Chapter: Medical Physiology: Heart Muscle; The Heart as a Pump and Function of the Heart Valves
Work Output of the Heart: Graphical Analysis of Ventricular Pumping
Work Output of the Heart
The stroke work output of the heart is the amount of energy that the heart converts to work during each heartbeat while pumping blood into the arteries.Minutework output is the total amount of energy converted towork in 1 minute; this is equal to the stroke work output times the heart rate per minute.
Work output of the heart is in two forms. First, by far the major proportion is used to move the blood from the low-pressure veins to the high-pressure arteries. This is called volume-pressure work or external work.
Second, a minor proportion of the energy is used to accelerate the blood to its velocity of ejection through the aortic and pulmonary valves. This is thekineticenergy of blood flow component of the work output.
Right ventricular external work output is normally about one sixth the work output of the left ventricle because of the sixfold difference in systolic pressures that the two ventricles pump. The additional work output of each ventricle required to create kinetic energy of blood flow is proportional to the mass of blood ejected times the square of velocity of ejection.
Ordinarily, the work output of the left ventricle required to create kinetic energy of blood flow is only about 1 per cent of the total work output of the ventri-cle and therefore is ignored in the calculation of the total stroke work output. But in certain abnormal con-ditions, such as aortic stenosis, in which blood flows with great velocity through the stenosed valve, more than 50 per cent of the total work output may be required to create kinetic energy of blood flow.
Graphical Analysis of Ventricular Pumping
Figure 9–7 shows a diagram that is especially useful in explaining the pumping mechanics of the left ventricle. The most important components of the diagram are the two curves labeled “diastolic pressure” and “systolic pressure.” These curves are volume-pressure curves.
The diastolic pressure curve is determined by filling the heart with progressively greater volumes of blood and then measuring the diastolic pressure immediately before ventricular contraction occurs, which is the end-diastolic pressure of the ventricle.
The systolic pressure curve is determined by record-ing the systolic pressure achieved during ventricular contraction at each volume of filling.
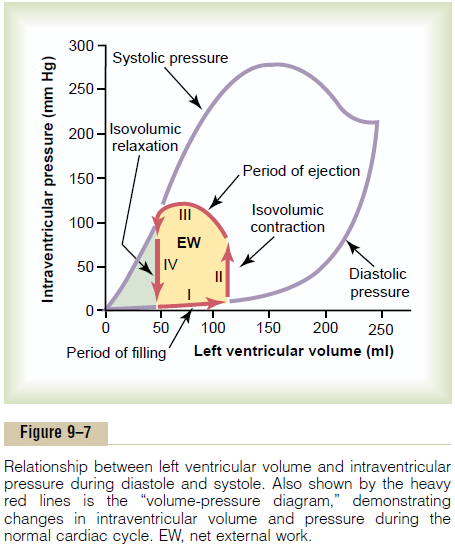
Until the volume of the noncontracting ventricle rises above about 150 milliliters, the “diastolic” pressure does not increase greatly. Therefore, up to this volume, blood can flow easily into the ventricle from the atrium. Above 150 milliliters, the ventricular diastolic pressure increases rapidly, partly because of fibrous tissue in the heart that will stretch no more and partly because the pericardium that surrounds the heart becomes filled nearly to its limit.
During ventricular contraction, the “systolic” pres-sure increases even at low ventricular volumes and reaches a maximum at a ventricular volume of 150 to 170 milliliters. Then, as the volume increases still further, the systolic pressure actually decreases under some conditions, as demonstrated by the falling systolic pressure curve in Figure 9–7, because at these great volumes, the actin and myosin filaments of the cardiac muscle fibers are pulled apart far enough that the strength of each cardiac fiber contraction becomes less than optimal.
Note especially in the figure that the maximum sys-tolic pressure for the normal left ventricle is between 250 and 300 mm Hg, but this varies widely with each person’s heart strength and degree of heart stimulation by cardiac nerves. For the normal right ventricle,the maximum systolic pressure is between 60 and80 mm Hg.
“Volume-Pressure Diagram” During the Cardiac Cycle; Cardiac Work Output. The red lines in Figure 9–7 form a loopcalled the volume-pressure diagram of the cardiac cycle for normal function of the left ventricle. It is divided into four phases.
Phase I: Period of filling. This phase in the volume-pressure diagram begins at a ventricular volume of about 45 milliliters and a diastolic pressure near 0 mm Hg. Forty-five milliliters is the amount of blood that remains in the ventricle after the previous heartbeat and is called the end-systolicvolume. As venous blood flows into the ventriclefrom the left atrium, the ventricular volume normally increases to about 115 milliliters, called the end-diastolic volume, an increase of 70 milliliters. Therefore, the volume-pressure diagram during phase I extends along the line labeled “I,” with the volume increasing to 115 milliliters and the diastolic pressure rising to about 5 mm Hg.
Phase II: Period of isovolumic contraction. During isovolumic contraction, the volume of the ventricle does not change because all valves are closed. However, the pressure inside the ventricle increases to equal the pressure in the aorta, at a pressure value of about 80 mm Hg, as depicted by the arrow end of the line labeled “II.”
Phase III: Period of ejection. During ejection, the systolic pressure rises even higher because of still more contraction of the ventricle. At the same time, the volume of the ventricle decreases because the aortic valve has now opened and blood flows out of the ventricle into the aorta. Therefore, the curve labeled “III” traces the changes in volume and systolic pressure during this period of ejection.
Phase IV: Period of isovolumic relaxation. At the end of the period of ejection, the aortic valve closes, and the ventricular pressure falls back to the diastolic pressure level. The line labeled “IV” traces this decrease in intraventricular pressure without any change in volume. Thus, the ventricle returns to its starting point, with about 45 milliliters of blood left in the ventricle and at an atrial pressure near 0 mm Hg.
Readers well trained in the basic principles of physics should recognize that the area subtended by this func-tional volume-pressure diagram (the tan shaded area, labeled EW) represents the net external work output of the ventricle during its contraction cycle. In experimen-tal studies of cardiac contraction, this diagram is used for calculating cardiac work output.
When the heart pumps large quantities of blood, the area of the work diagram becomes much larger. That is, it extends far to the right because the ventricle fills with more blood during diastole, it rises much higher because the ventricle contracts with greater pressure, and it usually extends farther to the left because the ventricle contracts to a smaller volume—especially if the ventri-cle is stimulated to increased activity by the sympathetic nervous system.
Concepts of Preload and Afterload. In assessing the contrac-tile properties of muscle, it is important to specify the degree of tension on the muscle when it begins to con-tract, which is called the preload, and to specify the load against which the muscle exerts its contractile force, which is called theafterload.
For cardiac contraction, the preload is usually con-sidered to be the end-diastolic pressure when the ven-tricle has become filled.
The afterload of the ventricle is the pressure in the artery leading from the ventricle. In Figure 9–7, this cor-responds to the systolic pressure described by the phase III curve of the volume-pressure diagram. (Sometimes the afterload is loosely considered to be the resistance in the circulation rather than the pressure.)
The importance of the concepts of preload and after-load is that in many abnormal functional states of the heart or circulation, the pressure during filling of the ventricle (the preload), the arterial pressure against which the ventricle must contract (the afterload), or both are severely altered from normal.
Related Topics