Chapter: Medicine and surgery: Gastrointestinal system
Crohn’s disease - Disorders of the large bowel and inflammatory bowel disease
Crohn’s disease
Definition
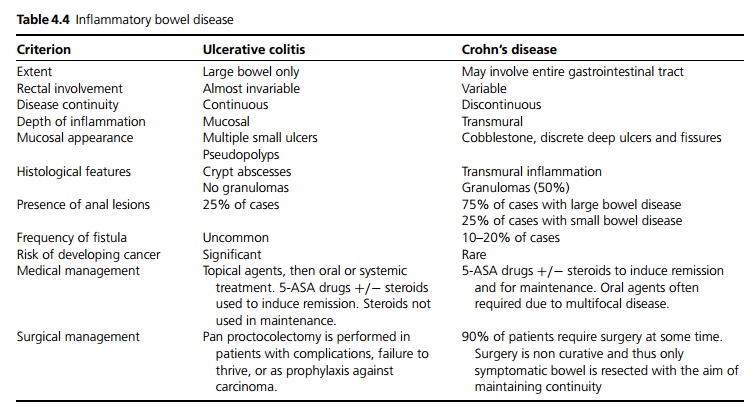
A chronic granulomatous inflammatory bowel disease (IBD), which may affect the whole bowel (see Table 4.4).
Incidence
5–6 per 100,000 per year.
Age
Peak incidence 20–50 years.
Sex
M = F
Geography
Incidence varies from country to country, most common in the West.
Aetiology
1. Familial: There is significant concordance between monozygotic twins. Crohn’s disease is more common in relatives of patients.
2. Genetic: HLA B27 is more common in patients with IBD. A specific susceptibility gene for Crohn’s disease has been found on chromosome 16, IBD1. This encodes a protein, NOD2, which regulates macrophage activation in response to intracellular lipopolysaccharide.
3. Smoking: Patients with Crohn’s disease are more likely to be tobacco smokers.
4. Some suggestion of infective trigger, but no clear evidence.
Pathophysiology
Crohn’s disease is a chronic relapsing and remitting inflammatory disease that can affect any part of the gastrointestinal tract. The site most commonly affected is the terminal ileum. The disease may affect a small area of the bowel or may be extensive affecting the whole bowel. Multiple areas may be affected with normal bowel inbetween termed ‘skip lesions’.
Clinical features
The clinical picture is dependent on the area affected. Colonic disease presents with passage of blood and mucus, terminal ileal disease often presents with diarrhoea, abdominal pain and weight loss. Abdominal pain is variable from chronic to acute, and may occur in any part of the abdomen. It may mimic other pathologies such as intestinal obstruction or acute appendicitis. Specific features to be elucidated include oral or perianal ulcer- ation, joint pain and swelling, rashes such as erythema nodosum, and signs of iritis.
Macroscopy
In early disease there is oedema of the mucosa and submucosa resulting in a loss of transverse folds. Later in the course there is a cobblestone effect due to submucosal oedema and deep fissured ulcers. Bowel wall thickening and strictures result from oedema and fibrosis. These areas are interspersed by normal areas of bowel.
Microscopy
Transmural (full thickness) inflammatory cell infiltrates are seen. Ulcers extend deep within the bowel wall, fissures and fibrous scars are also seen. Non-caesating granulomas in the presence of mucosal changes of inflammatory bowel disease are characteristic and diagnostic of Crohn’s disease.
Complications
Fibrosis and scarring leads to stricture formation and intestinal obstruction. Inflammation of the serosal surface may cause adhesions and intestinal obstruction. Transmural inflammation may lead to fisulae, perforation and abscess formation. In long-standing disease there is an increased incidence of carcinoma of the bowel.
Investigations
Anaemia may be due to chronic disease, iron deficiency or vitamin B12 or folate deficiency. The platelet count may be raised in active disease.
Inflammatory markers such as C reactive protein and ESR may be raised.
A small bowel contrast follow through may reveal deep ulceration and areas of narrowing (sting sign). Strictures are also demonstrated.
Colonosocopy with biopsy is diagnostic. Capsular endoscopy can be used to visualise the small bowel.
Other investigations include a white cell scan to identify areas of active inflammation and MRI scanning for perianal disease.
Management
Symptomatic treatment includes anti-diarrhoeal agents such as loperamide or codeine phosphate. Anaemia is supported with ferrous sulphate.
Acute exacerbations:
· Induction of remission. Mild cases may be treated initially with 5-aminosalicylic acid (5-ASA) drugs such as mesalazine. The next step is often antibiotics in ileitis or colitis (usually ciprofloxacin and metronidazole) – these may work by reducing inflammation due to infection, or transmigration of bacteria through the gut wall. Moderate or severe cases require corticosteroids which may be given as enemas in colonic disease or orally/parenterally, often in combination with 5-ASA drugs and antibiotics. Steroids are withdrawn following induction of remission, but relapse may occur.
· Maintenance of remission – apart from 5-ASA drugs, steroidsparing agents such as azathioprine and 6-mercaptopurine may be used to allow the reduction and withdrawal of steroid dose. Azathioprine requires careful monitoring as it may cause bone marrow suppression particularly in TPMT deficient patients (see above) or abnormal liver function tests.
· Infliximab (a monoclonal antibody directed against tumour necrosis factor alpha –TNFα) is used in moderate to severe Crohn’s disease, particularly for fistulising Crohn’s.
· Elemental and polymeric diets may be used, particularly in children.
Surgical: 80–90% of patients will require some form of surgical intervention during their lifetime. Surgery may be required for complications or if there is failure of medical treatment and severe symptoms. The procedure involves resection of affected bowel; however, poor wound healing may lead to fistulas, so surgery is avoided if possible.
Prognosis
The condition runs a course of relapses and remissions. Virtually all patients will have a significant relapse within 20 years. Mortality is twice that of the general population, operative mortality of 5%. The risk of malignancy is 2–3% (slightly higher than the general population).
Related Topics