Chapter: Clinical Anesthesiology: Anesthetic Equipment & Monitors : The Anesthesia Machine
Anesthesia Ventilators Pressure & Volume Monitoring
Pressure & Volume Monitoring
Peak inspiratory pressure is the highest
circuit pressure generated during an inspiratory cycle, and provides an
indication of dynamic compli-ance. Plateau pressure is the pressure measured
during an inspiratory pause (a time of no gas flow), and mirrors static
compliance. During
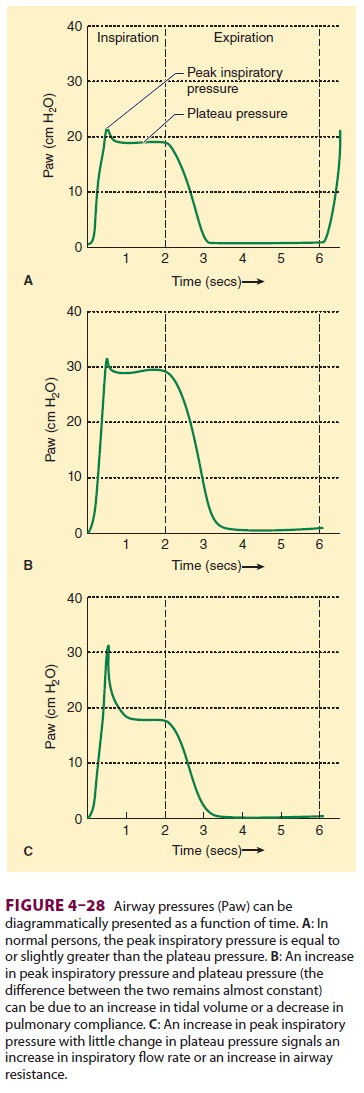
normal ventilation of a patient without
lung dis-ease, peak inspiratory pressure is equal to or only slightly greater
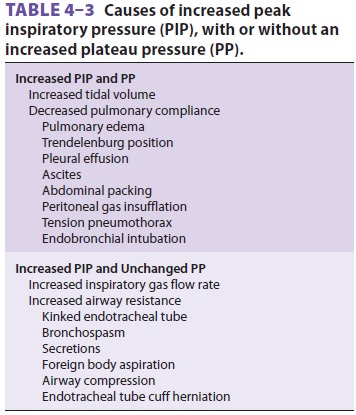
than plateau pressure. An increase in both peak inspiratory pressure and
plateau pressure implies an increase in tidal volume or a decrease in pulmonary
compliance. An increase in peak inspira-tory pressure without any change in
plateau pressure signals an increase in airway resistance or inspira-tory gas
flow rate (Table
4–3). Thus, the shape of the breathing-circuit pressure waveform can
provide important airway information. Many anesthesia machines graphically
display breathing-circuit pres-sure (Figure 4–28). Airway secretions or kinking of
the tracheal tube can be easily ruled out with the use of a suction catheter.
Flexible fiberoptic bronchos-copy will usually provide a definitive diagnosis.
Ventilator Alarms
Alarms are an integral part of all modern anesthesia ventilators. Whenever a ventilator is used “disconnect alarms” must be passively activated. Anesthesia workstations should have at least three disconnect alarms: low peak inspiratory pres-sure, low exhaled tidal volume, and low exhaled car-bon dioxide. The first is always built into the ventilator whereas the latter two may be in separate modules. A small leak or partial breathing-circuit disconnection may be detected by subtle decreases in peak inspiratory pressure, exhaled volume, or end-tidal carbon dioxide before alarm thresholds are reached. Other built-in ventilator alarms include high peak inspiratory pressure, high PEEP, sustained high airway pressure, negative pressure, and low oxygen-supply pressure. Most modern anesthesia ventilators also have integrated spirometers and oxygen analyzers that provide additional alarms.
Related Topics