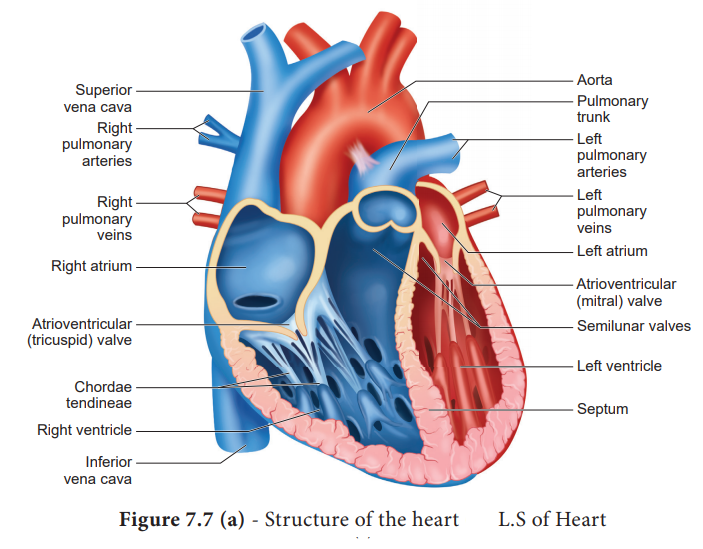
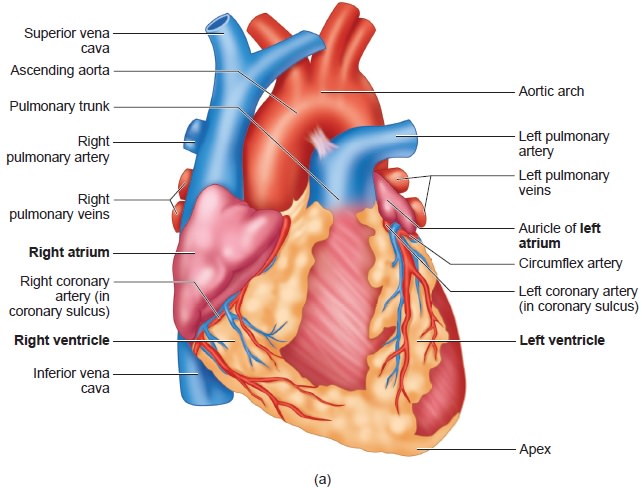
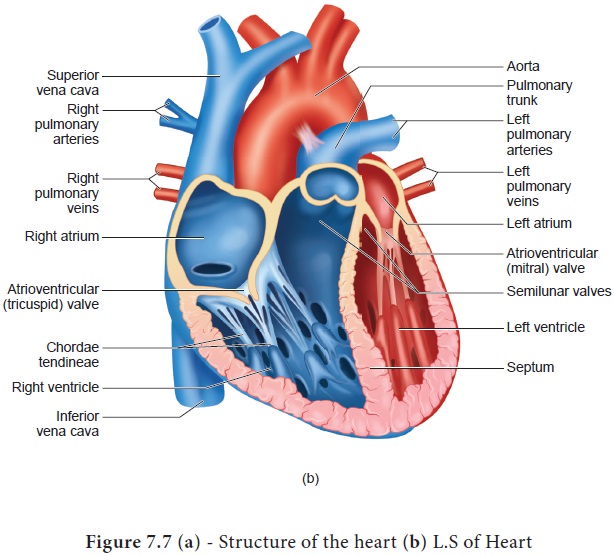
to a closed fist. The structure of heart and the L.S of
heart are shown in Figure 7.7 (a) and (b). Heart is divided into four chambers,
upper two small auricles or atrium and lower two large ventricles. The walls of
the ventricles are thicker than the auricles due to the presence of -papillary
muscles. The heart wall is made up of three layers, the outer epicardium,
middle myocardium and inner endocardium. The space present between the
membranes is called pericardial space and is filled with pericardial fluid.
The two
auricles are separated by inter auricular septum and the two ventricles are
separated by inter ventricular septum The separation of chambers avoids
mixing of oxygenated and deoxygenated blood. The auricle communicates with the
ventricle through an opening called auriculo ventricular aperture which is
guarded by the auriculo ventricular valves. The opening between the right
atrium and the right ventricle is guarded by the tricuspid valve (three flaps or cusps), whereas a bicuspid (two flaps or cusps) or mitral valve guards the opening between
the left atrium and left ventricle. The valves of the heart allows the blood to
flow only in one direction, i.e., from the atria to the ventricles and from the
ventricles to the pulmonary artery or the aorta. These valves prevent backward
flow of blood.
