Chapter: Ophthalmology: The Ophthalmic Examination
Examination of the Lens
Examination of the Lens
The ophthalmologist uses a slit lamp to examine the lens. The eye can also be examined with a focused light if necessary.
Direct illumination will produce ared
reflection of the fundusif the lens isclearand
gray shadows if lens opacities are
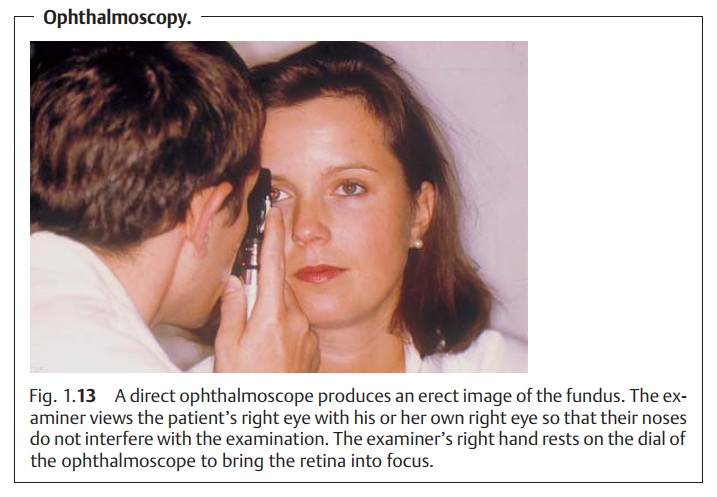
present. The examiner then illuminates the eye laterally with a focused light held as close to the eye as possible
and inspects the eye through a +14 diopter loupe (see Fig. 1.10). This examination permits better
evaluation of changes in the conjunctiva, cornea, and anterior chamber. With
severe opacification of the lens, a gray coloration will be vis-ible in the
pupillary plane. Any such light-scattering opacity is referred to as a
cataract.
Indirect ophthalmoscopy is usually performed
by the ophthalmologist and produces a
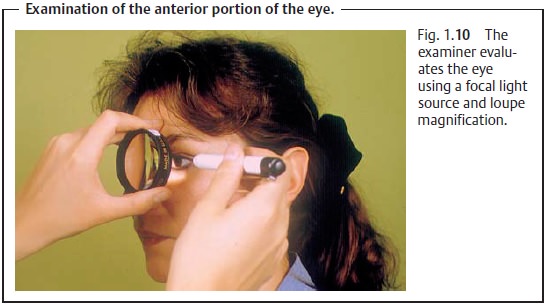
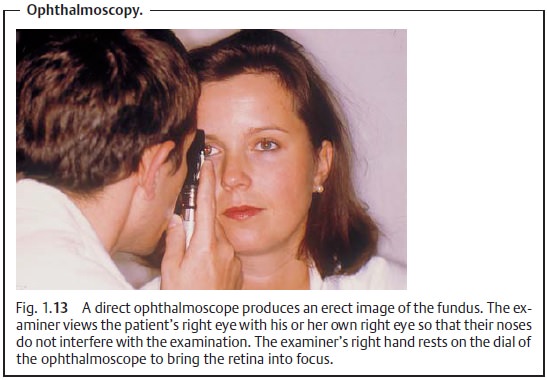
laterally reversed image of the fundus. Less experienced examiners will prefer direct ophthalmoscopy. Here, the oph-thalmoscope is held as close to the patient as
possible (Fig. 1.13; see also Figs. 12.4b and c). Refractive errors in the patient’s eye and the examiner’s eye
are corrected by selecting the ophthalmoscope lens required to bring the retina
into focus. The examiner sees an erect,
16 power magnified image of the ret-ina. The examination should be performed in
a slightly darkened room with the patient’s pupils dilated. Students should be
able to identify the optic disk. In a
normal eye, it is sharply defined structure with vital coloration (i.e.,
yel-lowish orange) at the level of the retina and may have a central
excavation. The central vein lies lateral to the artery; venous diameter is
normally 1.5 times greater than arterial diameter. Each vascular structure
should be of uni-form diameter, and there should be no vascular constriction
where vessels overlap. A spontaneous venous
pulse is normal; an arterial pulse
is abnormal. Younger patients will have a foveal and macular light reflex, and
the retina will have a reddish color (see Fig. 12.8). An ophthalmologist should be con-sulted if
there are any abnormal findings.
Related Topics