Chapter: Essentials of Anatomy and Physiology: The Senses
Eyeball: Layers and Cavities of the Eyeball
EYEBALL
Most of the eyeball is within and protected by the orbit, formed by the lacrimal, maxilla, zygomatic, frontal, sphenoid, and ethmoid bones. The six extrin-sic muscles of the eye (Fig. 9–4) are attached to this bony socket and to the surface of the eyeball. There are four rectus (straight) muscles that move the eyeball up and down or side to side; the name tells you which direction. The medial rectus muscle, for example, pulls the eyeball medially, as if to look at the nose. The two oblique (slanted) muscles rotate the eye. The cra-nial nerves that innervate these muscles are the oculo-motor, trochlear, and abducens (3rd, 4th, and 6th cranial nerves, respectively). The very rapid and com-plex coordination of these muscles in both eyes is, for-tunately, not something we have to think about. The convergence of both eyes on an object is very impor-tant to ensure a single image (that is, to prevent dou-ble vision) and to give us depth perception and a three-dimensional world.
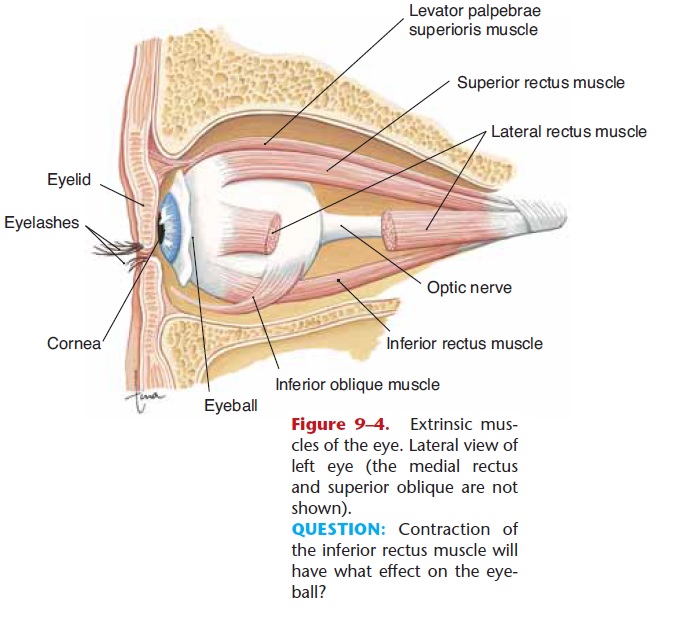
Figure 9–4. Extrinsic mus-cles of the eye. Lateral view of left eye (the medial rectus and superior oblique are not shown).
QUESTION: Contraction of the inferior rectus muscle will have what effect on the eye-ball?
Layers of the Eyeball
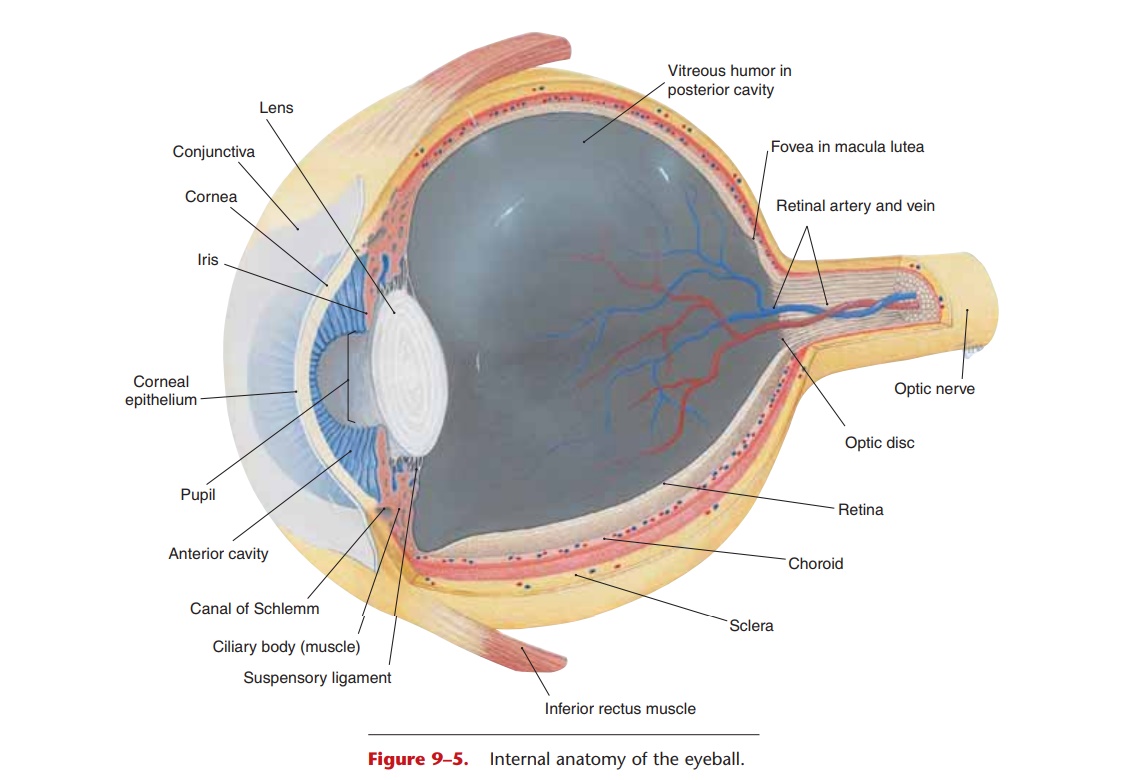
In its wall, the eyeball has three layers: the outer sclera, middle choroid layer, and inner retina (Fig. 9–5). The sclera is the thickest layer and is made of fibrous connective tissue that is visible as the white of the eye. The most anterior portion is the cornea, which differs from the rest of the sclera in that it is transparent. The cornea has no capillaries, covers the iris and pupil inside the eye, and is the first part of the eye that refracts, or bends, light rays.