The
opening of right and left ventricles into the pulmonary artery and aorta are
guarded by aortic and pulmonary valves and are called semilunar valves. Each semilunar valve is made of three half-moon
shaped cusps. The myocardium of the ventricle is thrown into irregular muscular
ridges called trabeculae corneae.
The trabeculae corneae are modified into chordae
tendinae. The opening and closing of the semilunar valves are achieved by
the chordae tendinae. The chordae tendinae are attached to the lower end of the
heart by papillary muscles. Heart receives deoxygenated blood from various
parts of the body through the inferior venacava and superior venacava which
open into the right auricle. Oxygenated blood from lungs is drained into the
left auricle through four pulmonary veins.
1. Origin and conduction of heart beat
The heart
in human is myogenic (cardiomyocytes can produce spontaneous rhythmic
depolarisation that initiates contractions). The sequence of electrical
conduction of heart is shown in Figure 7.8. The cardiac cells with fastest
rhythm are called the Pacemaker cells, since they determine the contraction
rate of the entire heart. These cells are located in the right sinuatrial (SA)
node/ Pacemaker. On the left side of the right atrium is a node called auriculo
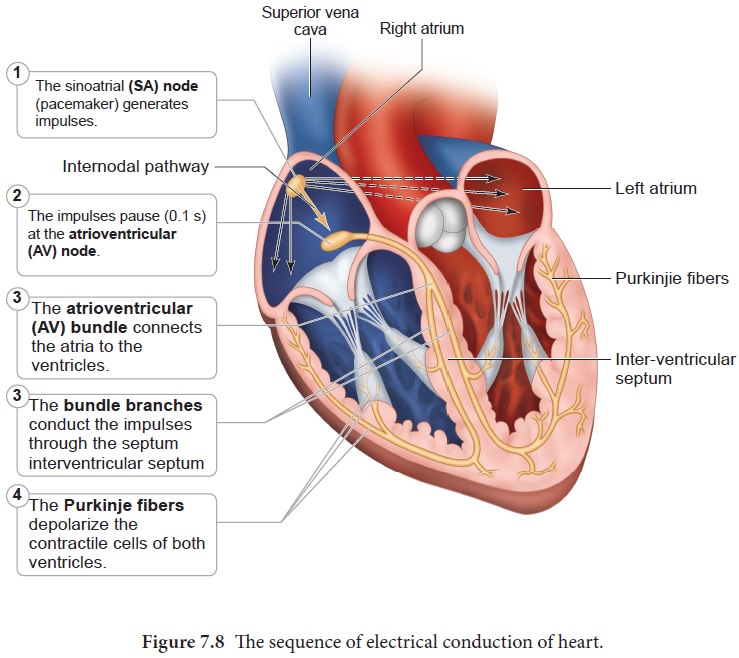
Two special cardiac muscle fibres originate from the auriculo
ventricular node and are called the bundle of His which runs down into the
interventricular septum and the fibres spread into the ventricles. These fibres
are called the Purkinje fibres.
Pacemaker
cells produce excitation through depolarisation of their cell membrane. Early
depolarisation is slow and takes place by sodium influx and reduction in
potassium efflux. Minimumpotential is required to activate voltage gated
calcium (Ca+) channels that causes rapid depolarisation which
results in action potential. The pace maker cells repolarise slowly via K+
efflux.
HEART
BEAT- Rhythmic contraction and expansion of heart is called heart beat. The
contraction of the heart is called systole
and the relaxation of the heart is called diastole.
The heart normally beats 70-72 times per min in a human adult. During each cardiac cycle two sounds
The first heart sound (lub) is associated with the closure of the tricuspid and
bicuspid valves whereas second heart sound (dub) is associated with the closure
of the semilunar valves. These sounds are of clinical diagnostic significance.
An increased heart rate is called tachycardia and decreased heart rate is
called bradycardia.
