Chapter: Medical Physiology: Regulation of Extracellular Fluid Osmolarity and Sodium Concentration
Kidneys Excrete Excess Water by Forming a Dilute Urine
The Kidneys Excrete Excess Water by Forming a Dilute Urine
The normal kidney has tremendous capability to vary the relative proportions of solutes and water in the urine in response to various challenges. When there is excess water in the body and body fluid osmolarity is reduced, the kidney can excrete urine with an osmolarity as low as 50 mOsm/L, a concentration that is only about one sixth the osmolarity of normal extracellular fluid. Conversely, when there is a deficit of water and extracellular fluid osmolarity is high, the kidney can excrete urine with a concentration of 1200 to 1400 mOsm/L. Equally important, the kidney can excrete a large volume of dilute urine or a small volume of concentrated urine without major changes in rates of excretion of solutes such as sodium and potassium. This ability to regulate water excretion independently of solute excretion is necessary for survival, especially when fluid intake is limited.
Antidiuretic Hormone Controls Urine Concentration
There is a powerful feedback system for regulating plasma osmolarity and sodium concentration that operates by altering renal excretion of water inde-pendently of the rate of solute excretion. A primary effector of this feedback is antidiuretic hormone (ADH), also called vasopressin.
When osmolarity of the body fluids increases above normal (that is, the solutes in the body fluids become too concentrated), the posterior pituitary gland secretes more ADH, which increases the permeability of the distal tubules and collecting ducts to water. This allows large amounts of water to be reabsorbed and decreases urine volume but does not markedly alter the rate of renal excretion of the solutes.
When there is excess water in the body and extra-cellular fluid osmolarity is reduced, the secretion of ADH by the posterior pituitary decreases, thereby reducing the permeability of the distal tubule and col-lecting ducts to water, which causes large amounts of dilute urine to be excreted. Thus, the rate of ADH secretion determines, to a large extent, whether the kidney excretes a dilute or a concentrated urine.
Renal Mechanisms for Excreting a Dilute Urine
When there is a large excess of water in the body, the kidney can excrete as much as 20 L/day of dilute urine, with a concentration as low as 50 mOsm/L. The kidney performs this impressive feat by continuing to reab-sorb solutes while failing to reabsorb large amounts of water in the distal parts of the nephron, including the late distal tubule and the collecting ducts.
Figure 28–1 shows the approximate renal responses in a human after ingestion of 1 liter of water. Note that urine volume increases to about six times normal within 45 minutes after the water has been drunk.
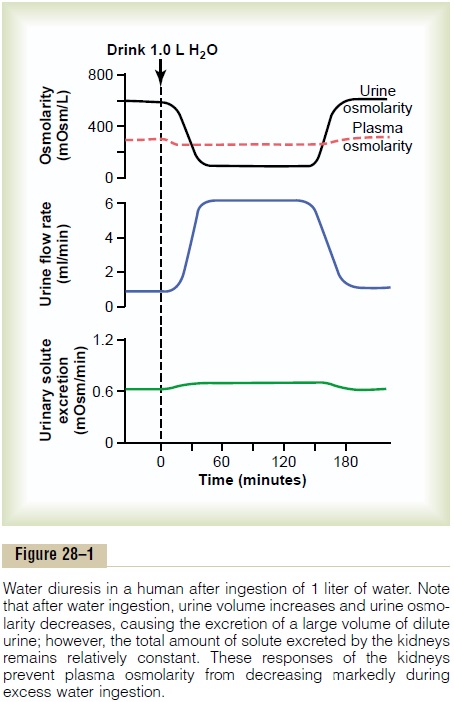
However, the total amount of solute excreted remains relatively constant because the urine formed becomes very dilute and urine osmolarity decreases from 600 to about 100 mOsm/L. Thus, after ingestion of excess water, the kidney rids the body of the excess water but does not excrete excess amounts of solutes.
When the glomerular filtrate is initially formed, its osmolarity is about the same as that of plasma (300 mOsm/L). To excrete excess water, it is necessary to dilute the filtrate as it passes along the tubule. This is achieved by reabsorbing solutes to a greater extent than water, as shown in Figure 28–2, but this occurs only in certain segments of the tubular system as follows.
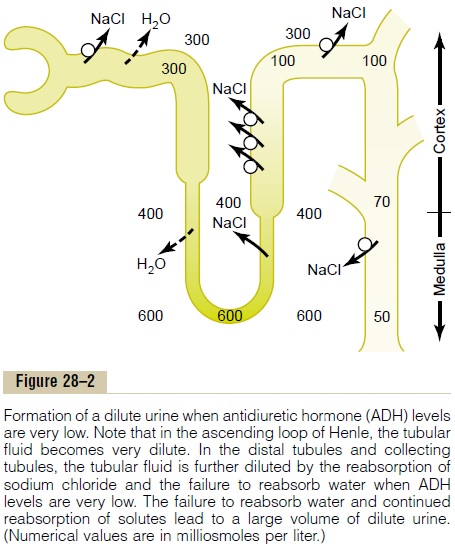
Tubular Fluid Remains Isosmotic in the Proximal Tubule. Asfluid flows through the proximal tubule, solutes and water are reabsorbed in equal proportions, so that little change in osmolarity occurs; that is, the proximal tubule fluid remains isosmotic to the plasma, with an osmolarity of about 300 mOsm/L.As fluid passes down the descending loop of Henle, water is reabsorbed by osmosis and the tubular fluid reaches equilibrium with the surrounding interstitial fluid of the renal medulla, which is very hypertonic—about two to four times the osmolarity of the original glomerular filtrate. There-fore, the tubular fluid becomes more concentrated as it flows into the inner medulla.
Tubular Fluid Becomes Dilute in the Ascending Loop of Henle.
In the ascending limb of the loop of Henle, especially in the thick segment, sodium, potassium, and chloride are avidly reabsorbed. However, this portion of the tubular segment is impermeable to water, even in the presence of large amounts of ADH.
Therefore, the tubular fluid becomes more dilute as it flows up the ascending loop of Henle into the early distal tubule, with the osmolarity decreasing progressively to about 100 mOsm/L by the time the fluid enters the early distal tubular segment. Thus, regardless of whetherADH is present or absent, fluid leaving the early distal tubular segment is hypo-osmotic, with an osmolarity of only about one third the osmolarity of plasma.
Tubular Fluid in Distal and Collecting Tubules Is Further Diluted in the Absence of ADH. As the dilute fluid in the earlydistal tubule passes into the late distal convoluted tubule, cortical collecting duct, and collecting duct, there is additional reabsorption of sodium chloride. In the absence of ADH, this portion of the tubule is also impermeable to water, and the additional reabsorption of solutes causes the tubular fluid to become even more dilute, decreasing its osmolarity to as low as 50 mOsm/L.The failure to reabsorb water and the con-tinued reabsorption of solutes lead to a large volume of dilute urine.
To summarize, the mechanism for forming a dilute urine is to continue reabsorbing solutes from the distal segments of the tubular system while failing to reab-sorb water. In healthy kidneys, fluid leaving the ascending loop of Henle and early distal tubule is always dilute, regardless of the level of ADH. In the absence of ADH, the urine is further diluted in the late distal tubule and collecting ducts, and a large volume of dilute urine is excreted.
Related Topics