Chapter: Obstetrics and Gynecology: Sexually Transmitted Diseases
General Diagnostic Principles of Sexually Transmitted Diseases(STDs)
GENERAL DIAGNOSTIC PRINCIPLES
Many sexually transmitted
infections are asymptomatic in women or are asymptomatic during the initial
stages of the infection. The signs and
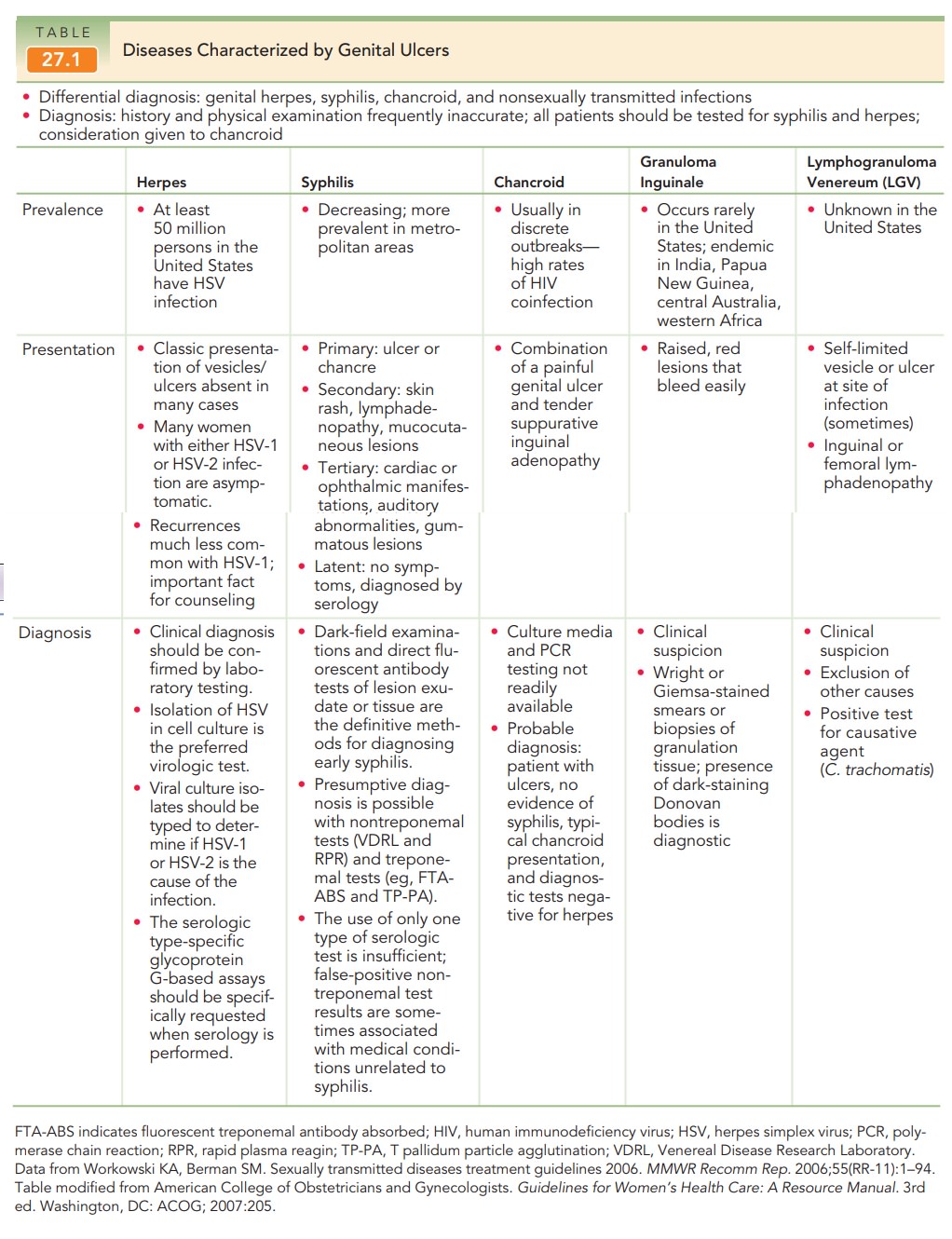
symptoms of many STDs may be char-acterized by genital ulcers or infection of
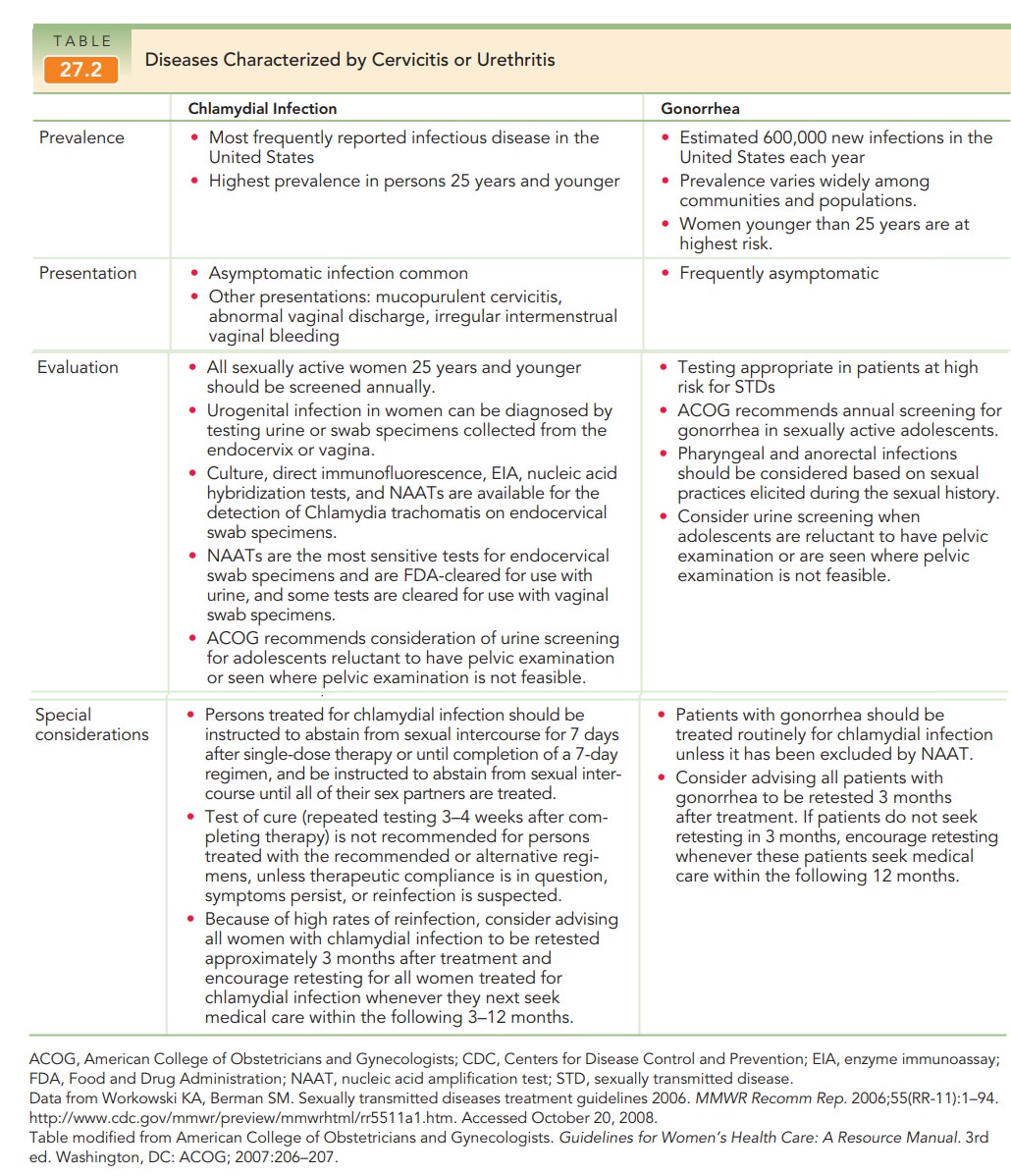
the cervix (cervicitis), ure-thra (urethritis), or both (Table 27.2).
Because 20% to 50% ofpatients with one STD have a coexisting infection, when
one infection is confirmed, other infections must be suspected.
Because of the variations in
signs and symptoms and the asymptomatic presentation of STDs, a thorough sexual
history and physical examination are essential in detecting the presence of an
STD. The findings obtained through a systematic physical assessment, combined
with the patient’s history, usually help make the proper diagnosis. The
inguinal region should be evaluated for rashes, lesions, and adenopathy. The
vulva, perineum, and perianal areas should be inspected for lesions or
ulcerations, and palpated for thickening or swelling. The Bartholin glands,
Skene ducts, and urethra should be evaluated, as these are frequent sites of
gonorrheal infection. In patients with urinary symp-toms, the urethra should be
gently milked to express any discharge. The vagina and cervix should be
inspected for lesions and abnormal discharge. If a patient engages in anal
intercourse, the rectum should be considered a potential site for infection.
For completeness, the oral cavity as well as the cervical and other lymph nodes
should be evaluated, if appropriate, based upon the patient’s modes of sexual
expression.
Related Topics