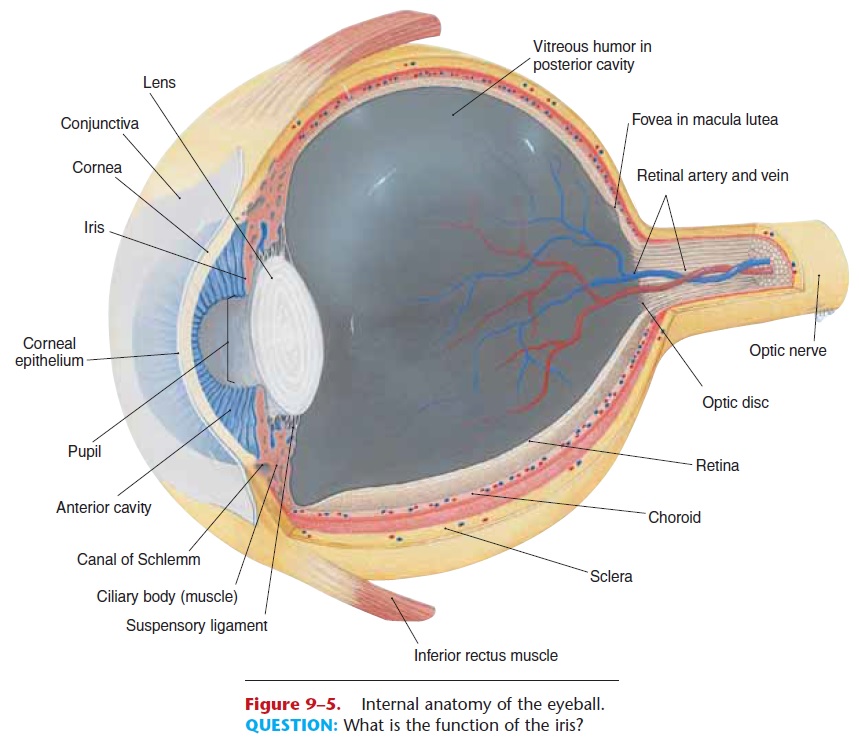
The choroid layer contains blood vessels and a dark blue pigment (derived from melanin) that absorbs light within the eyeball and thereby prevents glare (just as does the black interior of a camera). The anterior portion of the choroid is modified into more specialized structures: the ciliary body and the iris. The ciliary body (muscle) is a circular muscle that surrounds the edge of the lens and is connected to the lens by suspensory ligaments. The lens is made of a transparent, elastic protein, and, like the cornea, has no capillaries. The shape of the lens is changed by the ciliary muscle, which enables the eye to focus light from objects at varying distances from the eye.
Just in front of the lens is the circular iris, the col-ored part of the eye; its pigment is a form of melanin.
What we call “eye color” is the color of the iris and is a genetic characteristic, just as skin color is. Two sets of smooth muscle fibers in the iris change the diame-ter of the pupil, the central opening. Contraction of the radial fibers dilates the pupil; this is a sympathetic response. Contraction of the circular fibers constricts the pupil; this is a parasympathetic response (oculo-motor nerves). Pupillary constriction is a reflex that protects the retina from intense light or that permits more acute near vision, as when reading.
