Method, Procedure, Principle, Importance - Differential Staining | 11th Microbiology : Chapter 3 : Stains and Staining Methods
Chapter: 11th Microbiology : Chapter 3 : Stains and Staining Methods
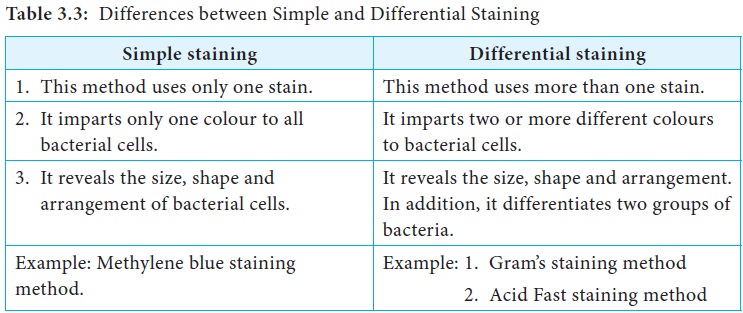
Differential Staining
Differential Staining
In this method more than one stain is
employed. In some method the stains are applied separately, while in other
method they are mixed and applied in one application. These procedures show
differences between the cells or parts of a cell and can be used for of
identification. The two most important differential stains used by bacteriologists
are Gram stain and Acid Fast stain. The differences between simple and
differential staining are shown in Table 3.3.
Gram’s Staining Method
The Gram’s stain technique was
developed by Danish Bacteriologist Hans Christian Gram in 1884. It is one of
the most useful staining methods because it classifies bacteria into two large
groups namely Gram positive and Gram negative. In this method, the fixed
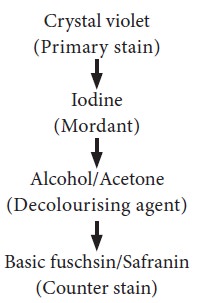
bacterial smear is subjected to staining reagents in the order of sequence
listed below:
The organisms that retain the colour
of the primary stain are called Gram positive and those that do not retain the
primary stain when decolorised and take on the colour of the counter stain are
called Gram negative.
Mordants: Mordants are not dyes. They are important to increase the biological specimen’s affinity for
a dye. Some stains never stain the cells or its components unless treated with
a mordant. The mordant becomes attached to a cell or its components and then
combines with the stain to form an insoluble colour complex.
Procedure of Gram’s Staining
Gram’s Staining comprises of four
steps:
Step 1: A heat fixed smear is covered with a basic violet dye, Example: Crystal violet.
This stain imparts its colour to all cells. It is referred to as a primary
stain, since it is applied first.
Step 2: After a short time, the slide is washed off and the smear is covered with iodine, a mordant. At this stage both Gram positive and Gram negative bacteria appear dark violet.
Step 3: Next, the slide is decolurized with alcohol or an acetone alcohol solution. This solution is a
decolurizing agent, which removes the primary stain from the cells of some
species but not from others.
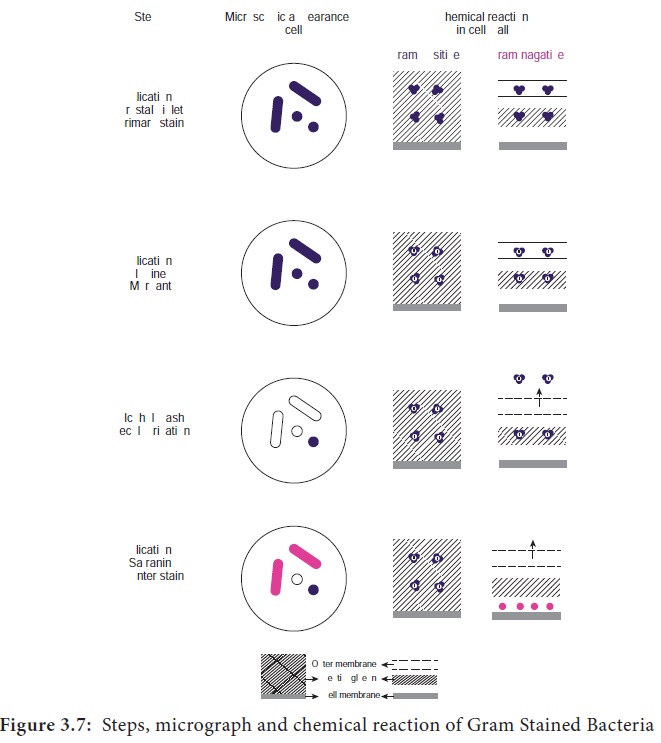
Step 4: The slide is immediately washed after decolurization and the slide is then counter stained with basic
fuchsin or safranin, a basic red dye. The smear is washed again, blot dried and
examined under microscope (Figure 3.7).
Principle of Gram’s Staining
The exact mechanism of action of this
staining technique is not clearly understood. However, the most acceptable
explanations are associated with the structure and composition of the cell
wall.
The cell wall of Gram positive
bacteria have a thicker peptidoglycan (consists of disaccharides and amino
acids) than Gram negative bacteria. Figure 3.8 depicts the cell wall of Gram
positive
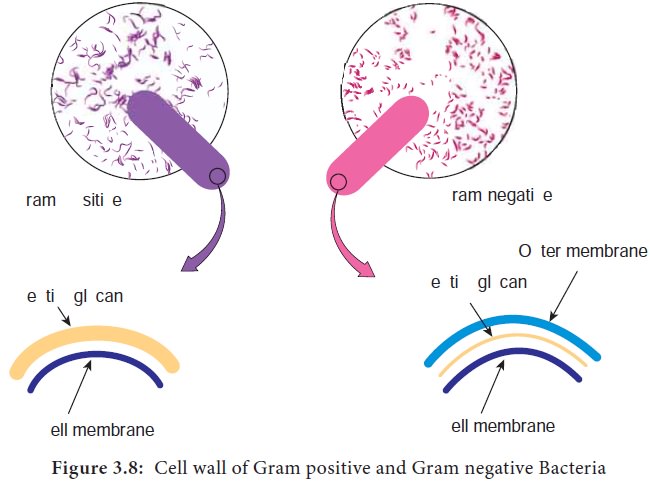
In
addition, Gram negative bacteria contain a layer of lipo polysaccharide
(consists of lipids and polysaccharide) as part of their cell wall. When
Crystal violet and subsequently Iodine is applied to both Gram positive and
Gram negative cells, the two combine to form CV-I complex.
The cell wall of Gram positive
bacteria with lower lipid content get dehydrated during alcohol treatment. The
pore size decreases and the permeability is reduced. Thus, the CV-I complex
cannot be extracted and the cells remain violet.
The alcohol treatment of Gram negative bacteria extracts the lipid which results in increased porosity or permeability of the cell wall. Thus, the crystal violet iodine [CV-I] complex is extracted and the bacteria are decolorized. These cells subsequently take on the colour of the counter stain basic fuchsin or safranin and appears red to pink.
Importance of Gram Staining
This century old staining method
still remains as the universal basis for bacterial classification and
identification. Even with today’s elaborate and expensive
Examination of Gram stained organisms
usually provides the basis for classifying, identifying and characterizing
bacteria. Gram staining of clinical specimens, however provides only a
preliminary indication of the identity of the etiological agent (the organism
causing the disease). Gram nature of common pathogenic bacteria is given in
Table 3.4.
Gram stains of clinical specimens or
of growth on culture plates are especially important in determining the most
effective antibiotic for the ill patients who required immediate therapy.

Related Topics