Chapter: Medical Surgical Nursing: Homeostasis, Stress, and Adaptation
Cellular Injury
CELLULAR
INJURY
Injury is defined as a
disorder in steady-state regulation. Any stressor that alters the ability of
the cell or system to maintain op-timal balance of its adjustment processes
will lead to injury. Structural and functional damage then occurs, which may be
re-versible (permitting recovery) or irreversible (leading to disability or
death). Homeostatic adjustments are concerned with the small changes within the
body’s systems. With adaptive changes, com-pensation occurs and a steady state
is achieved, although it may be at new levels. With injury, steady-state
regulation is lost, and changes in functioning ensue.
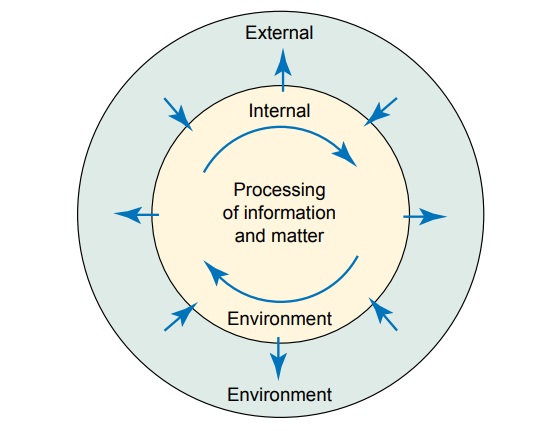
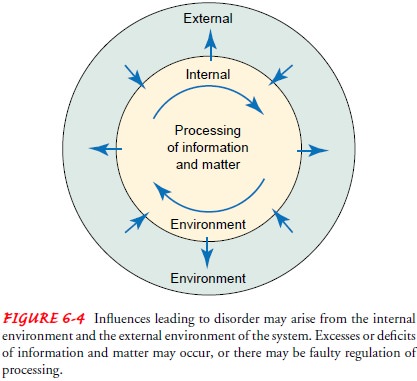
Causes of disorder and
injury in the system (cell, tissue, organ, body) may arise from the external or
internal environment (Fig. 6-4) and include hypoxia, nutritional imbalance,
physical agents, chemical agents, infectious
agents, immune mecha-nisms, genetic defects, and psychogenic factors. The
most com-mon causes are hypoxia (oxygen deficiency), chemical injury, and
infectious agents. In addition, the presence of one injury makes the system
more susceptible to another injury. For example, in-adequate oxygenation and
nutritional deficiencies make the sys-tem vulnerable to infection. These agents
act at the cellular level by damaging or destroying
· The integrity of the
cell membrane, necessary for ionic bal-ance
· The ability of the cell
to transform energy (aerobic respira-tion, production of adenosine
triphosphate)
· The ability of the cell
to synthesize enzymes and other nec-essary proteins
· The ability of the cell
to grow and reproduce (genetic in-tegrity)
Hypoxia
Inadequate cellular oxygenation
(hypoxia) interferes with the cell’s ability to transform energy. Hypoxia may
be caused by:
· decrease in blood supply
to an area
· decrease in the
oxygen-carrying capacity of the blood (de-creased hemoglobin)
· ventilation/perfusion or
respiratory problem that reduces the amount of oxygen available in the blood
· problem in the cell’s
enzyme system that makes it unable to use the oxygen delivered to it
The usual cause is
ischemia, or deficient blood supply. Ischemia is commonly seen in myocardial
cell injury in which arterial blood flow is decreased because of
atherosclerotic narrowing of blood vessels. Ischemia also results from
intravascular clots (thrombi or emboli) that may form and interfere with blood
sup-ply. Thrombi and emboli are common causes of cerebrovascular accidents
(strokes). The length of time different tissues can sur-vive without oxygen
varies. For example, brain cells may succumb in 3 to 6 minutes, depending on
the situation. If the condition leading to hypoxia is slow and progressive,
collateral circulation may develop, whereby blood is supplied by other blood
vessels in the area. However, this mechanism is not highly reliable.
Nutritional Imbalance
Nutritional imbalance
refers to a relative or absolute deficiency or excess of one or more essential
nutrients. This may be mani-fested as undernutrition (inadequate consumption of
food or calories) or overnutrition (caloric excess). Caloric excess to the
point of obesity overloads cells in the body with lipids. By re-quiring more
energy to maintain the extra tissue, obesity places a strain on the body and
has been associated with the development of disease, especially pulmonary and
cardiovascular disease.
Specific deficiencies
arise when an essential nutrient is defi-cient or when there is an imbalance of
nutrients. Protein defi-ciencies and avitaminosis (deficiency of vitamins) are
typical examples. An energy deficit leading to cell injury can occur if there
is insufficient glucose, or insufficient oxygen to transform the glucose into energy.
A lack of insulin, or the inability to use insulin, may also prevent glucose
from entering the cell from the blood. This occurs in diabetes mellitus, a
metabolic disorder that can lead to nutritional deficiency.
Physical Agents
Physical agents, including
temperature extremes, radiation, elec-trical shock, and mechanical trauma, can
cause injury to the cells or to the entire body. The duration of exposure and
the intensity of the stressor determine the severity of damage.
EXTREMES OF HIGH TEMPERATURE
When a person’s
temperature is elevated, hypermetabolism oc-curs and the respiratory rate,
heart rate, and basal metabolic rate all increase. With fever induced by
infections, the hypothalamic thermostat may be reset at a higher temperature,
then return to normal when the fever abates. The increase in body temperature
is achieved through physiologic mechanisms. Body temperatures greater than 41°C (106°F)
suggest hyperthermia, because the physiologic function of the thermoregulatory
center breaks down and the temperature soars. This physiologic condition occurs
in people with heat stroke. Eventually, the high temperature causes coagulation
of cell proteins, and the cells die. The body must be cooled rapidly to prevent
brain damage.