The retina lines the posterior two-thirds of the eyeball and contains the visual receptors, the rods and cones (Fig. 9–6). Rods detect only the presence of light, whereas cones detect colors, which, as you may know from physics, are the different wavelengths of visible light. Rods are proportionally more abundant toward the periphery, or edge, of the retina. Our best vision in dim light or at night, for which we depend on the rods, is at the sides of our visual fields. Cones are most abundant in the center of the retina, espe-cially an area called the macula lutea directly behind the center of the lens on what is called the visual axis. The fovea, which contains only cones, is a small depression in the macula and is the area for best color vision.
An important cause of vision loss for people over 65 years of age is age-related macular degeneration (AMD), that is, loss of central vision, and some cases seem to have a genetic component. In the dry form of AMD, small fatty deposits impair circulation to the macula, and cells die from lack of oxygen. In the wet form of AMD, abnormal blood vessels begin leaking into the retina, and cells in the macula die from the damaging effects of blood outside its vessels. The macula, the center of the visual field, is the part of
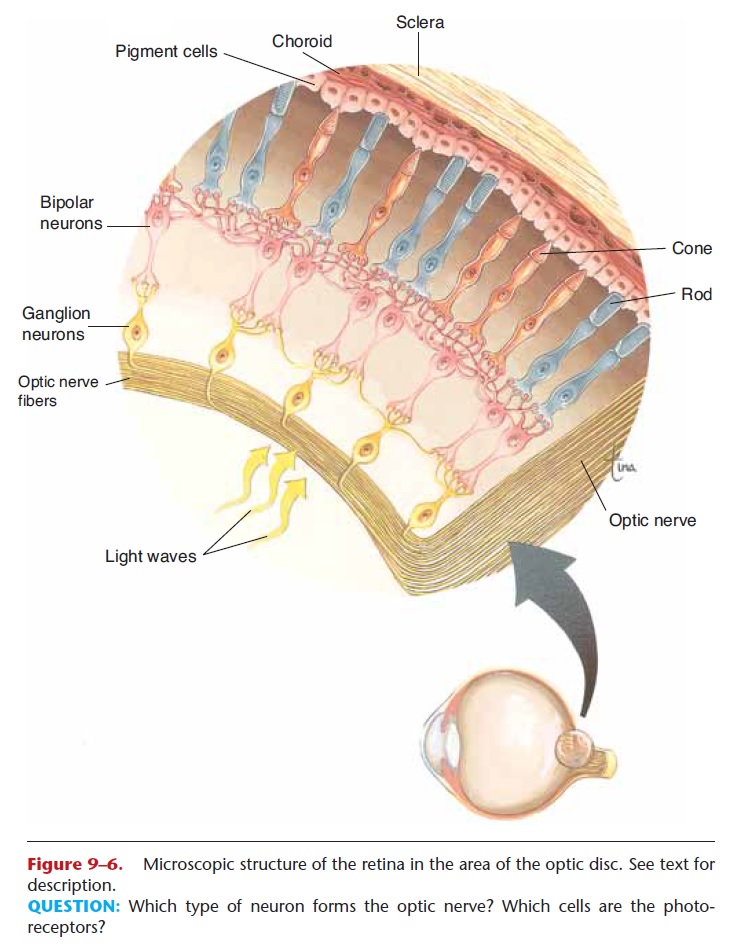
Figure 9–6. Microscopic structure of the retina in the area of the optic disc. See text for description.
When light strikes the retina, the rods and cones generate impulses. These impulses are carried by gan-glion neurons, which all converge at the optic disc(see Figs. 9–5 and 9–6) and pass through the wall of the eyeball as the optic nerve. There are no rods or cones in the optic disc, so this part of the retina is sometimes called the “blind spot.” We are not aware of a blind spot in our field of vision, however, in part because the eyes are constantly moving, and in part because the brain “fills in” the blank spot to create a “complete” picture.
Cavities of the Eyeball
There are two cavities within the eye: the posterior cavity and the anterior cavity. The larger, posterior cavity is found between the lens and retina and con-tains vitreous humor (or vitreous body). This semi-solid substance keeps the retina in place. If the eyeball is punctured and vitreous humor is lost, the retina may fall away from the choroid; this is one possible cause of a detached retina.
The anterior cavity is found between the back of the cornea and the front of the lens, and contains aqueous humor, the tissue fluid of the eyeball. Aqueous humor is formed by capillaries in the ciliary body, flows anteriorly through the pupil, and is reab-sorbed by the canal of Schlemm (small veins also called the scleral venous sinus) at the junction of the iris and cornea. Because aqueous humor is tissue fluid, you would expect it to have a nourishing function, and it does. Recall that the lens and cornea have no capil-laries; they are nourished by the continuous flow of aqueous humor.
Related Topics