Chapter: Medical Physiology: Pulmonary Ventilation
Pulmonary Volumes and Capacities
Pulmonary Volumes and Capacities
Recording Changes in Pulmonary Volume—Spirometry
A simple method for studying pulmonary ventilation is to record the volume movement of air into and out of the lungs, a process called spirometry. A typical basic spirometer is shown in Figure 37–5. It consists of a drum inverted over a chamber of water, with the drum counterbalanced by a weight. In the drum is a breathing gas, usually air or oxygen; a tube connects the mouth with the gas chamber. When one breathes into and out of the chamber, the drum rises and falls, and an appropriate recording is made on a moving sheet of paper.
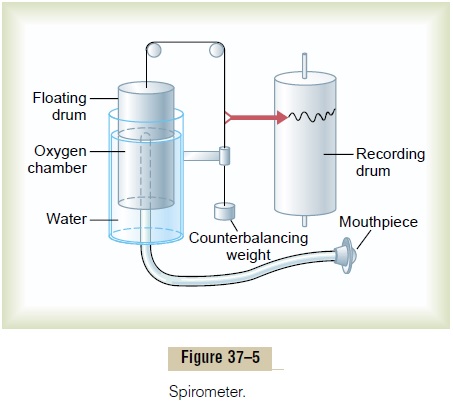
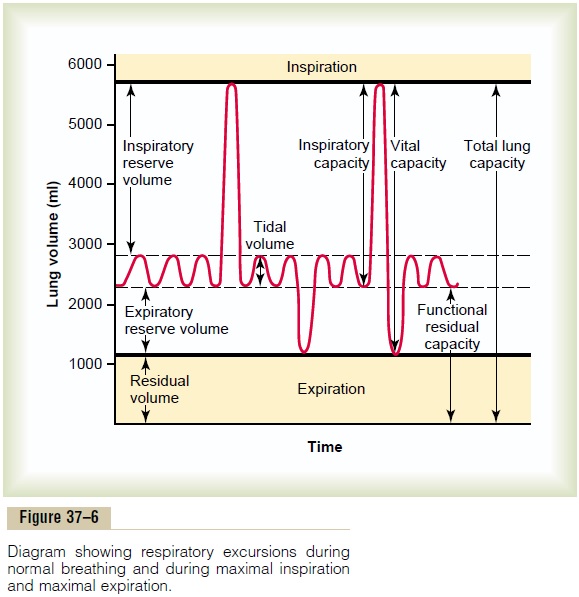
Figure 37–6 shows a spirogram indicating changes in lung volume under different conditions of breathing. For ease in describing the events of pulmonary venti-lation, the air in the lungs has been subdivided in this diagram into four volumes and four capacities, which are the average for a young adult man.
Pulmonary Volumes
To the left in Figure 37–6 are listed four pulmonary lung volumes that, when added together, equal the maximum volume to which the lungs can be expanded.
The significance of each of these volumes is the following:
1. The tidal volume is the volume of air inspired or expired with each normal breath; it amounts to about 500 milliliters in the adult male.
2. The inspiratory reserve volume is the extra volume of air that can be inspired over and above the normal tidal volume when the person inspires with full force; it is usually equal to about 3000 milliliters.
3. The expiratory reserve volume is the maximum extra volume of air that can be expired by forceful expiration after the end of a normal tidal expiration; this normally amounts to about 1100 milliliters.
4. The residual volume is the volume of air remaining in the lungs after the most forceful expiration; this volume averages about 1200 milliliters.
Pulmonary Capacities
In describing events in the pulmonary cycle, it is sometimes desirable to consider two or more of the volumes together. Such combinations are called pul-monary capacities. To the right in Figure 37–6 are listedthe important pulmonary capacities, which can be described as follows:
1. The inspiratory capacity equals the tidal volume plus the inspiratory reserve volume. This is the amount of air (about 3500 milliliters) a person can breathe in, beginning at the normal expiratory level and distending the lungs to the maximum amount.
2. The functional residual capacity equals the expiratory reserve volume plus the residual volume. This is the amount of air that remains inthe lungs at the end of normal expiration (about 2300 milliliters).
3. The vital capacity equals the inspiratory reservevolume plus the tidal volume plus the expiratory reserve volume. This is the maximum amount ofair a person can expel from the lungs after first filling the lungs to their maximum extent and then expiring to the maximum extent (about 4600 milliliters).