2. Cardiac Cycle
The events that occur at the beginning of heart beat and lasts until the beginning of next beat is called cardiac cycle. It lasts for 0.8 seconds. The series of events that takes place in a cardiac cycle.
PHASE 1:
Ventricular diastole- The pressure in the auricles increases than that of the
ventricular pressure. AV valves are open while the semi lunar valves are
closed. Blood flows from the auricles into the ventricles passively.
PHASE 2:
Atrial systole - The atria contracts while the ventricles are still relaxed.
The contraction of the auricles pushes maximum volume of blood to the
ventricles until they reach the end diastolic volume (EDV). EDV is related to
the length of the cardiac muscle fibre. More the muscle is stretched, greater
the EDV and the stroke volume.
PHASE 3:
Ventricular systole (isovolumetric contraction) - The ventricular contraction
forces the AV valves to close and increases the pressure inside the ventricles. The blood is then pumped from the ventricles into
the aorta without change in the size of the muscle fibre length and ventricular
chamber volume (isovolumetric contraction).
PHASE 4:
Ventricular systole (ventricular ejection) - Increased ventricular pressure
forces the semilunar valves to open and blood is ejected out of the ventricles
without backflow of blood. This point is the end of systolic volume (ESV).
PHASE 5:
(Ventricular diastole) -The ventricles begins to relax, pressure in the arteries
exceeds ventricular pressure, resulting in the closure of the semilunar valves.
The heart returns to phase 1 of the cardiac cycle.
3. Cardiac output
The
amount of blood pumped out by each ventricle per minute is called cardiac
output(CO). It is a product of heart rate (HR) and stroke volume (SV). Heart
rate or pulse is the number of beats per minute. Pulse pressure = systolic
pressure– diastolic pressure. Stroke volume (SV) is the volume of blood pumped
out by one ventricle with each beat. SV depends on ventricular contraction. CO
= HR X SV. SV represents the difference between EDV (amount of blood that
collects in a ventricle during diastole) and ESV (volume of blood remaining in
the ventricle after contraction). SV = EDV - ESV. According to Frank – Starling
law of the heart, the critical factor controlling SV is the degree to which the
cardiac muscle cells are stretched just before they contract. The most
important factor stretching cardiac muscle is the amount of blood returning to
the heart and distending its ventricles, venous return. During vigorous
exercise, SV may double as a result of venous return. Heart’s pumping action
normally maintains a balance between cardiac output and venous return. Because
the heart is a double pump, each side can fail independently of the other. If
the left side of the heart fails, it results in pulmonary congestion and if the
right side fails, it results in peripheral congestion. Frank – Starling effect
protects the heart from abnormal increase in blood volume.
Blood Pressure
Blood
pressure is the pressure exerted on the surface of blood vessels by the blood.
This pressure circulates the blood through arteries, veins and capillaries.
There are two types of pressure, the systolic pressure and the diastolic pressure.
Systolic pressure is the pressure in the arteries as the chambers of the heart
contracts. Diastolic pressure is the pressure in the arteries when the heart
chambers relax. Blood pressure is measured using a sphygmomanometer (BP
apparatus). It is expressed as systolic pressure / diastolic pressure. Normal
blood pressure in man is about 120/80mm Hg. Mean arterial pressure is a
function of cardiac output and resistance in the arterioles. The primary reflex
pathway for homeostatic control of mean arterial pressure is the baroreceptor
reflex. The baroreceptor reflex functions every morning when you get out of bed. When you are lying flat the gravitational force is
evenly distributed. When you stand up, gravity causes blood to pool in the
lower extremities. The decrease in blood pressure upon standing is known as
orthostatic hypotension. Orthostatic reflex normally triggers baroreceptor
reflex. This results in increased cardiac output and increased peripheral
resistance which together increase the mean arterial pressure.
4. Electrocardiogram (ECG)
An
electrocardiogram (ECG) records the electrical activity of the heart over a
period of time using electrodes placed on the skin, arms, legs and chest. It
records the changes in electrical potential across the heart during one cardiac
cycle. The special flap of muscle which initiates the heart beat is called as
sinu-auricular node or SA node in the right atrium. It spreads as a wave of
contraction in the heart. The waves of the ECG are due to depolarization and
not due to contraction of the heart. This wave of depolarisation occurs before
the beginning of contraction of the cardiac muscle. A normal ECG shows 3 waves
designated as P wave, QRS complex and T wave as shown in Figure 7.9 and the
stages of the ECG graph are shown in Figure 7.10.
