Chapter: Medical Physiology: Respiratory Insufficiency-Pathophysiology, Diagnosis, Oxygen Therapy
Atelectasis
Atelectasis
Atelectasis means collapse of the alveoli. It can occur in localized areas of a lung or in an entire lung. Its most common causes are (1) total obstruction of the airway or (2) lack of surfactant in the fluids lining the alveoli.
Airway Obstruction. The airway obstruction type ofatelectasis usually results from (1) blockage of many small bronchi with mucus or (2) obstruction of a major bronchus by either a large mucus plug or some solid object such as a tumor. The air entrapped beyond the block is absorbed within minutes to hours by the blood flowing in the pulmonary capillaries. If the lung tissue is pliable enough, this will lead simply to collapse of the alveoli.
However, if the lung is rigid because of fibrotic tissue and cannot collapse, absorption of air from the alveoli creates very negative pressures within the alveoli, which pull fluid out of the pulmonary cap-illaries into the alveoli, thus causing the alveoli to fill completely with edema fluid. This almost always is the effect that occurs when an entire lung becomes atelectatic, a condition called massive collapse of the lung.
The effects on overall pulmonary function caused by massive collapse (atelectasis) of an entire lung areshown in Figure 42–7. Collapse of the lung tissue not only occludes the alveoli but also almost always increases the resistance to blood flow through the pul-monary vessels of the collapsed lung.
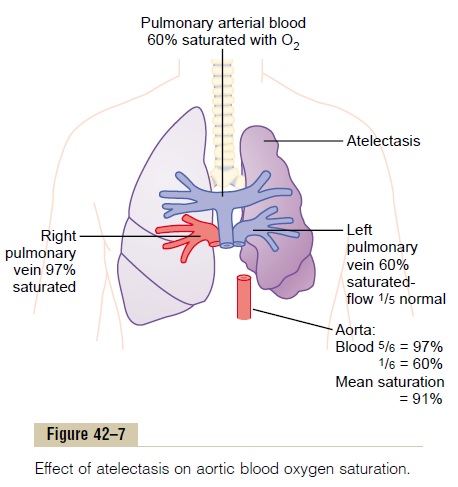
This resistance increase occurs partially because of the lung collapse itself, which compresses and folds the vessels as the volume of the lung decreases. In addition, hypoxia in the collapsed alveoli causes additional vasoconstriction.
Because of the vascular constriction, blood flow through the atelectatic lung becomes slight. Fortu-nately, most of the blood is routed through the venti-lated lung and therefore becomes well aerated. In the situation shown in Figure 42–7, five sixths of the blood passes through the aerated lung and only one sixth through the unaerated lung. As a result, the overall ventilation-perfusion ratio is only moderately com-promised, so that the aortic blood has only mild oxygen desaturation despite total loss of ventilation in an entire lung.
Lack of “Surfactant” as a Cause of Lung Collapse. The secre-tion and function of surfactant in the alveoli were discussed. It was pointed out that the surfactant is secreted by special alveolar epithelial cells into the fluids that coat the inside surface of the alveoli. The surfactant in turn decreases the surface tension in the alveoli 2- to 10-fold, which normally plays a major role in preventing alveolar collapse. However, in a number of conditions, such as in hyalinemembrane disease (also called respiratory distress syn-drome), which often occurs in newborn prematurebabies, the quantity of surfactant secreted by the alveoli is so greatly depressed that the surface tension of the alveolar fluid becomes several times normal. This causes a serious tendency for the lungs of these babies to collapse or to become filled with fluid. Many of these infants die of suffocation when large portions of the lungs become atelectatic.
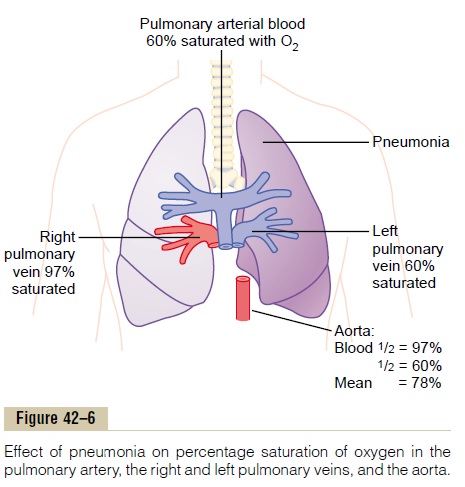
Related Topics