4. The total lung capacity is the maximum volume to which the lungs can be expanded with the greatest possible effort (about 5800 milliliters); it is equal to the vital capacity plus the residual volume.
All pulmonary volumes and capacities are about 20 to 25 per cent less in women than in men, and they aregreater in large and athletic people than in small and asthenic people.
Abbreviations and Symbols Used in Pulmonary Function Studies
Spirometry is only one of many measurement proce-dures that the pulmonary physician uses daily. Many of these measurement procedures depend heavily on mathematical computations. To simplify these calcula-tions as well as the presentation of pulmonary function data, a number of abbreviations and symbols have become standardized. The more important of these are given in Table 37–1. Using these symbols, we present here a few simple algebraic exercises showing some of the interrelations among the pulmonary volumes and capacities; the student should think through and verify these interrelations.
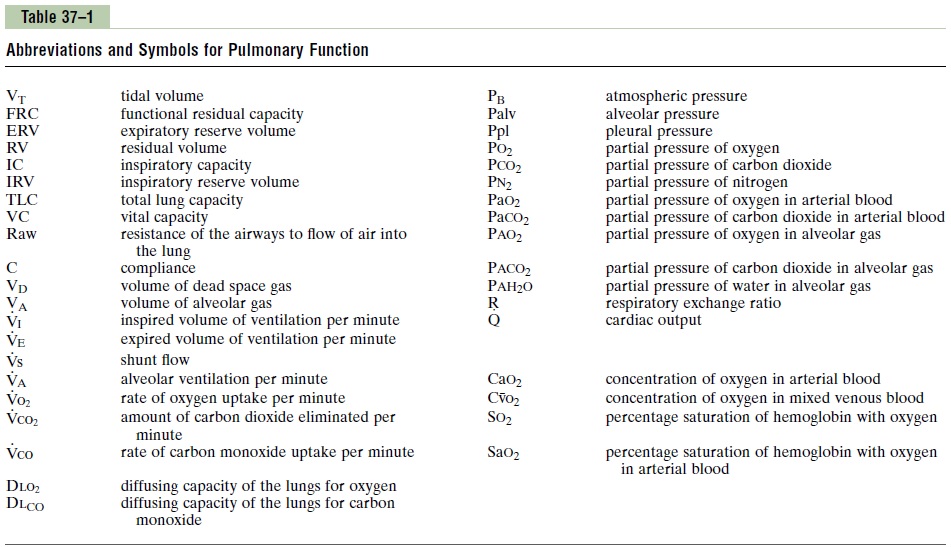
VC = IRV + VT + ERV
VC = IC + ERV
TLC = VC + RV
TLC = IC + FRC
FRC = ERV + RV
Determination of Functional Residual Capacity, Residual Volume, and Total Lung Capacity— Helium Dilution Method
The functional residual capacity (FRC), which is the volume of air that remains in the lungs at the end of each normal expiration, is important to lung function. Because its value changes markedly in some types of pulmonary disease, it is often desirable to measure this capacity. The spirometer cannot be used in a direct way to measure the functional residual capacity, because the air in the residual volume of the lungs cannot be expired into the spirometer, and this volume constitutes about one half of the functional residual capacity. To measure functional residual capacity, the spirometer must be used in an indirect manner, usually by means of a helium dilution method, as follows.
A spirometer of known volume is filled with air mixed with helium at a known concentration. Before breath-ing from the spirometer, the person expires normally. At the end of this expiration, the remaining volume in the lungs is equal to the functional residual capacity. At this point, the subject immediately begins to breathe from the spirometer, and the gases of the spirometer mix with the gases of the lungs. As a result, the helium becomes diluted by the functional residual capacity gases, and the volume of the functional residual capacity can be cal-culated from the degree of dilution of the helium, using the following formula:
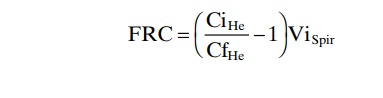
where FRC is functional residual capacity, CiHe is initial concentration of helium in the spirometer, CfHe is final concentration of helium in the spirometer, and ViSpir is initial volume of the spirometer.
Once the FRC has been determined, the residual volume (RV) can be determined by subtracting expira-tory reserve volume (ERV), as measured by normal spirometry, from the FRC. Also, the total lung capacity (TLC) can be determined by adding the inspiratory capacity (IC) to the FRC. That is,
RV = FRC – ERV
and
TLC = FRC + IC
Related Topics