Chapter: 11th 12th std standard Class Nursing Health Care Hospital Hygiene Higher secondary school College Notes
Dietary Guidelines In Dialysis And Kidney Transplant
DIETARY GUIDELINES IN
DIALYSIS AND KIDNEY TRANSPLANT
Dialysis is a procedure that replaces some of the kidneys normal
functions. It is performed when a person has kidney failure. Dialysis helps to
remove waste products including salt, excess fluids and maintain a safe level
of blood chemicals such as potassium, sodium and chloride in the body and also
controls blood pressure.
Haemodialysis
In haemodialysis the patients blood circulates outside the body through
coils or sheets of semipermeable membranes that are constantly bathed by a
hypotonic dialyzing fluid so that nitrogenous wastes are removed into the
dialysate. The membranes do not permit bacteria to enter the blood nor can
proteins escape from the blood. However some aminoacids are lost into the
dialysate. As haemodialysis is performed 3 times a week for 3 - 4 hrs, it may
be necessary to regulate the protein intake based on the level of nitrogen
waste products. If diet is not controlled dialysis will need to be more
frequent.
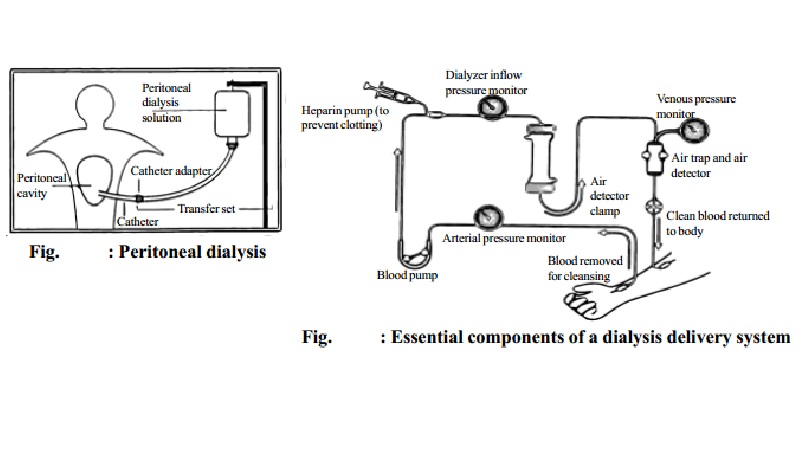
Peritoneal Dialysis
This
consists of introducing 1 to 2 litres of dialysis fluid into the peritoneal
cavity and 30 to 90 minutes later withdrawing the fluid. The process is
repeated until the blood urea level drops to tolerable levels. Some blood
proteins and amino acids are lost and compensation must be made. Fig.
represents peritoneal dialysis.
In
continuous ambulatory peritoneal dialysis (CAPD), the dialysate is introduced
into the abdominal cavity 3 - 5 times each day through a permanent indwelling
catheter. The dialysate remains in the abdominal cavity for 4 - 8 hrs after
which it is drained and fresh dialysate instilled. Protein losses occur but can
be replaced by dietary protein.
system
Source : Srilakshmi B., (2000). Dietetics. 4th ed. New Age International Publishers.
Dietary Management
The diet of a patient on kidney dialysis is important to maintain
biochemical control. The objectives are to
1.
Maintain protein and kilocalorie balance.
2.
Prevent dehydration or fluid overload.
3.
Maintain normal serum potassium and sodium blood
levels and
4.
Maintain acceptable phosphate and calcium
levels.
Protein
For adults 1 g/kg body weight provides nutritional needs, maintains
positive nitrogen balance and replaces amino acids lost during dialysis
treatment. 75 percent of daily protein allowance should be protein of high
biological value such as eggs, meat, fish and poultry. Milk is restricted as it
has a high content of sodium, phosphate and potassium.
Energy
Carbohydrates are given to supply energy and prevent protein breakdown.
The usual need is 40 kcal / kg lean body weight. Simple carbohydrate foods
should be given.
Water balance
Fluid is limited to 400 to 500 ml / day plus an amount equal to urinary
output.
Sodium
To control body fluid retention and hypertension, sodium is limited to
1000 to 2000 mg / day.
Potassium
Potassium accumulation can cause cardiac arrest and hence potassium
restriction is necessary. A dietary allowance of 1500 to 2000 mg /d ay is
given.
Vitamins
During dialysis water soluble vitamins from the blood are lost. A daily
supplement of all water soluble vitamins is given. Fat soluble vitamins
especially vitamin A and D may build up.
Diet for a person with kidney transplant
Initially after the kidney transplant, it is necessary to maintain
dietary restrictions. Diet modification can help to keep the blood pressure,
blood sugar and cholesterol levels within the normal limits. Optimal protein
and energy intake with restriction of salt, simple sugars, total fat,
cholesterol and saturated fat is necessary. The healthy diet pyramid advocates
eating more cereals, bread, legumes, vegetables and fruit, eating moderate
amounts of milk, cheese, lean meat, poultry, fish and eggs and eating least
quantities of sugar, oil and butter.
Related Topics