Chapter: Medical Physiology: Muscle Blood Flow and Cardiac Output During Exercise; the Coronary Circulation and schemic Heart Disease
Control of Blood Flow Through the Skeletal Muscles
Control of Blood Flow Through the Skeletal Muscles
Local Regulation—Decreased Oxygen in Muscle Greatly Enhances Flow. The tremendous increase in muscleblood flow that occurs during skeletal muscle activity is caused primarily by chemical effects acting directly on the muscle arterioles to cause dilation. One of the most important chemical effects is reduction of oxygen in the muscle tissues. That is, during muscle activity, the muscle uses oxygen rapidly, thereby decreasing the oxygen concentration in the tissue fluids. This in turn causes local arteriolar vasodilation both because the arteriolar walls cannot maintain contraction in the absence of oxygen and because oxygen deficiency causes release of vasodilator substances. The most important vasodilator substance is probably adeno-sine, but experiments have shown that even large amounts of adenosine infused directly into a muscle artery cannot sustain vasodilation in skeletal muscle for more than about 2 hours.
Fortunately, even after the muscle blood vessels have become insensitive to the vasodilator effects of adenosine, still other vasodilator factors continue to maintain increased capillary blood flow as long as the exercise continues. These factors include (1) potassium ions, (2) adenosine triphosphate (ATP), (3) lactic acid, and (4) carbon dioxide. We still do not know quanti-tatively how great a role each of these plays in in-creasing muscle blood flow during muscle activity;
Nervous Control of Muscle Blood Flow. In addition to localtissue vasodilator mechanisms, skeletal muscles are provided with sympathetic vasoconstrictor nerves and (in some species of animals) sympathetic vasodilator nerves as well.
Sympathetic Vasoconstrictor Nerves. The sympa-thetic vasoconstrictor nerve fibers secrete norepineph-rine at their nerve endings. When maximally activated,this can decrease blood flow through resting muscles to as little as one half to one third normal. This vaso-constriction is of physiologic importance in circulatory shock and during other periods of stress when it is necessary to maintain a normal or even high arterial pressure.
In addition to the norepinephrine secreted at the sympathetic vasoconstrictor nerve endings, the medul-lae of the two adrenal glands also secrete large amounts of norepinephrine plus even more epineph-rine into the circulating blood during strenuous exer-cise. The circulating norepinephrine acts on the muscle vessels to cause a vasoconstrictor effect similar to that caused by direct sympathetic nerve stimulation. The epinephrine, however, often has a slight vasodilator effect because epinephrine excites more of the beta adrenergic receptors of the vessels, which are vasodila-tor receptors, in contrast to the alpha vasoconstrictor receptors excited especially by norepinephrine.
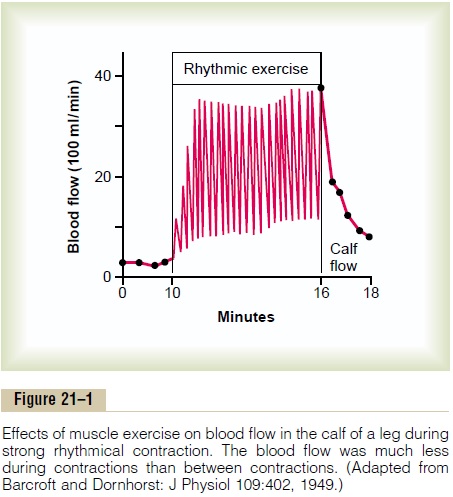
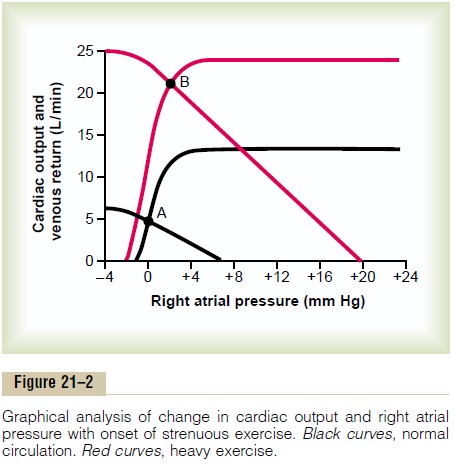
Related Topics