Chapter: Medical Surgical Nursing: Critical Thinking,Ethical Decision Making, and the Nursing Process
Diagnosis - Using the Nursing Process
DIAGNOSIS
The assessment component
of the nursing process serves as the basis for identifying nursing diagnoses
and collaborative prob-lems. Soon after the completion of the health history
and the physical assessment, the nurse organizes, analyzes, synthesizes, and
summarizes the data collected and determines the patient’s need for nursing care.
Nursing Diagnosis
Nursing, unlike
medicine, does not yet have a complete taxon-omy, or classification system, of
diagnostic labels. Classification of discrete items into meaningful categories
organizes components of knowledge into coherent units of related information.
Some rea-sons for establishing taxonomies are to help identify what is known
about a field of study, to discover what gaps in knowledge exist, to provide a
common language that enhances communica-tion among colleagues, and to facilitate
the coding of standardized information for use in databases. Nursing diagnoses,
the first tax-onomy created in nursing, have fostered the development of
autonomy and accountability in nursing and have helped to de-lineate the scope
of practice. Many state nurse practice acts include nursing diagnosis as a
nursing function, and nursing diagnosis is included in the ANA’s Standards of Clinical Nursing Practice
and the standards of many nursing specialty organizations.
The official
organization that has assumed responsibility for de-veloping the taxonomy of
nursing diagnoses and formulating nursing diagnoses acceptable for study is the
North American Nursing Diagnosis Association (NANDA). NANDA has grouped
diagnoses according to patterns of human responses (Chart 3-7). The diagnostic
labels identified by NANDA have been generally accepted but require further
validation, refinement, and expansion based on clinical use and research; they
are not yet complete or mutually exclusive, and more investigation is needed to
determine their validity and clinical applicability.


Choosing a Nursing Diagnosis
When choosing the
nursing diagnoses for a particular patient, the nurse must first identify the
commonalities among the assessment data collected. These common features lead
to the categorization of related data that reveal the existence of a problem
and the need for nursing intervention. The patient’s identified problems are
then defined in the nursing diagnoses. The most commonly selected nursing
diagnoses are compiled and categorized by NANDA in a taxonomy that is updated
at least every 2 years. It is important to remember that nursing diagnoses are
not medical diagnoses; they are not medical treatments prescribed by the
physician; and they are not diagnostic studies. Nursing diagnoses are not the
equip-ment used to implement medical therapy, and they are not the problems
that the nurse experiences while caring for the patient. They are the patient’s
actual or potential health problems that in-dependent nursing actions can
resolve. Nursing diagnoses that are succinctly stated in terms of the specific
problems of the patient will guide the nurse in the development of the nursing
plan of care.
To give additional
meaning to the diagnosis, the characteristics and the etiology of the problem
must be identified and included as part of the diagnosis. For example, the
nursing diagnoses and their defining characteristics and etiology for a patient
who has rheumatoid arthritis may include
· Impaired physical
mobility related to pain and stiffness with joint movement
· Self-care deficits
(bathing/hygiene, dressing/grooming, feed-ing, toileting) related to fatigue
and joint stiffness
· Low self-esteem
(chronic, situational, risk for situational) related to loss of independence
·
Imbalanced nutrition: Less than body requirements
related to fatigue and inadequate food intake
Collaborative Problems
In addition to nursing
diagnoses and their related nursing inter-ventions, nursing practice involves
certain situations and inter-ventions that do not fall within the definition of
nursing diagnoses. These activities pertain to potential problems or
complications that are medical in origin and require collaborative
interventions with the physician and other members of the health care team. The
term collaborative problem is used to
identify these situations.
Collaborative problems
are certain physiologic complications that nurses monitor to detect changes in
status or onset of com-plications. Nurses manage collaborative problems using
physician-prescribed and nursing-prescribed interventions to minimize
complications. A primary focus of the nurse when treating collaborative
problems is monitoring the pa-tient for the onset of complications or changes
in the status of ex-isting complications. The complications are usually related
to the patient’s disease process, treatments, medications, or diagnostic
studies. The nurse prescribes nursing interventions that are ap-propriate for
managing the complications and implements the treatments prescribed by the
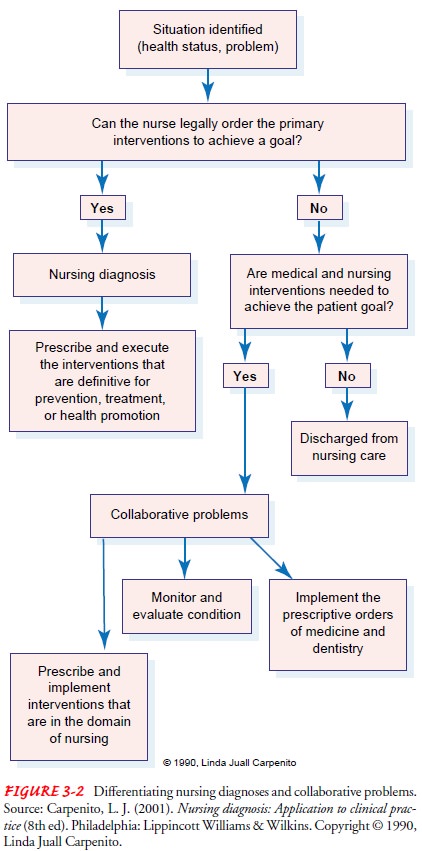
physician. Figure 3-2 depicts the dif-ferences between nursing diagnoses and
collaborative problems. After the nursing diagnoses and collaborative problems
have been identified, they are recorded on the plan of nursing care.
Related Topics