Chapter: Medicine and surgery: Nervous system
Spinal cord compression - Disorders of the spinal cord
Spinal cord compression
Definition
Spinal cord compression is a medical emergency, as without rapid relief of the compression, permanent neurological deficit results.
Aetiology
Causes are shown in Table 7.11.
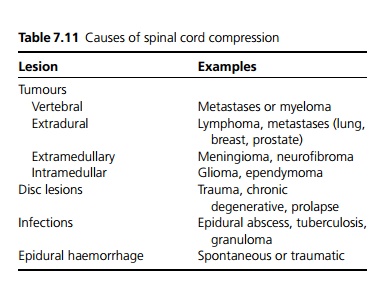
Clinical features
Patients may present with clumsiness, weakness, loss of sensation, loss of bowel or bladder control which may begin as urinary hesitancy and urgency progressing to painless urinary retention. Back pain may precede the presentation with cord compression for many months and there may be radicular pain at the level of compression (radiating around the chest for thoracic lesions and into the limb(s) for cervical and lumbar lesions). On examination there may be a spastic paraparesis or tetraparesis with weakness, increased reflexes and upgoing plantars. There is variable sensory loss below the level of the lesion.
· Conus medullaris: Compression of the sacral segments of the cord causes early disturbance of bladder and bowel control, there is reduced sensation over the perianal region.
· Cauda equina lesion: Compression below L1 affects the spinal nerves and cauda equina resulting in a flaccid, asymmetrical paraparesis. Reflexes are loss and there is loss of sensation over the perianal region (saddle anaesthesia). However, bladder and bowel control are preserved until relatively late.
Investigations
Plain spinal films may show bone disease, urgent MRI spine or myelography (injection of water-soluble contrast into the lumbar subarachnoid space) is required in acute cases. MRI is most useful as it can demonstrate most causes of spinal cord compression.
Management
Identification and treatment aimed at the underlying cause. In as many as 20% of cases, the cord compression is the initial presentation of an underlying malignancy. Radiotherapy is used for metastases, in other causes urgent neurosurgical decompression is required to maximise return of function.
Prognosis
Prognosis is related to the degree of damage and speed of decompression. Bladder control that has been lost for more than 24 hours is usually not regained.
Related Topics