Chapter: Clinical Dermatology: Reactive erythemas and vasculitis
Erythema multiforme
Erythema
multiforme
Cause
In erythema multiforme, the victim has usually reacted to an infection, often herpes simplex, or to a drug, but other factors have occasionally been implicated (Table 8.6).

Presentation
The
symptoms of an upper respiratory tract infection may precede the eruption.
Typically, annular non-scaling plaques appear on the palms, soles, forearms and
legs. They may be slightly more purple than the wheals of ordinary urticaria.
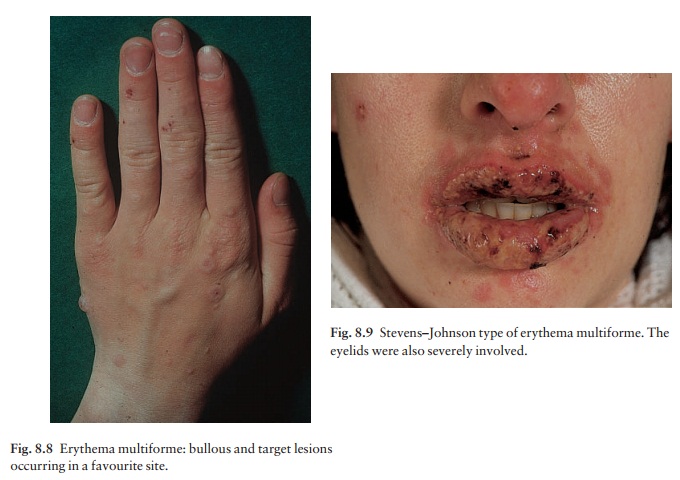
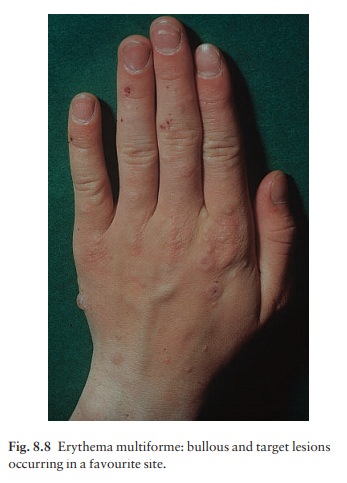
Individual lesions enlarge but clear centrally. A new lesion may begin at the
same site as the original one, so that the two concentric plaques look like a
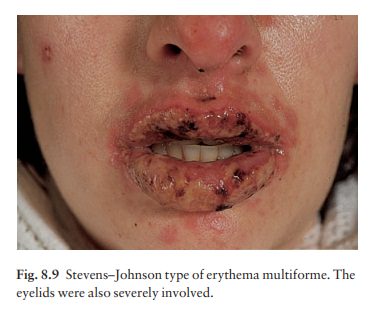
target (Fig. 8.8). Some lesions blister. The Stevens–Johnson syndrome is a
severe vari-ant of erythema multiforme associated with fever and mucous
membrane lesions. The oral mucosa, lips and bulbar conjunctivae are most
commonly affected, but the nares, penis, vagina, pharynx, larynx and
tracheo-bronchial tree may also be involved (Fig. 8.9).
Course
Crops of new lesions appear for 1 or 2 weeks, or until the responsible drug or other factor has been eliminated. Individual lesions last several days, and this differentiates them from the more fleeting lesions of an annular urticaria. The site of resolved lesions is marked transiently by hyperpigmentation, particu-larly in pigmented individuals. A recurrent variant of erythema multiforme exists, characterized by repeated attacks; this merges with a rare form in which lesions continue to develop over a prolonged period, even for years.
Complications
There
are usually no complications. However, severe lesions in the tracheo-bronchial
tree of patients with Stevens–Johnson syndrome can lead to asphyxia, and ulcers
of the bulbar conjunctiva to blindness. Corneal ulcers, anterior uveitis and
panophthalmitis may also occur. Genital ulcers can cause urinary retention, and
phimosis or vaginal stricture after they heal.
Differential diagnosis
Erythema
multiforme can mimic the annular variant of urticaria as described above.
However, target lesions are pathognomonic of erythema multiforme. Its acral
distribution, the way individual lesions last for more than 24 h, their purple
colour and the involvement of mucous membranes all help to identify erythema
multiforme. Other bullous disorders may enter the differential diagnosis .
Investigations
The
histology of erythema multiforme is distinctive. Its main features are
epidermal necrosis and dermal changes, consisting of endothelial swelling, a
mixed lymphohistiocytic perivascular infiltrate and papil-lary dermal oedema.
The abnormalities may be pre-dominantly epidermal or dermal, or a combination
of both; they probably depend on the age of the lesion biopsied.
Most
investigations are directed towards identifying a cause. A careful history
helps rule out a drug reac-tion. Tzanck smears culture of suspicious prodromal
vesicles may identify a precipitating herpes simplex infection, which usually
is almost healed by the time the erythema multiforme erupts. A chest X-ray and
serological tests should identify mycoplasmal pneumonia. A search for other
infectious agents, neoplasia, endocrine causes or collagen disease is sometimes
necessary, especially when the course is prolonged or recurrent. About 50% of
cases have no demonstrable provoking factor.
Treatment
The
best treatment for erythema multiforme is to identify and remove its cause. In
mild cases, only symp-tomatic treatment is needed and this includes the use of
antihistamines.
The
Stevens–Johnson syndrome, on the other hand, may demand immediate consultation
between derma-tologists and specialists in other fields such as ophthal-mology,
urology and infectious diseases, depending on the particular case. Intravenous
infusions of human gammaglobulin seem to be worthwhile. The use of systemic
steroids to abort Stevens–Johnson syndrome is debatable, but many believe that
a short course (e.g. prednisolone 80 mg/day in divided doses in an adult) helps.
However, the dose should be tapered rapidly or stopped because prolonged
treatment in the Stevens– Johnson syndrome has been linked, controversially,
with a high complication rate. Good nursing care with attention to the mouth
and eyes is essential. The prevention of secondary infection, maintenance of a
patent airway, good nutrition, and proper fluid and electrolyte balance are
important.
Herpes
simplex infections should be suspected in recurrent or continuous erythema
multiforme of oth-erwise unknown cause. Treatment with oral acyclovir 200 mg
three to five times daily or valciclovir 500 mg twice daily may prevent attacks, both of herpes simplex
and of the recurrent erythema multiforme which follows it.
Related Topics