Chapter: Basic & Clinical Pharmacology : The Alcohols
Alcohol-Drug Interactions
Alcohol-Drug Interactions
Interactions
between ethanol and other drugs can have important clinical effects resulting
from alterations in the pharmacokinetics or pharmacodynamics of the second
drug.
The
most common pharmacokinetic alcohol-drug interactions stem from alcohol-induced
increases of drug-metabolizing enzymes, as described. Thus, prolonged intake of
alcohol without damage to the liver can enhance the metabolic biotransformation
of other drugs. Ethanol-mediated induction of hepatic cytochrome P450 enzymes
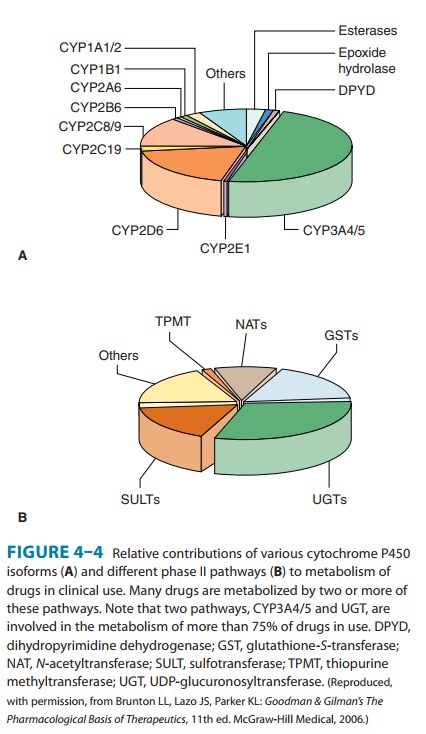
is particularly important with regard to acetaminophen. Chronic consumption of
three or more drinks per day increases the risk of hepatotoxicity due to toxic
or even high therapeutic levels of acetaminophen as a result of increased
P450-mediated conversion of acetaminophen to reactive hepatotoxic metabolites
(see Figure 4–4). In 1998, the Food and Drug Administration (FDA) announced
that all over-the-counter products containing acetaminophen must carry a
warning about the relation between chronic ethanol consumption and
acetamin-ophen-induced hepatotoxicity.
In
contrast, acute alcohol use can
inhibit metabolism of other drugs because of decreased enzyme activity or
decreased liver blood flow. Phenothiazines, tricyclic antidepressants, and
sedative-hypnotic drugs are the most important drugs that interact with alcohol
by this pharmacokinetic mechanism.
Pharmacodynamic
interactions are also of great clinical signifi-cance. The additive CNS
depression that occurs when alcohol is combined with other CNS depressants,
particularly sedative-hypnotics, is most important. Alcohol also potentiates
the pharmacologic effects of many nonsedative drugs, including vasodilators and
oral hypoglycemic agents.
Related Topics