Chapter: Medical Physiology: Regulation of Extracellular Fluid Osmolarity and Sodium Concentration
Countercurrent Exchange in the Vasa Recta Preserves Hyperosmolarity of the Renal Medulla
Countercurrent Exchange in the Vasa Recta Preserves Hyperosmolarity of the Renal Medulla
Blood flow must be provided to the renal medulla to supply the metabolic needs of the cells in this part of the kidney. Without a special medullary blood flow system, the solutes pumped into the renal medulla by the countercurrent multiplier system would be rapidly dissipated.
There are two special features of the renal medullary blood flow that contribute to the preserva-tion of the high solute concentrations:
1. The medullary blood flow is low, accounting forless than 5 per cent of the total renal blood flow. This sluggish blood flow is sufficient to supply the metabolic needs of the tissues but helps to minimize solute loss from the medullary interstitium.
2. The vasa recta serve as countercurrent exchangers,minimizing washout of solutes from the medullary interstitium.
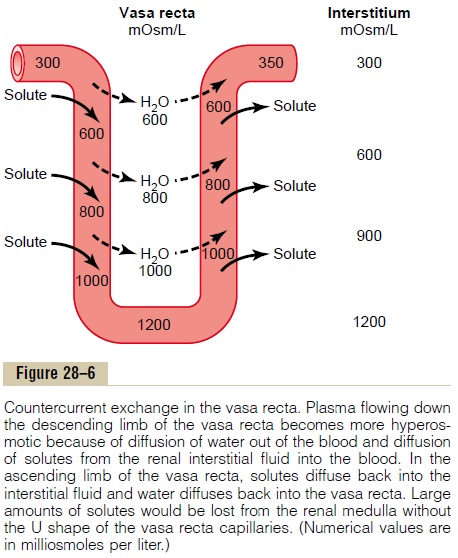
The countercurrent exchange mechanism operates as follows (Figure 28–6): Blood enters and leaves the medulla by way of the vasa recta at the boundary of the cortex and renal medulla. The vasa recta, like other capillaries, are highly permeable to solutes in the blood, except for the plasma proteins. As blood descends into the medulla toward the papillae, it becomes progressively more concentrated, partly by solute entry from the interstitium and partly by loss of water into the interstitium. By the time the blood reaches the tips of the vasa recta, it has a con-centration of about 1200 mOsm/L, the same as that of the medullary interstitium. As blood ascends back toward the cortex, it becomes progressively less concentrated as solutes diffuse back out into the medullary interstitium and as water moves into the vasa recta.
Thus, although there is a large amount of fluid and solute exchange across the vasa recta, there is little net dilution of the concentration of the interstitial fluid at each level of the renal medulla because of the U shape of the vasa recta capillaries, which act as countercur-rent exchangers. Thus, the vasa recta do not create themedullary hyperosmolarity, but they do prevent it from being dissipated.
The U-shaped structure of the vessels minimizes loss of solute from the interstitium but does not prevent the bulk flow of fluid and solutes into the blood through the usual colloid osmotic and hydro-static pressures that favor reabsorption in these capil-laries. Thus, under steady-state conditions, the vasa recta carry away only as much solute and water as is absorbed from the medullary tubules, and the high concentration of solutes established by the counter-current mechanism is maintained.
Increased Medullary Blood Flow Can Reduce Urine Concentrat-ing Ability. Certain vasodilators can markedly increaserenal medullary blood flow, thereby “washing out” some of the solutes from the renal medulla and reduc-ing maximum urine concentrating ability. Large increases in arterial pressure can also increase the blood flow of the renal medulla to a greater extent than in other regions of the kidney and tend to wash out the hyperosmotic interstitium, thereby reducing urine concentrating ability. As discussed earlier, maximum concentrating ability of the kidney is deter-mined not only by the level of ADH but also by the osmolarity of the renal medulla interstitial fluid. Even with maximal levels of ADH, urine concentrating ability will be reduced if medullary blood flow increases enough to reduce the hyperosmolarity in the renal medulla.
Related Topics