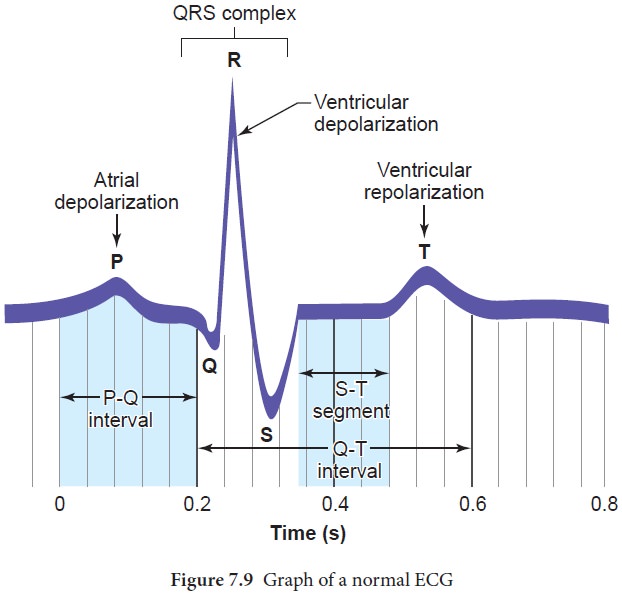
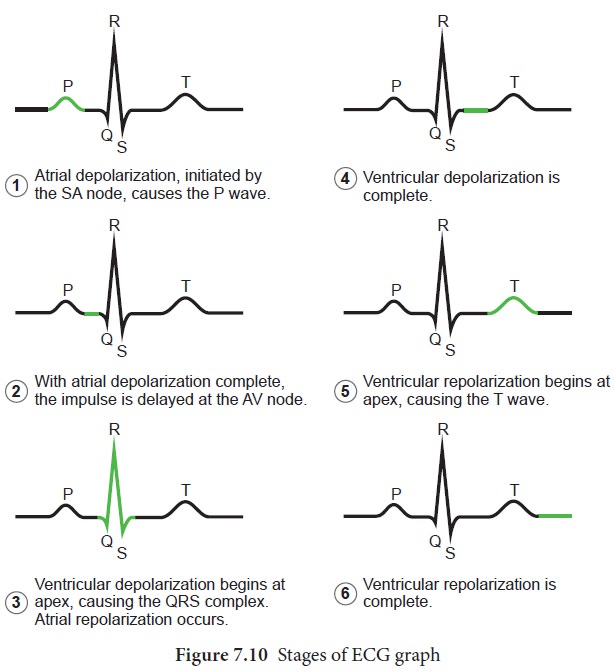
P Wave (atrial depolarisation)
It is a
small upward wave and indicates the depolarisation of the atria. This is the
time taken for the excitation to spread through atria from SA node. Contraction
of both atria lasts for around 0.8-1.0 sec.
PQ Interval (AV node delay)
It is the
onset of P wave to the onset of QRS complex. This is from the start of
depolarisation of the atria to the beginning of ventricular depolarisation. It
is the time taken for the impulse to travel from the atria to the ventricles
(0.12-0.21sec). It is the measure of AV conduction time.
QRS Complex (ventricular depolarisation)
No
separate wave for atrial depolarisation in the ECG is visible. Atrial
depolarisation occurs simultaneously with the ventricular depolarisation. The
normal QRS complex lasts for 0.06-0.09 sec. QRS complex is shorter than the P
wave, because depolarisation spreads through the Purkinjie fibres. Prolonged
QRS wave indicates delayed conduction through the ventricle, often caused due to
ventricular hypertrophy or due to a block in the branches of the bundle of His.
ST Segment
It lies
between the QRS complex and T wave. It is the time during which all regions of
the ventricles are completely depolarised and reflects the long plateau phase
before repolarisation. In the heart muscle, the prolonged
depolarisation is due to retardation of K+ efflux and is responsible for the
plateau. The ST segment lasts for 0.09 sec.
T wave (ventricular depolarisation)
It
represents ventricular depolarisation. The duration of the T wave is longer
than QRS complex because repolarisation takes place simultaneously throughout
the ventricular depolarisation.
Related Topics