Chapter: Essentials of Anatomy and Physiology: The Vascular System
Veins - Anatomy and Physiology
VEINS
Veins carry blood from capillaries back to the heart; the smaller veins are called venules. The same three tissue layers are present in veins as in the walls of arteries, but there are some differences when com-pared to the arterial layers. The inner layer of veins is smooth endothelium, but at intervals this lining is folded to form valves (see Fig. 13–1). Valves prevent backflow of blood and are most numerous in veins of the legs, where blood must often return to the heart against the force of gravity.
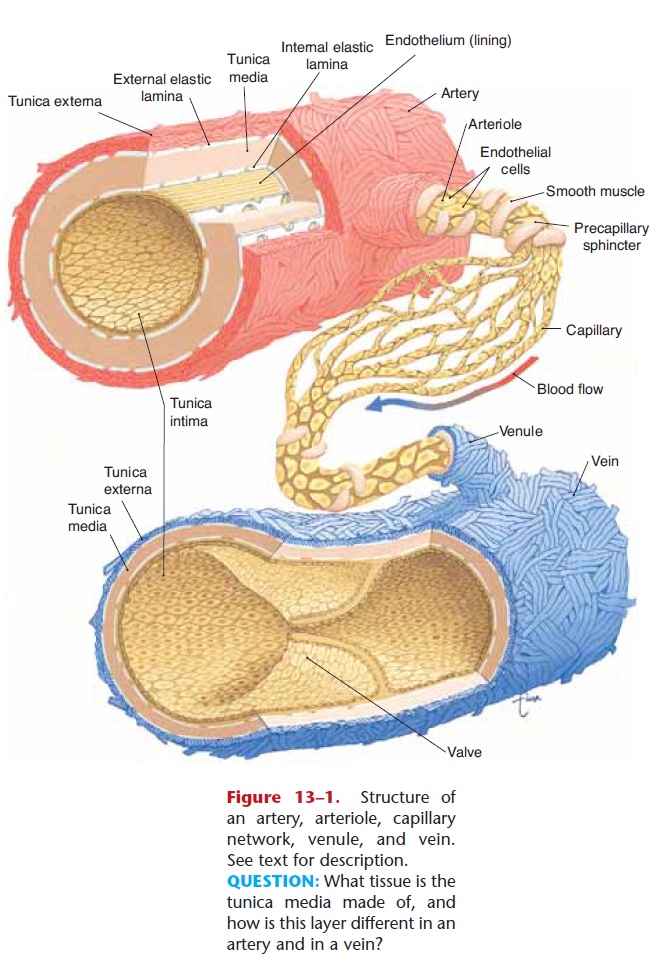
The middle layer of veins is a thin layer of smooth muscle. It is thin because veins do not regulate blood pressure and blood flow into capillaries as arteries do. Veins can constrict extensively, however, and this function becomes very important in certain situations such as severe hemorrhage. The outer layer of veins is also thin; not as much fibrous connective tissue is nec-essary because blood pressure in veins is very low.
ANASTOMOSES
An anastomosis is a connection, or joining, of vessels, that is, artery to artery or vein to vein. The general purpose of these connections is to provide alternate pathways for the flow of blood if one vessel becomes obstructed.
An arterial anastomosis helps ensure that blood will get to the capillaries of an organ to deliver oxygen and nutrients and to remove waste products. There are arterial anastomoses, for example, between some of the coronary arteries that supply blood to the myocardium.
A venous anastomosis helps ensure that blood will be able to return to the heart in order to be pumped again. Venous anastomoses are most numerous among the veins of the legs, where the possibility of obstruc-tion increases as a person gets older.
Related Topics