Chapter: Medical Surgical Nursing: End-of-Life Care
Goal Setting in Palliative Care at the End of Life
GOAL SETTING IN PALLIATIVE CARE AT THE END OF LIFE
As
the treatment goals begin to shift in the direction of comfort care over
aggressive disease-focused treatment, symptom relief and patient/family-defined
quality of life assume greater promi-nence in treatment decision making.
Patient, family, and clini-cians may all be accustomed to an almost automatic
tendency to pursue exhaustive diagnostic testing to locate and treat the source
of the patient’s illness or symptoms. Each decision to withdraw treatment or
discontinue diagnostic testing will be an extremely emotional one for the
patient and family. They may fear that the support from health care providers
on which they have come to rely will be withdrawn along with the treatment.
Throughout
the course of the illness, and especially as the pa-tient’s functional status
and symptoms indicate approaching death, clinicians need to assist the patient
and family to weigh the benefits of continued diagnostic testing and
disease-focused med-ical treatment against the burdens of those activities.
Patients and their families may be extremely reluctant to forego monitoring
that has become routine throughout the illness (such as blood testing, x-rays)
but that may contribute little to a primary focus on comfort. Likewise, health
care providers from other disciplines may have difficulty discontinuing such
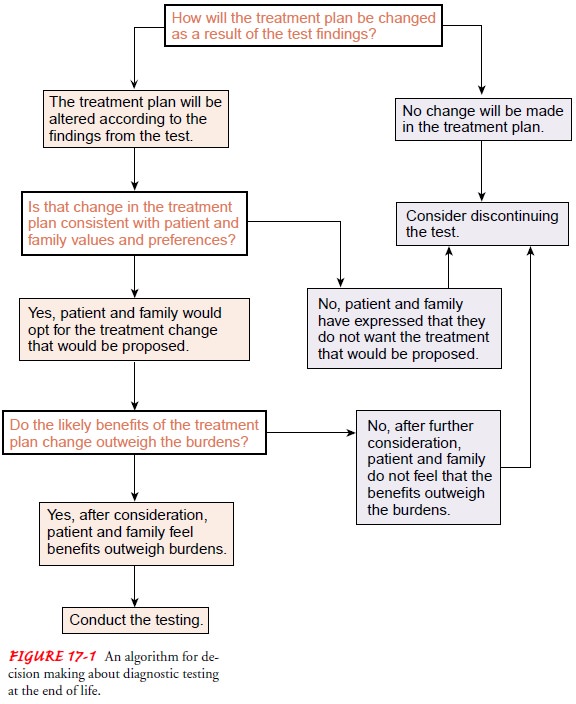
diagnostic testing or med-ical treatment. The nurse should collaborate with
other members of the interdisciplinary team to share assessment findings and
de-velop a coordinated plan of care (Fig. 17-1). In addition, the nurse may
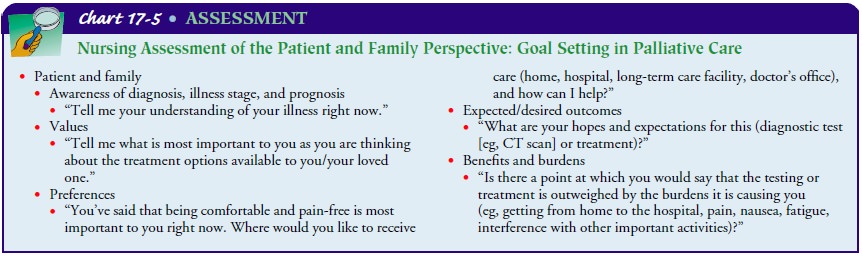
assist the patient and family to clarify their goals, ex-pected outcomes, and
values as they consider treatment options
(Chart 17-5). The nurse needs to work with interdisciplinary colleagues
to ensure that the patient and family are referred for continuing psychosocial
support, symptom management, and assistance with other care-related challenges
(eg, arranging for home care or hospice support, referrals for financial
assistance).
Related Topics