The local response to
thermal or burn injury is similar. There is an increase in metabolic activity,
and, as heat increases, protein is coagulated, enzyme systems are destroyed,
and, in the extreme, charring or carbonization occurs. Burns of the epithelium
are classified as partial-thickness burns if epithelializing elements re-main
to support healing. Full-thickness burns lack such elements and must be grafted
for healing. The amount of body surface in-volved determines the prognosis for
the patient. If the injury is severe, the entire body system becomes involved,
and hyper-metabolism develops as a pathophysiologic response.
EXTREMES OF LOW TEMPERATURE
Extremes of low
temperature, or cold, cause vasoconstriction. Blood flow becomes sluggish and
clots form, leading to ischemic damage in the involved tissues. With still
lower temperatures, ice crystals may form, and the cells may burst.
RADIATION AND ELECTRICAL SHOCK
Radiation is used for
diagnosis and treatment of diseases. Ioniz-ing forms of radiation may cause
injury by their destructive ac-tion. Radiation decreases the protective
inflammatory response of the cell, creating a favorable environment for
opportunistic in-fections. Electrical shock produces burns as a result of the
heat generated when electrical current travels through the body. It may also
abnormally stimulate nerves, leading, for example, to fibrillation of the
heart.
MECHANICAL TRAUMA
Mechanical trauma can
result in wounds that disrupt the cells and tissues of the body. The severity
of the wound, the amount of blood loss, and the extent of nerve damage are
significant factors in the outcome.
Chemical Agents
Chemical injuries are
caused by poisons, such as lye, which has a corrosive action on epithelial
tissue, or by heavy metals, such as mercury, arsenic, and lead, each with its
own specific destructive action. Many other chemicals are toxic in specific
amounts, in certain people, and in distinctive tissues. Excessive secretion of
hydrochloric acid can damage the stomach lining; large amounts of glucose can
cause osmotic shifts, affecting the fluid and elec-trolyte balance; and too
much insulin can cause subnormal levels of glucose in the blood (hypoglycemia)
and can lead to coma.
Drugs, including
prescribed medications, can also cause chem-ical poisoning. Some individuals
are less tolerant of medications than others and manifest toxic reactions at
the usual or custom-ary dosages. Aging tends to decrease tolerance to
medications. Polypharmacy (taking many medications at one time) also occurs
frequently in the aging population and is a problem because of the
unpredictable effects of the resulting medication interactions.
Alcohol (ethanol) is
also a chemical irritant. In the body, al-cohol is broken down into
acetaldehyde, which has a direct toxic effect on liver cells that leads to a
variety of liver abnormalities, including cirrhosis in susceptible individuals.
Disordered liver cell function leads to complications in other organs of the
body.
Infectious Agents
Biologic agents known to
cause disease in humans are viruses, bacteria, rickettsiae, mycoplasmas, fungi,
protozoa, and nema-todes. The severity of the infectious disease depends on the
num-ber of microorganisms entering the body, their virulence, and the host’s
defenses (eg, health, age, immune defenses).
Some bacteria, such as
those that cause tetanus and diphtheria, produce exotoxins that circulate and
create cell damage. Others, such as the gram-negative bacteria, produce
endotoxins when they are killed. The tubercle bacillus induces an immune
reaction.
Viruses, the smallest
living organisms, survive as parasites of the living cells they invade. Viruses
infect specific cells. Through a complex mechanism, they replicate within the
cells, then invade other cells and continue to replicate. An immune response is
mounted by the body to eliminate the viruses, and the cells har-boring the
viruses can be injured in the process. Typically, an in-flammatory response and
immune reaction are the physiologic responses of the body to the presence of
infection.
Disordered Immune Responses
The immune system is an
exceedingly complex system; its pur-pose is to defend the body from invasion by
any foreign object or foreign cell type, such as cancerous cells. This is a
steady-state mechanism, but like other adjustment processes it can become
disordered, and cell injury will occur. The immune response de-tects foreign
bodies by distinguishing non-self substances from self substances and
destroying the non-self entities. The entrance of an antigen (foreign
substance) into the body evokes the production of antibodies that attack and
destroy the antigen (antigen–antibody reaction).
The immune system can be
hypoactive or hyperactive. When it is hypoactive, immunodeficiency diseases
occur; when it is hy-peractive, hypersensitivity disorders arise. A disorder of
the im-mune system itself can result in damage to the body’s own tissues. Such
disorders are labeled autoimmune diseases (see Unit 11).
Genetic Disorders
Genetic defects as
causes of disease and their effects on genetic structure are of intense
research interest. Many of these defects produce mutations that have no
recognizable effect, such as lack of a single enzyme; others contribute to more
obvious congen-ital abnormalities, such as Down syndrome. As a result of the
Human Genome Project, patients can be genetically assessed for conditions such
as sickle cell disease, cystic fibrosis, hemophilia A and B, breast cancer,
obesity, cardiovascular disease, phenylke-tonuria, and Alzheimer’s disease. The
availability of genetic information and technology enables health care
providers to per-form screening, testing, and counseling for patients with
genetic concerns. Knowledge obtained from the Human Genome Proj-ect has also
created opportunities for assessing a person’s genetic profile and preventing
or treating disease. Diagnostic genetics and gene therapy have the potential to
identify and modify a gene before it begins to express traits that would lead
to disease or disability.
Related Topics