Chapter: Essentials of Psychiatry: Eating Disorders
Eating Disorders
Eating Disorders
In the
current psychiatric nomenclature of the Diagnostic
and Statistical Manual of Mental
Disorders, Fourth Edition (DSM-IV-TR), the eating disorders consist of two
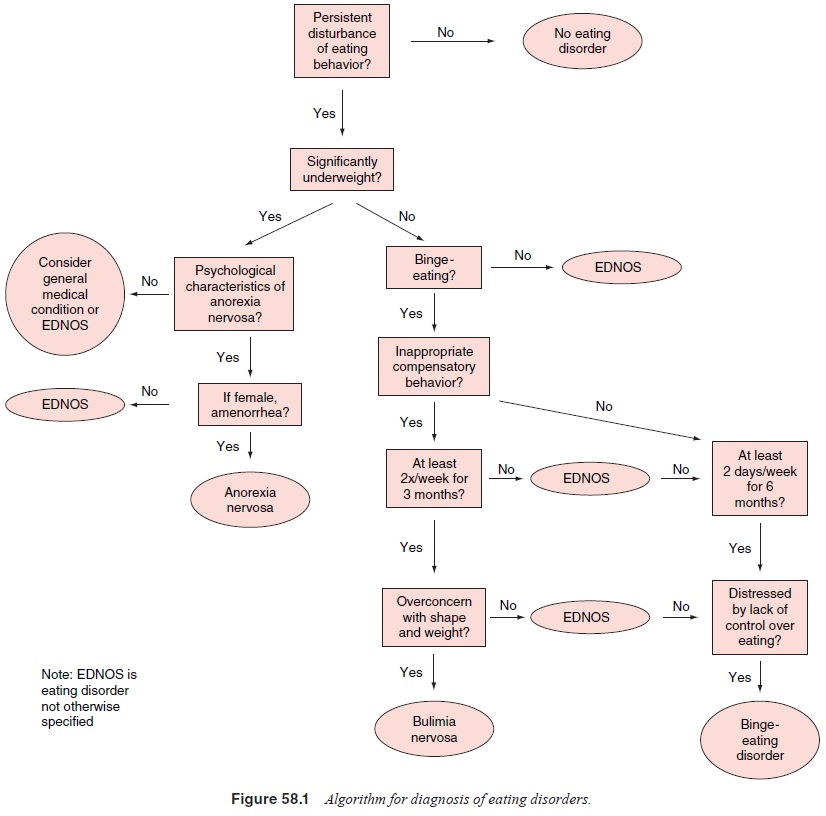
clearly defined syndromes: anorexia nervosa and bulimia nervosa. Many
individuals present-ing for treatment of an eating disorder (Figure 58.1) fail
to meet formal criteria for either anorexia nervosa or bulimia nervosa, which
raises an important theoretical and practical question: What is an eating
disorder? Although this topic has received surprisingly little attention, it
has been suggested that a working definition of an eating disorder might be “a
persistent disturbance of eating be-havior or behavior intended to control
weight, which significantly impairs physical health or psychosocial
functioning” (Fairburn and Walsh, 2002). This definition clearly encompasses
the recog-nized disorders, anorexia nervosa and bulimia nervosa. In addi-tion,
it provides a basis for viewing eating disorders as clinically significant
problems that do not meet criteria for anorexia nervosa or bulimia nervosa. The
term atypical eating disorder is often ap-plied to such problems, even though
the number of individuals suf-fering from them may well outnumber those with
“typical” eating disorders. One example of an atypical eating disorder is that
of women who are overly concerned about their weight, have dieted to a
below-normal weight, but have not ceased menstruating and, therefore, do not
meet full criteria for anorexia nervosa. Another is that of individuals who
binge and vomit regularly, but at less than the twice-a-week frequency required
for bulimia nervosa.
An
additional example of a clinically important atypical eating disorder is the
occurrence of frequent binge-eating that is not followed by the self-induced
vomiting or other inappropri-ate attempts to compensate that are characteristic
of bulimia ner-vosa. This disturbance, for which the name binge-eating disorder
has been proposed (DSM-IV appendix B) is a common behavio-ral pattern among
obese individuals who present for treatment at weight loss clinics.
At
present, obesity is not considered an eating disorder. Obesity refers to an
excess of body fat and is viewed as a general medical, not a psychiatric,
condition. At this stage of our knowl-edge, obesity is conceived as an
etiologically heterogeneous condi-tion. Obese individuals are at increased risk
for a number of serious medical problems and are subject to significant social
stigmatiza-tion and its psychological sequelae. However, the widely held
as-sumption that obesity is the result of a psychiatric disorder in which
eating is used as a coping mechanism for depression or anxiety has not been
substantiated by empirical research. Studies of obese and normal-weight subjects
from the general (nonpatient) population have found no more psychiatric
disturbance in those who are over-weight than in those who are of normal
weight.. Therefore, it seems appropriate at present to describe as having an
eating disorder onlythose obese individuals who manifest a clear behavioral
abnormal-ity that impairs health or psychosocial functioning.
Related Topics