Chapter: Basic & Clinical Pharmacology : Antidepressant Agents
Neuroendocrine Factors in the Pathophysiology of Depression
Neuroendocrine Factors in the
Pathophysiology of Depression
Depression is known to
be associated with a number of hormonal abnormalities. Among the most
replicated of these findings are abnormalities in the HPA axis in patients with
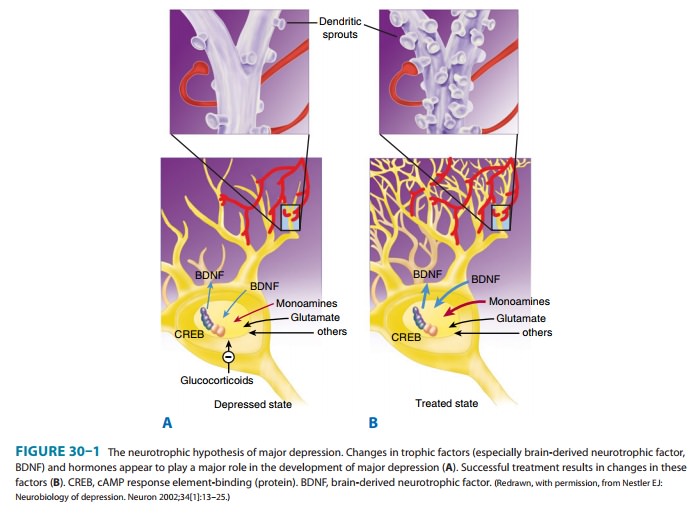
MDD. Moreover, MDD is associated with elevated cortisol levels (Figure 30–1), nonsuppression
of adrenocorticotropic hormone (ACTH) release in the dexamethasone suppression
test, and chronically elevated levels of corticotropin-releasing hormone. The
significance of these HPA abnormalities is unclear, but they are thought to
indicate a dysregu-lation of the stress hormone axis. More severe types of
depression, such as psychotic depression, tend to be associated with HPA
abnor-malities more commonly than milder forms of major depression. It is well known that
both exogenous glucocorticoids and endogenous elevation of cortisol are
associated with mood symptoms and cogni-tive deficits similar to those seen in
MDD.
Thyroid dysregulation
has also been reported in depressed patients. Up to 25% of depressed patients
are reported to have abnormal thyroid function. These include a blunting of
response of thyrotropin to thyrotropin-releasing hormone, and elevations in
circulating thyroxine during depressed states. Clinical hypothyroidism often
presents with depressive symp-toms, which resolve with thyroid hormone
supplementation. Thyroid hormones are also commonly used in conjunction with
standard antidepressants to augment therapeutic effects of the latter.
Finally, sex steroids
are also implicated in the pathophysiology of depression. Estrogen deficiency
states, which occur in the postpartum and postmenopausal periods, are thought
to play a role in the etiology of depression in some women. Likewise, severe
testosterone deficiency in men is sometimes associated with depressive
symptoms. Hormone replacement therapy in hypogonadal men and women may be
associated with an improvement in mood and depressive symptoms.
Related Topics